 |
 |
 |
| |
Risk factors linked to age-related comorbidities among people living with HIV aged over 40 years
|
| |
| |
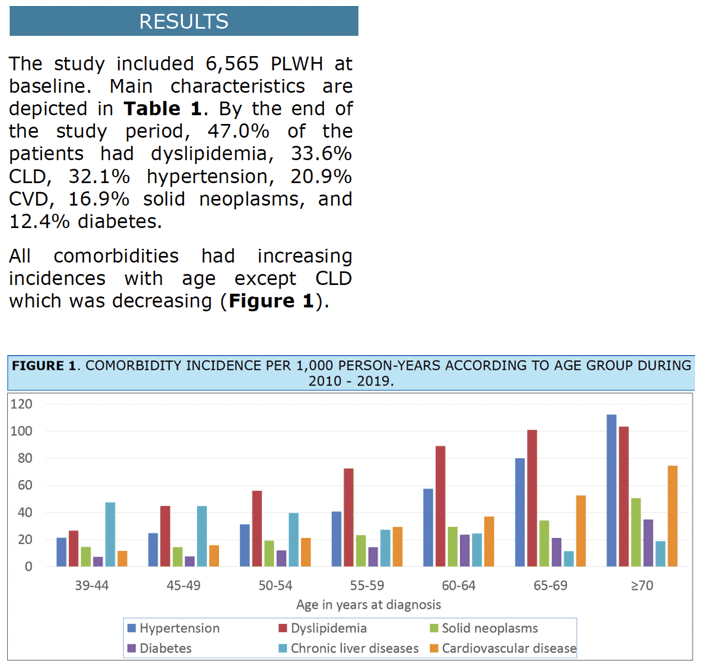
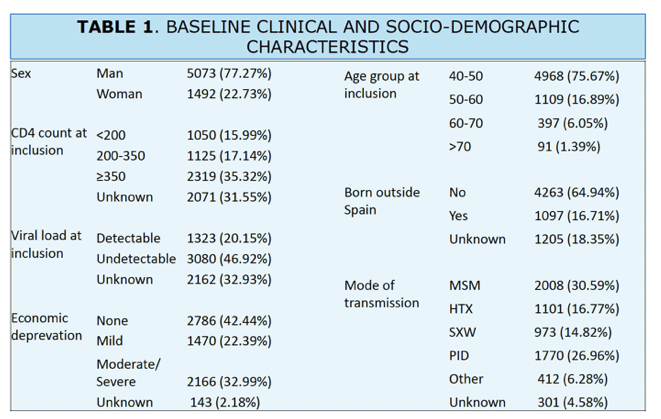
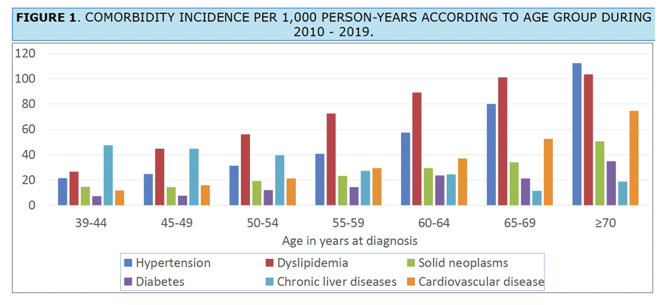
Age was associated with an increased risk for all comorbidities except for solid neoplasms.

AIDS 2022 July 29-Aug 2 Montreal
Presenter
Andreu Bruguera Riera
Authors
A. Bruguera Riera * (1), S. Moreno (1), D. Nomah (1), Y. Diaz (1), J. Aceiton (1), J.M. Llibre (2), V. Falcó (3), A. Imaz (4), P. Domingo (5), H. Knobel (6), E. Leon (7), I. Vilaró (8), J. Casabona (1), J.M. Miró (9), PISCIS study group
Institutions
(1) Center for Epidemiological Studies on Sexually Transmitted Infections and AIDS in Catalonia, Badalona, Spain, (2) Hospital Germans Trias i Pujol, Badalona, Spain, (3) Hospital de la Vall d'Hebron, Barcelona, Spain, (4) Hospital de Bellvitge, Hospitalet del Llobregat, Spain, (5) Hospital Sant Pau, Barcelona, Spain, (6) Hospital del Mar, Barcelona, Spain, (7) Consorci Sanitari Integral, Hospitalet del Llobregat, Spain, (8) Hospital de Vic, Vic, Spain, (9) Hospital Clínic-Institut d'Investigacions Biomèdiques August Pi i Sunyer, Barcelona, Spain
program abstract
BACKGROUND: Since the inception of the combined antiretroviral therapy, remarkable improvements have been witnessed regarding HIV outcomes, but this has led to a rise in chronic comorbidities usually associated with ageing. We described the factors associated with the most prevalent comorbidities in a cohort of people living with HIV (PLWH) aged over 40 years.
METHODS: We conducted a retrospective cohort study using data from the Catalan PLWH cohort (PISCIS) between January 1, 2010, to December 31, 2019. Only patients who were aged 40 years as of the start of the study period were included in the analysis. Chronic conditions were coded according to the Swedish National study of Aging and Care in Kungsholmen (SNAC-K). We used multivariable Cox regression models to assess factors associated with considered comorbidities (dyslipidemia, chronic liver diseases (CLD), hypertension, cardiovascular disease (CVD), solid neoplasms, and diabetes).
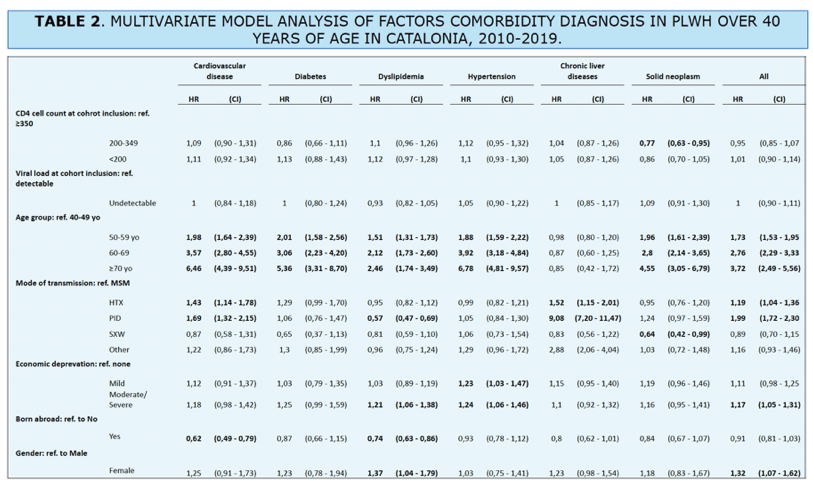
RESULTS: The study included 6565 PLWH at baseline. By the end of the study period, 51.2% patients were without any of the selected comorbidities, while 47.0% had dyslipidemia, 33.6% CLD, 32.1% hypertension, 20.9% CVD, 16.9% solid neoplasms, and 12.4% diabetes. Age was associated with an increased risk for all comorbidities except for solid neoplasms. Heterosexual men (HTX) and people who inject drugs (PWID) presented higher risk for CVD (HR=1.19 [CI=1.04-1.358], HR=1.99 [CI=1.72-2.30]) respectively; diabetes (HR=1.43 [CI=1.14-1.78], HR=1.69 [CI=1.32-2.15]), and solid neoplasms (HR=1.52 [CI=1.15-2.01], HR=9.08 [CI=7.20-11.47]). We observed a lower risk of hypertension among PWID (HR=0.57 [CI=0.47-0.69]) compared to men who have sex with men (MSM). Moderate/severe economic deprivation was linked to a higher risk of CVD (HR=1.17 [CI=1.05-1.31]), hypertension (HR=1.21 [CI=1.06-1.38]), and CLD (HR=1.24 [CI=1.06-1.46]). Migrants had a lower risk of diabetes (HR=0.62 (0.49-0.79]) and hypertension (HR=0.74 (0.63-0.86]), while women had higher risk of CVD (HR=1.32 [CI=1.07-1.62]) and hypertension (HR=1.37 [CI=1.04-1.79]).
CONCLUSIONS: Apart from ageing, there are several sociodemographic factors associated to a higher risk of chronic comorbidities, such as female sex, lower socioeconomic status, being HTX, PWID or of Spanish origin. These factors are crucial in understanding the future health needs of an ageing PLWH population and could be vital in planning public health interventions.




|
| |
|
 |
 |
|
|