| |
Prevalence and risk factors for falls and fall-related injuries in the 2018 National Post-acute and Long-term Care Study (25%) & for PLWH
|
| |
| |
Download the PDF here
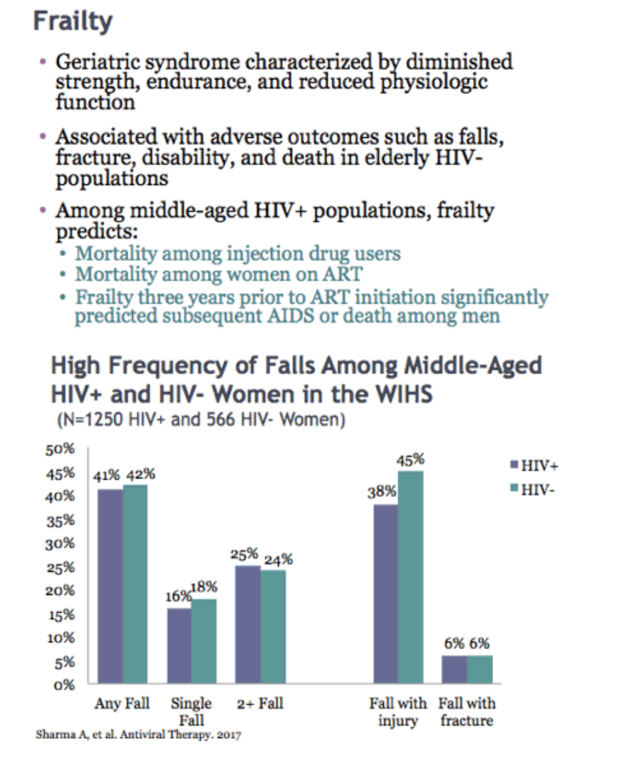
Frailty Predicts Recurrent but Not Single Falls 10 Years Later in HIV+ and HIV- Women
25% of HIV+ middle aged women in WIHS (36-48) experienced 2+ falls in WIHS
Detectable viral load quadruples odds of recurrent falls in older men with HIV
About 10% of recorded falls led to injury and almost 5% caused fracture.
Multivariate analysis did not link HIV infection to higher odds of falling, but 3 variables emerged as independent predictors of falling in the combined HIV-positive and negative group: taking diabetes drugs, peripheral neuropathy, and illicit drug use. Five variables independently predicted recurrent falls in the combined HIV-positive and negative group: taking diabetes drugs, taking antidepressants, peripheral neuropathy, illicit drug use, and every additional 5 years of age.
Among men with HIV, a detectable viral load (versus an undetectable load) independently predicted 4-fold higher odds of recurrent falls. Four other variables independently predicted recurrent falls: efavirenz use (about 4-fold higher odds), taking diabetes drugs (about 4-fold higher odds), peripheral neuropathy (about 2-fold higher odds), and illicit drug use (about 2-fold higher odds).
The researchers suggested their findings support fall prevention through physical activity, antiretroviral adherence, transition to nonefavirenz regimens, and counseling about pets, curbs, and other physical hazards.
Risk Factors for Falls in HIV-Infected Persons
The odds of falling increased 1.7 for each comorbidity and 1.4 for each medication (P <0.001) and were higher in persons with
cardiovascular disease, hypertension, dementia, neuropathy, arthritis, chronic pain, psychiatric disease, frailty, or disability [all odds ratio (OR) >/= 1.8; P /= 2.7; P
Frailty and the Risk of Falls in HIV-Infected Older Adults in the ACTG A5322 Study

Frailty predicts recurrent falls among older women with and without HIV
Frailty, physical function impairment, comorbidity burden, and falls are predictive of mortality among middle-aged adults with HIV
Two or More Anticholinergics Tied to Falls, Frailty in People With HIV
The evidence suggests that exercise based and tailored interventions are the most effective way to reduce falls and associated healthcare costs among older people in the community.
------------------------------------------------
Prevalence and risk factors for falls and fall-related injuries in the 2018 National Post-acute and Long-term Care Study
30 August 2022
In this nationally representative cross-sectional study, we found that over one-quarter of RCC residents sustained a fall in the past 90 days, of which over one-third resulted in injury. Our study contributes to the epidemiology of falls in the long-term care setting in recent years. While it is well-known that approximately one-third of community-dwelling older adults report a fall each year, less is known about fall prevalence in long-term care.5, 6 Falls often have serious consequences, especially in frail older residents. Moreover, fall-related injuries reduce the ability to function normally and our analysis shows over 3-fold increased risk of ED visits or hospitalization.
We found that functional and cognitive impairment, multimorbidity, and antipsychotic use increased the likelihood of falls and fall-related injuries. Therefore, appropriate management of these acute and chronic conditions, including reducing inappropriate medication use, is a critical aspect of effective falls prevention.7-9
In conclusion, our analysis suggests a high national prevalence of falls and fall-related injuries in US RCCs, with over one-quarter of residents having a fall in the past 90 days. In addition, dependence in daily activities and cognitive impairment were key risk factors for falls.
Falls and related injuries are common and cause significant morbidity and mortality in older adults living in long-term care settings.1 However, prior epidemiological estimates of falls in this setting are nearly 30 years old and not nationally representative.2 Contemporary representative data are needed to inform research and policy related to falls. Thus, we evaluated the prevalence and characteristics associated with falls and fall-related injuries using a nationally representative sample of residential care community (RCC) residents in the United States.
This study used publicly available data at the resident level from the National Post-acute and Long-term Care Study (NPLTCS), conducted by the National Center for Health Statistics in the US. The NPLTCS draws from a random sample of licensed RCCs in each of the 50 states and the District of Columbia. To be eligible, RCCs had to be state regulated; have four or more beds; provide room, board and meals, 24-hour on-site supervision, and help with personal care or health-related services. RCCs exclusively serving mentally ill, intellectually or developmentally disabled populations were excluded. Two residents were randomly selected from eligible RCCs that agreed to participate. The questionnaire was directed to the administrator at the RCC and conducted via computer-assisted telephone interviews.3 In this cross-sectional analysis, we used the 2018 survey (conducted between July 2018 and February 2019), including 904 residents from 419 RCCs.3 Survey weights were applied to yield national estimates for RCCs in the US population.4
RESULTS
After excluding residents with missing values for falls, the final sample included 876 RCC residents, representing a national sample of 895,068 residents. Table 1 describes the sample characteristics overall and by fall status, with mean age of 83.3 years. The prevalence of falls during the past 90 days at the RCC was 26.4%.
The occurrence of falls did not differ by sex, race, use of Medicaid, visual impairment, or number of comorbidities. However, a greater proportion of those with falls were prescribed polypharmacy ≥9 medications, dependent per the Katz Index of Independence in Activities of Daily Living (Katz ADL score), requiring a walking aid, or having impaired cognitive function. Additionally, those who fell had a marginally higher proportion of hospital overnight stays or emergency department (ED) visits or had aggressive verbal or behavioral symptoms. Among those who had fallen, 36.4% had fall-related injuries.
Those who were dependent or partially dependent, measured by the Katz ADL score, had approximately 3.5- and 4.0-fold increased odds of falling, respectively, than those who were independent in daily living. For fall-related injuries, those who were Black residents (OR: 2.07; 95% CI: 1.39, 7.89), with cognitive impairment (OR: 3.88; 95% CI: 1.73, 8.84), experienced a hospital overnight stay or ED visit in the past 12 months (OR: 1.23; 95% CI: 1.82, 7.02), or had 2–5 comorbidities (OR: 3.00; 95% CI: 1.11, 8.11) were more likely to have fall-related injuries.
Subgroup analysis among those with dementia (n = 280, representing 247,021 residents) showed that taking antipsychotics increased the odds of falls more than twofold than those not taking antipsychotics (OR: 2.33; 95% CI: 1.11, 4.90).
|
|
| |
| |
|
|
|