 |
 |
 |
| |
Combined Drinking, Smoking, Depression Tied to Higher Mortality in HIV+ US Women
|
| |
| |
AIDS 2022, July 29-August 2, Montreal
Mark Mascolini
Sustained combined heavy drinking, smoking, and depressive symptoms affected nearly 1 in 5 HIV-positive women in a large US cohort [1]. Compared with having none or one of these conditions, having sustained combined conditions—a syndemic state—raised the risk of all-cause mortality, non-AIDS mortality, and non-AIDS or nonoverdose mortality in an analysis of 3282 women with HIV in the Women's Interagency HIV Study (WIHS), a prospective observational cohort.
A team from the University of Florida and other US centers reminded colleagues that heavy drinking, smoking, and depressive symptoms remain highly prevalent in some HIV populations. But research is still meager on co-occurrence of two or more of these conditions—a syndemic—in women with HIV and on whether syndemic conditions synergize to increase mortality.
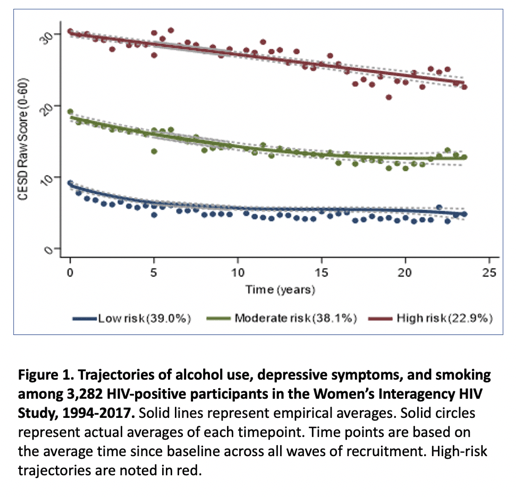
To address these questions, the investigators studied 3282 HIV-positive women enrolled in WIHS in 1994-2017 in three steps: (1) Group-based trajectory models charted long-term patterns of self-reported alcohol use, cigarette smoking, and depressive symptoms. (2) Researchers created syndemic phenotypes based on membership in high-risk trajectories for alcohol use, smoking, and depressive symptoms. (3) Cox proportional hazards models determined whether sustained systemic phenotypes affected all-cause mortality, non-AIDS mortality, and non-AIDS or nonoverdose mortality. The model considered several potential confounders: age, race/ethnicity, education, WIHS enrollment wave, illicit drug use, and time-varying HIV load and CD4 count.
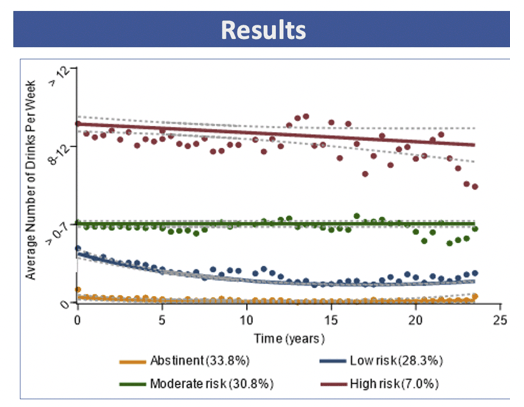
Through a median follow-up of 18.5 years, review of the National Death Index identified 616 deaths and their causes in these WIHS women. Reports of average number of drinks per week classified 33.8% of women as abstinent, 28.3% as low risk, 30.8% as moderate risk, and 7.0% as high risk. According to the raw score of the CESD depression tool, 39.0% of participants were low risk, 38.1% moderate risk, and 22.9% high risk. While 31.2% of the study group never smoked, 14.4% were long-time former smokers, 12.2% were recent quitters, and 42.1% were current smokers.
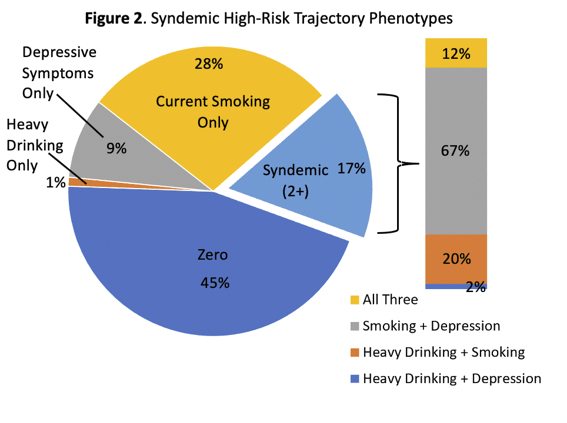
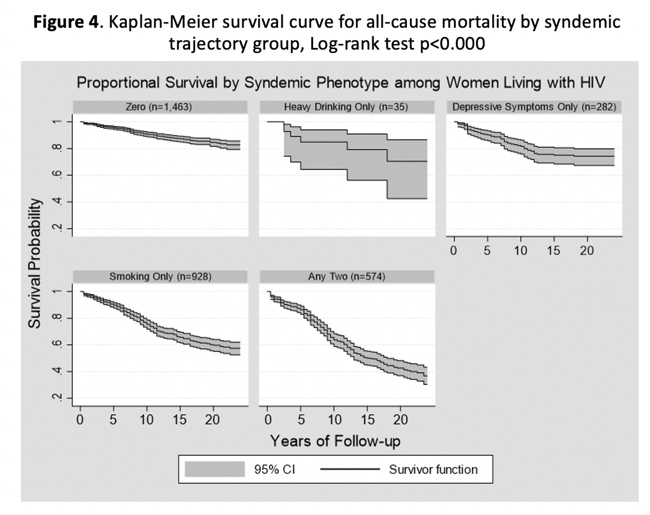
All told, 1% of the study group reported heavy drinking only, 9% had depressive symptoms only, 28% only currently smoked, 17% met syndemic criteria (two or more conditions), and 45% had none of these conditions. In the syndemic group, 67% reported both smoking and depression, 20% reported heavy drinking and smoking, 12% reported all three conditions, and 2% reported heavy drinking plus depression. Kaplan-Meier survival analysis calculated the best 20-year survival in 1463 women with none of the three conditions, slightly worse survival in 35 with heavy drinking only or 282 with depressive symptoms only, much worse survival in 928 with smoking only, and the worst survival in 574 women with any two conditions.
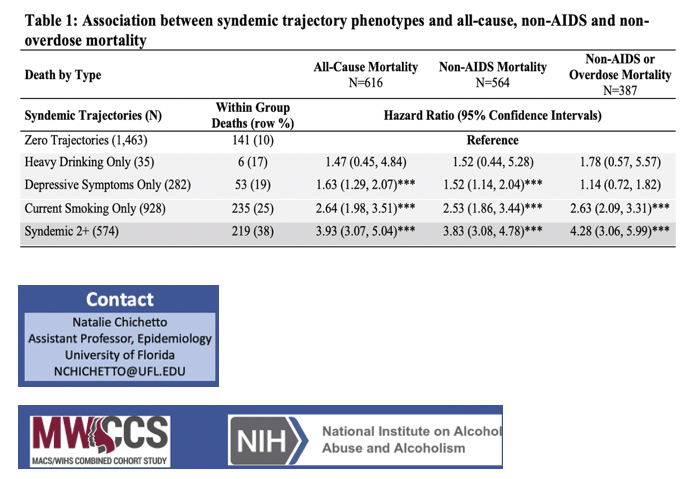
Compared with the zero-trajectory group (10% of whom died), those in the heavy drinking only trajectory (17% of whom died) did not have a significantly greater risk of all-cause mortality, non-AIDS mortality, or non-AIDS or nonoverdose mortality.
But compared with the zero-trajectory group, those in the depressive-symptoms-only trajectory (19% of whom died) ran a significantly higher risk of all-cause mortality (hazard ratio [HR] 1.63, 95% confidence interval [CI] 1.29 to 2.07) and non-AIDS mortality (HR 1.52, 95% CI 1.14 to 2.04). People in the current-smoking-only group (25% of whom died) ran a higher risk of reaching all three mortality endpoints compared with the zero-trajectory cluster: all-cause mortality (HR 2.64, 95% CI 1.98 to 3.51), non-AIDS mortality (HR 2.53, 95% CI 1.86 to 3.44), and non-AIDS or nonoverdose mortality (HR 2.63, 95% CI 2.09 to 3.31). And people in the syndemic trajectory (38% of whom died) had a higher risk of all-cause mortality (HR 3.93, 95% CI 3.07 to 5.04), non-AIDS mortality (HR 3.83, 95% CI 3.08 to 4.78), and non-AIDS or nonoverdose mortality (HR 4.28, 95% CI 3.06 to 5.99) compared with the zero-trajectory group.
Because sustained syndemics carried with them higher death risks, the researchers stressed "the need for coordinated strategies to screen and treat these co-occurring conditions."
Reference
1. Chichetto NE, Gebru NM, Plankey M, et al. Syndemic trajectories of heavy drinking, cigarette smoking, and depressive symptoms are associated with all-cause, non-AIDS, and non-overdose mortality in women living with HIV. AIDS 2022, July 29-August 2, Montreal. Abstract EPB082.

Syndemic Trajectories of Heavy Drinking, Cigarette Smoking, and Depressive Symptoms are Associated with Mortality in Women Living with HIV of the Women's Interagency HIV Study from 1994-2017
NE CHICHETTO1, NM GEBRU1, M PLANKEY2, HA TINDLE3, 4, JR KOETHE3, DB HANNA5, S SHOPTAW6, DL JONES7, JM LAZAR8, JR KIZER9, MH COHEN10; SA HABERLEN11; AA ADIMORA12, CD LAHIRI13, JM WISE14, MS FREIBERG3, 4
1University of Florida, 2Georgetown University Medical Center; 3Vanderbilt University Medical Center; 4Veterans Affairs Tennessee Valley Healthcare System; 5Albert Einstein College of Medicine; 6University of California Los Angeles; 7University of Miami; 8SUNY-Downstate Medical Center; 9San Francisco Veterans Affairs Health Care System, University of California; 10Stroger Hospital/Cook County Health and Hospitals System; 11Johns Hopkins University; 12UNC-Chapel Hill; 13Emory University; 14University of Alabama at Birmingham


|
| |
|
 |
 |
|
|