| |
High efficacy of switching to bictegravir/emtricitabine/tenofovir
alafenamide in people with suppressed HIV and preexisting M184V/I
|
| |
| |
Download the PDF here
Download the PDF here
AIDS: September 01, 2022
Abstract
Objective:
We investigated the prevalence of preexisting M184V/I and associated risk factors among clinical trial participants with suppressed HIV and evaluated the impact of M184V/I on virologic response after switching to bictegravir/emtricitabine/tenofovir alafenamide (B/F/TAF).
Design:
Participant data were pooled from six clinical trials investigating the safety and efficacy of switching to B/F/TAF in virologically suppressed people with HIV.
Methods:
Preexisting drug resistance was assessed by historical genotypes and/or baseline proviral DNA genotyping. Virologic outcomes were determined by last available on-treatment HIV-1 RNA. Stepwise selection identified potential risk factors for M184V/I in a multivariate logistic regression model.
Results:
Altogether, 2034 participants switched treatment regimens to B/F/TAF and had follow-up HIV-1 RNA data, and 1825 of these participants had baseline genotypic data available. Preexisting M184V/I was identified in 182 (10%), mostly by baseline proviral DNA genotype (n = 167). Most substitutions were M184V (n = 161) or M184V/I mixtures (n = 10). Other resistance substitutions were often detected in addition to M184V/I (n = 147). At last on-treatment visit, 98% (179/182) with preexisting M184V/I and 99% (2012/2034) of all B/F/TAF-treated participants had HIV-1 RNA less than 50 copies/ml, with no treatment-emergent resistance to B/F/TAF. Among adult participants, factors associated with preexisting M184V/I included other resistance, black race, Hispanic/Latinx ethnicity, lower baseline CD4+ cell count, advanced HIV disease, longer duration of antiretroviral therapy, and greater number of prior third agents.
Conclusion:
M184V/I was detected in 10% of virologically suppressed clinical trial participants at study baseline. Switching to B/F/TAF demonstrated durable efficacy in maintaining viral suppression, including in those with preexisting M184V/I.
Outcomes on bictegravir/emtricitabine/tenofovir in participants with preexisting M184V/I (bictegravir/emtricitabine/tenofovir, M184V/I n = 182)
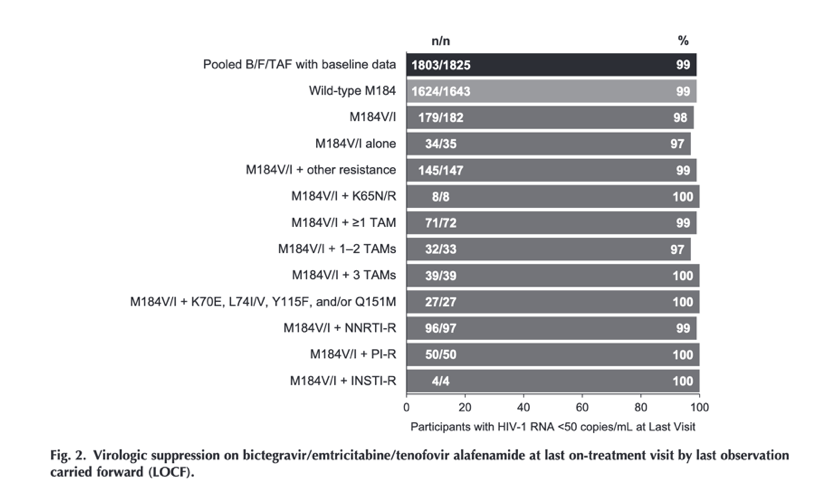
The 182 participants with preexisting M184V/I received B/F/TAF for a median duration of 69 weeks (IQR 50–96). By M = E analysis, the proportion of participants with HIV-1 RNA less than 50 copies/ml ranged from 98 to 100% at all study visits through a maximum of 180 weeks after B/F/TAF switch (Fig. 1b). At last on-treatment visit, 98% (179/182) with M184V/I had HIV-1 RNA less than 50 copies/ml compared with 99% (1803/1825) of those with baseline data and 99% (1624/1643) of those with wild-type M184 (P = 0.49 and 0.48, respectively, by Fisher's exact test) (Fig. 2). When analyzed by the presence of M184V/I alone or in combination with other resistance substitutions, virologic suppression at last visit ranged from 97 to 100%. All 12 participants with M184V/I and K65R or primary INSTI resistance were suppressed at last visit. When analyzed by M184V/I detection type, 98% (164/167) with BL-DNA M184V/I detection and 100% (38/38) with historical M184V/I were virally suppressed at last visit.
Three participants with preexisting M184V/I from study 1878 (switch from boosted PI with two NRTIs) had HIV-1 RNA greater than 50 copies/ml at their last study visit while receiving B/F/TAF. Two had preexisting M184V with another resistance substitution (K70R or K103N) and one had an M184V/I mixture only. All three cases of M184V/I were detected by BL-DNA genotyping. Two participants had HIV-1 RNA less than 100 copies/ml at last visit, which did not meet resistance testing criteria: the participant with M184V and K103N virologically suppressed to HIV-1 RNA less than 50 copies/ml on commercial B/F/TAF and the participant with M184V/I suppressed on a regimen of ritonavir-boosted atazanavir with FTC/TDF. The third participant who had M184V and K70R experienced confirmed virologic failure with HIV-1 RNA 2860 copies/ml after documented poor adherence and undetectable plasma bictegravir levels; there were no new resistance substitutions. This participant subsequently switched regimens to rilpivirine with cobicistat-boosted darunavir and achieved virologic suppression.
|
|
| |
| |
|
|
|