 |
 |
 |
| |
Macrophage Activation for 2 Years
After Switch From 3 to 2 Antiretrovirals
|
| |
| |
AIDS 2022, July 29-August 2, Montreal
Mark Mascolini
Macrophages became activated after people switched from a triple antiretroviral regimen to 2 antiretrovirals, and activation of these essential immune cells continued for 2 years in a 14-person study [1]. Macrophages are crucial in sensing and responding to pathogens and play a part in tissue repair after injury [2], but the clinical impact of their ongoing activation remains uncertain.
Researchers in Cannes, Nice, and Nimes noted the growing popularity of 2-drug antiretroviral regimens, which have proved virologically noninferior to 3-drug combinations in clinical trials. But whether two-drug antiretroviral therapy (ART) penetrates tissues and cellular reservoirs as well as three-drug combos remains a concern. Such penetration may be crucial to dampening immune activation, which has been linked to clinical outcomes in people with HIV [3]. Prior research linked dual antiretroviral therapy to higher levels of three inflammatory markers [4], and the Cannes team reported a significant jump in sCD163, a signal of macrophage activation, 6 months after a switch to dual therapy in people with a low CD4 nadir, previous AIDS, or low-level viremia [5].
Researchers invited patients at Cannes General Hospital and the Infectious Diseases Department at Nice University to join this 3-to-2 switch study if they met two criteria: taking ART with a viral load below 50 copies for at least 6 months, and switching from a triple-drug regimen to a dual-drug combination for simplification. The researchers excluded people not taking a stable regimen or taking four antiretrovirals. The investigators measured immune activation markers (IP-10, MCP-1, sCD163, sCD14) before the 3-to-2 switch, 6 months after the switch, and between 18 and 24 months later.
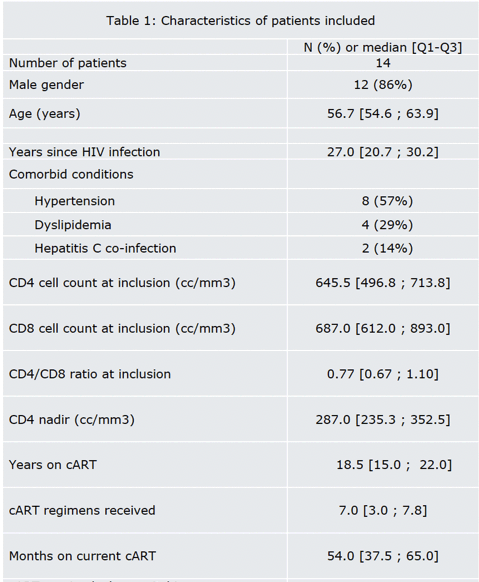
Twelve of the 14 study participants were men, and median age stood at 56.7 years. Median entry CD4 count was 645.5, CD8 count 687.0, CD4 nadir 287, years on antiretroviral therapy 18.5, antiretroviral regimens received 7, and months on current ART 54. Eight people were taking two nucleos(t)ides (NRTIs) and an integrase inhibitor, 5 were taking two NRTIs and a nonnucleoside, and 1 was taking another regimen. Eleven people switched to dolutegravir plus rilpivirine and 3 to dolutegravir plus lamivudine.
On the basis of age, years since HIV infection, years on ART, CD4/CD8 ratio, number of regimens received, and trajectories of the activation markers studied, the researchers divided the group into 7 people with a lower likelihood of immune activation and 7 with a higher likelihood.
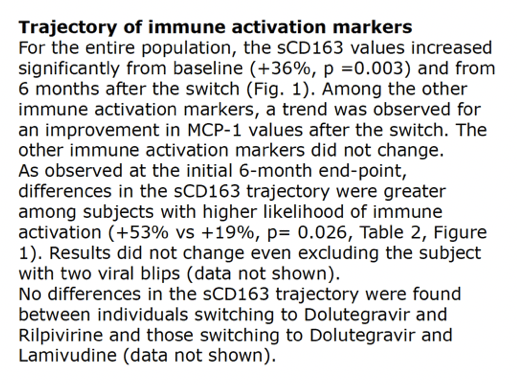
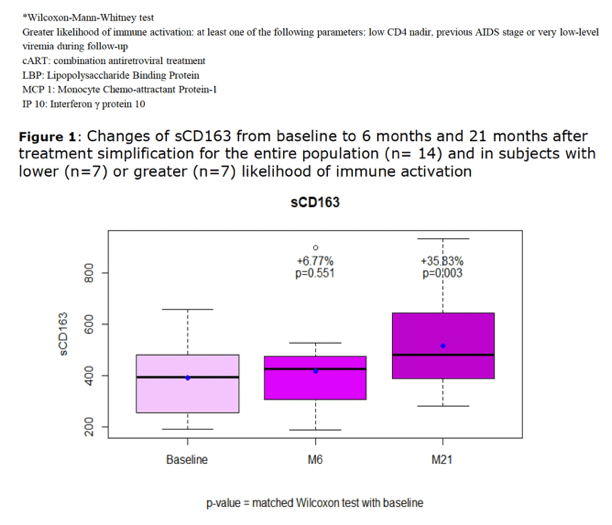
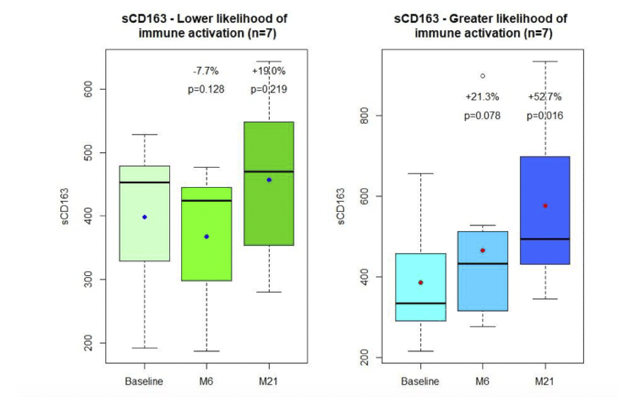
Levels of sCD163, the macrophage activation marker, rose by 6.77% from baseline to month 6 (not significant) and by 35.83% at month 21 (significant at P = 0.003). In the 7 people judged to have a higher likelihood of activation, the 6- and 21-month changes in sCD163 were 21.3% (P = 0.078, not significant) and 52.7% (P = 0.016, significant). In the 7 people with a lower likelihood of activation, the 6- and 21-month changes were -7.7% (P = 0.128, not significant) and 19.0% (P = 0.219, not significant).
The increase in macrophage activation was significant for the whole group and was higher in people with a low CD4 nadir, a previous AIDS diagnosis, or detectable residual viremia during follow-up. The researchers noted that the clinical impact of monocyte/macrophage activation in such patients remains to be defined, but they cited research indicating that sCD163 is a risk factor for non-AIDS conditions including HIV-associated neurocognitive disorders, cardiovascular disease, and liver fibrosis [6-9].
The investigators suggested two hypotheses to explain macrophage activation after a 3-to-2 switch: (1) Low lymph node penetration by integrase inhibitors and stopping 1 NRTI could result in insufficient antiretroviral pressure in viral reservoirs. (2) Switching from 2 NRTIs to 1 could lower a regimen’s ability to stifle cell-to-cell transmission of HIV-1.
References
1. Vassllo M, Durant J, Fabre R, et al. Switching to dual drug HIV regimen is associated with macrophage activation on a 2-years follow-up. AIDS 2022, July 29-August 2, Montreal. Abstract EPB125.
2. Watanabe S, Alexander M, Misharin AV, Budinger GRS. The role of macrophages in the resolution of inflammation. J Clin Invest. 2019;129:2619-2628. doi: 10.1172/JCI124615. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6597225/
3. Serrano-Villar S, Pérez-Elías MJ, Dronda F, et al. Increased risk of serious non-AIDS-related events in HIV-infected subjects on antiretroviral therapy associated with a low CD4/CD8 ratio. PLoS One. 2014;9:e8579.
4. Serrano-Villar S, Lopez-Huertas MR, Jimenez D, et al. A retrospective analysis of long-term changes of inflammatory biomarkers in individuals on suppressive three-drug or two-drug antiretroviral regimens. Lancet pre-print. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3976877
5. Vassallo M, Durant J, Fabre R, et al. Switching to a dual drug regimen in HIV-infected patients could be associated with macrophage activation? Front Med (Lausanne). 2021;8:712880.
6. Lidofsky A, Holmes JA, Feeney ER, et al. Macrophage activation marker soluble CD163 is a dynamic marker of liver fibrogenesis in human immunodeficiency virus/hepatitis C virus coinfection. J Infect Dis. 2018;218:1394-1403.
7. McKibben RA, Margolick JB, Grinspoon S, et al. Elevated levels of monocyte activation markers are associated with subclinical atherosclerosis in men with and those without HIV infection. J Infect Dis. 2015;211:1219-1228.
8. Knudsen TB, Ertner G, Petersen J, et al. Plasma soluble CD163 level independently predicts all-cause mortality in HIV-1-infected individuals. Clin Infect Dis. 2016;214:1198-1204.
9. Castley A, Williams L, James I, et al. Plasma CXCL10, sCD163 and sCD14 levels have distinct associations with antiretroviral treatment and cardiovascular disease risk factors. Plos One. 2016;11:e0158169.












Assessing the lymphoid tissue bioavailability of antiretrovirals in human primary lymphoid endothelial cells and in mice
https://academic.oup.com/jac/article/74/10/2974/5537354?login=false
Abstract
Background
The secondary lymphoid tissues (LTs), lymph nodes (LNs) and gut-associated lymphoid tissue (GALT) are considered reservoirs for HIV. Antiretrovirals (ARVs) have lower penetration into LT. In vitro models predictive of ARV LT penetration have not been established.
Objectives
To develop an in vitro model of LT bioavailability using human lymphoid endothelial cells (HLECs) and investigate its predictability with in vivo pharmacokinetic (PK) studies in mice.
Methods
ARV bioavailability in HLECs was evaluated at the maximum plasma concentration (Cmax) observed in HIV-infected patients. ARVs were: abacavir, atazanavir, darunavir, dolutegravir, efavirenz, elvitegravir, emtricitabine, maraviroc, raltegravir, rilpivirine, ritonavir, tenofovir disoproxil fumarate and the PK booster cobicistat. The LT PK of representative drugs showing high (efavirenz), intermediate (dolutegravir) and low (emtricitabine) HLEC bioavailability was investigated in BALB/c mice given 50/10/30 mg/kg efavirenz/dolutegravir/emtricitabine orally, daily for 3 days. The concordance of in vitro and in vivo ARV bioavailability was examined.
Results
ARVs showed high (>67th percentile; rilpivirine, efavirenz, elvitegravir and cobicistat), intermediate (67th-33rd percentile; ritonavir, tenofovir disoproxil fumarate, dolutegravir and maraviroc) and low (<33rd percentile; atazanavir, darunavir, raltegravir, emtricitabine and abacavir) HLEC bioavailability. The hierarchy of efavirenz, dolutegravir and emtricitabine bioavailability in LN, gut and brain tissues of mice was: efavirenz>dolutegravir>emtricitabine.
Conclusions
ARVs displayed distinct HLEC penetration patterns. PK studies of representative ARVs in LT of mice were concordant with HLEC bioavailability. These findings support further development of this approach and its translational predictability in humans.
Protease inhibitors effectively block cell-to-cell spread of HIV-1 between T cells
https://retrovirology.biomedcentral.com/articles/10.1186/1742-4690-10-161
Abstract
Background
The Human Immunodeficiency Virus type-1 (HIV-1) spreads by cell-free diffusion and by direct cell-to-cell transfer, the latter being a significantly more efficient mode of transmission. Recently it has been suggested that cell-to-cell spread may permit ongoing virus replication in the presence of antiretroviral therapy (ART) based on studies performed using Reverse Transcriptase Inhibitors (RTIs). Protease Inhibitors (PIs) constitute an important component of ART; however whether this class of inhibitors can suppress cell-to-cell transfer of HIV-1 is unexplored. Here we have evaluated the inhibitory effect of PIs during cell-to-cell spread of HIV-1 between T lymphocytes.
Results
Using quantitative assays in cell line and primary cell systems that directly measure the early steps of HIV-1 infection we find that the PIs Lopinavir and Darunavir are equally potent against both cell-free and cell-to-cell spread of HIV-1. We further show that a protease resistant mutant maintains its resistant phenotype during cell-to-cell spread and is transmitted more efficiently than wild-type virus in the presence of drug. By contrast we find that T cell-T cell spread of HIV-1 is 4-20 fold more resistant to inhibition by the RTIs Nevirapine, Zidovudine and Tenofovir. Notably, varying the ratio of infected and uninfected cells in co-culture impacted on the degree of inhibition, indicating that the relative efficacy of ART is dependent on the multiplicity of infection.
Conclusions
We conclude that if the variable effects of antiviral drugs on cell-to-cell virus dissemination of HIV-1 do indeed impact on viral replication and maintenance of viral reservoirs this is likely to be influenced by the antiviral drug class, since PIs appear particularly effective against both modes of HIV-1 spread.
|
| |
|
 |
 |
|
|