 |
 |
 |
| |
Aldafermin Meets 48-Week Primary and Secondary Endpoints for MASH Cirrhosis
|
| |
| |
AASLD 2023 nov 10-14
listen to live session
https://www.aasld.org/the-liver-meeting
AASLD 2023, The Liver Meeting, November 10-14, 2023, Boston
Mark Mascolini
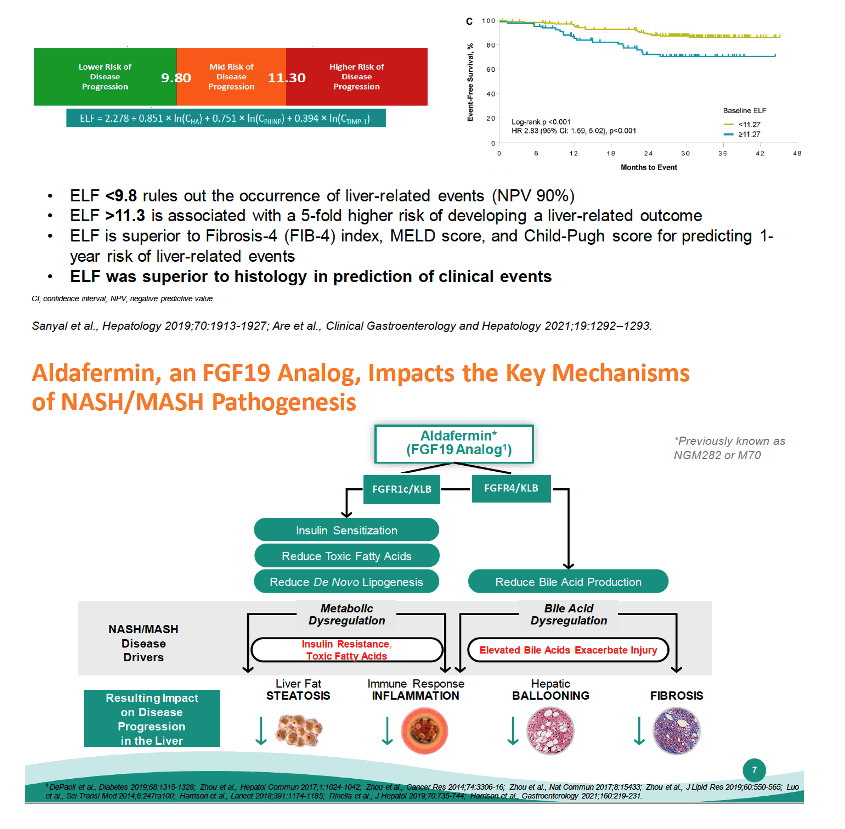
In the first late-stage randomized controlled trial involving compensated MASH/NASH cirrhosis that met its primary endpoint, ALPINE-4 found that 3 mg of aldafermin daily significantly lowered enhanced liver fibrosis (ELF) score from baseline to week 48 [1]. Prior worked showed that ELF predicts liver-related events in people with compensated cirrhosis related to metabolic dysfunction-associated steatohepatitis (MASH, formerly called NASH) [2]. ELF was the first and remains the only FDA-approved serum-based noninvasive test for prognostic assessment of MASH, according to ALPINE-4 researchers.
Aldafermin, an FGF19 analog, disrupts MASH pathogenesis by cutting bile acid production and-by promoting insulin sensitization and curbing toxic fatty acid-dampening de novo lipogenesis (fatty acid synthesis). If left unchecked, these two mechanisms result in steatosis, inflammation, hepatic cell ballooning, and fibrosis.
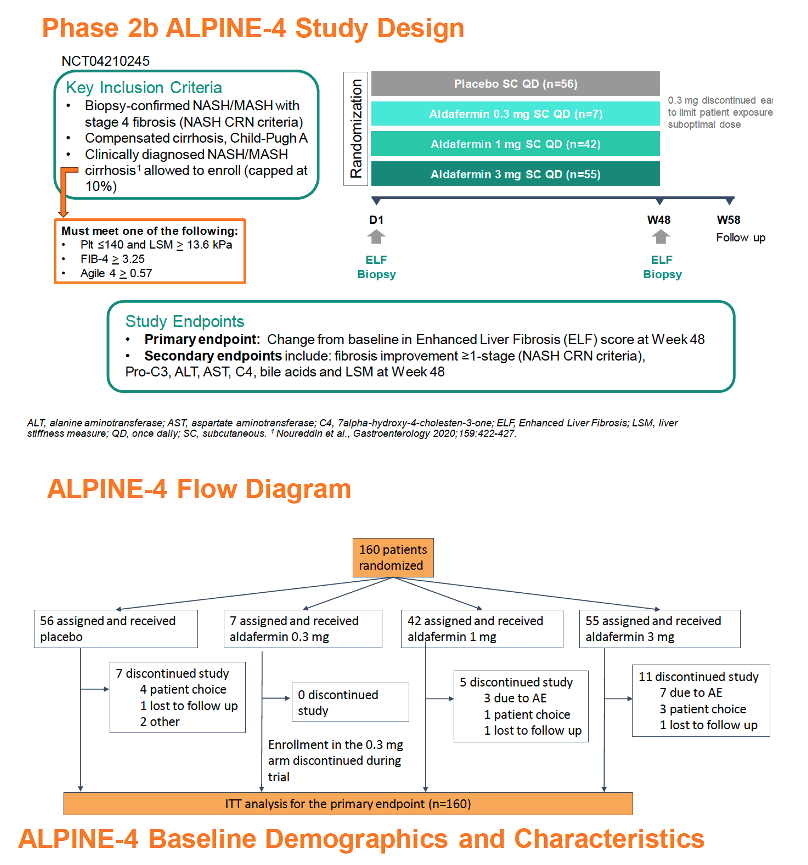
ALPINE-4 recruited people with (1) biopsy-confirmed MASH with stage 4 fibrosis, (2) compensated cirrhosis (Child-Pugh class A), or (3) clinically diagnosed MASH cirrhosis. The ALPINE investigators randomized 56 participants to placebo, 7 to 0.3 mg of subcutaneous aldafermin daily, 42 to 1 mg of subcutaneous aldafermin daily, and 55 to 3 mg of subcutaneous aldafermin daily. The 0.3-mg arm stopped early to limit exposure to a suboptimal dose. Everyone else continued aldafermin or placebo for 48 weeks. The primary endpoint was change from baseline ELF score at week 48. The intention-to-treat analysis for the primary endpoint involved 160 participants. The University of Chicago's Mary Rinella and ALPINE-4 colleagues published results of the trial shortly before The AASLD Liver Meeting [3].
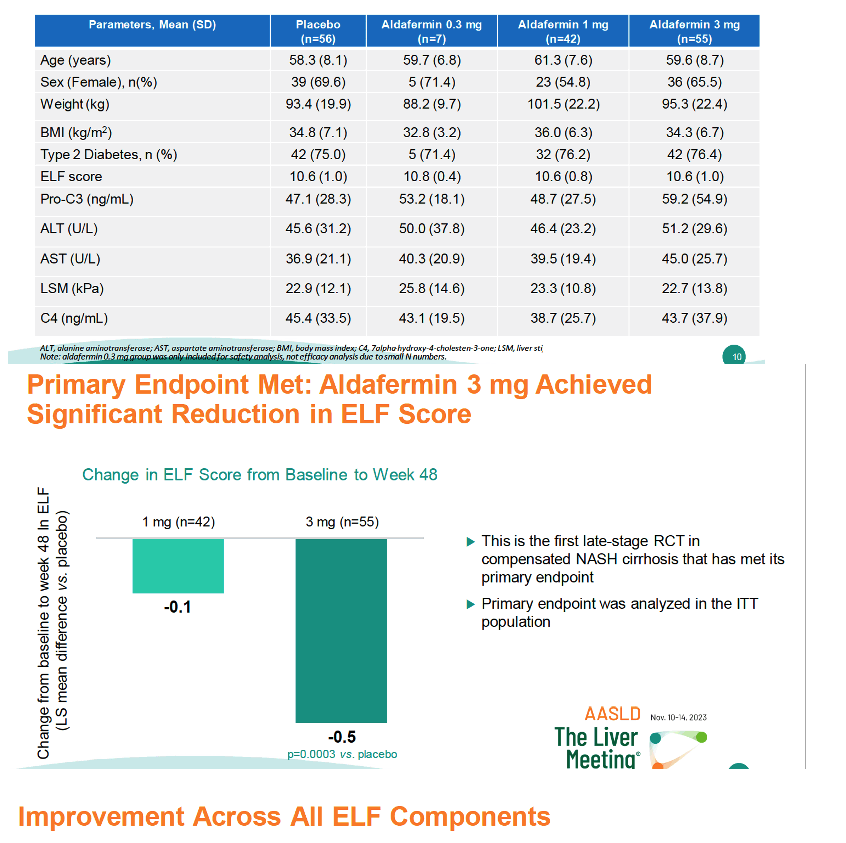
Average age was similar across the four study arms at about 60 years, and about 60% of participants were women. Body mass index averaged about 35 kg/m2 across the four arms, and about three quarters had diabetes. ELF score averaged about 10.6 in trial participants and ALT around 50 U/L.
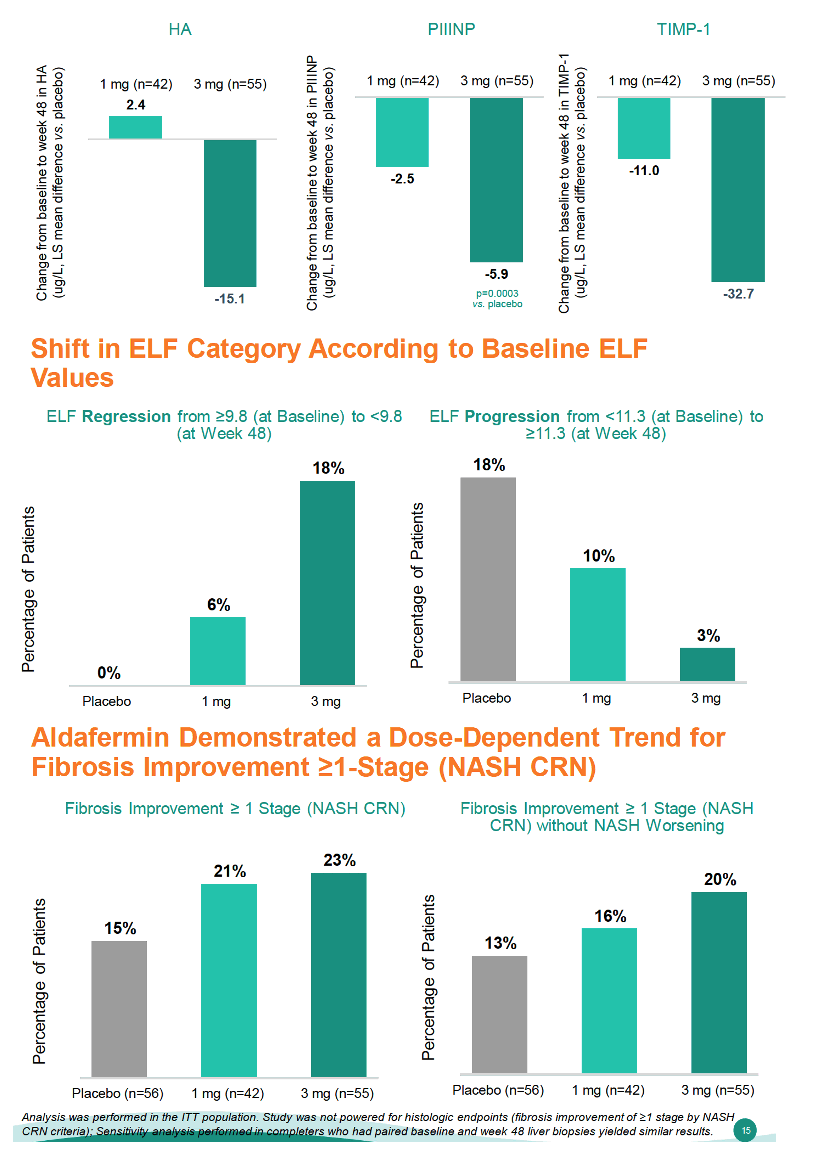
By week 48 the ELF score dropped 0.5 in the 3-mg aldafermin arm, a significant decline in an intention-to-treat analysis meaning the drug met the trial's primary endpoint (P = 0.0003 vs placebo). ELF dipped by only 0.1 through week 48 in the 1-mg aldafermin group. Type III N-terminal procollagen peptide (PIIINP), a fibrosis marker, also fell significantly with 3 mg of aldafermin (-5.9, P = 0.0003 vs placebo), compared with a drop of -2.5 with 1 mg of aldafermin. Levels of two other markers, hyaluronic acid and TIMP-1, also fell more with 3 mg than 1 mg, but the 3-mg drops did not differ significantly from placebo results.
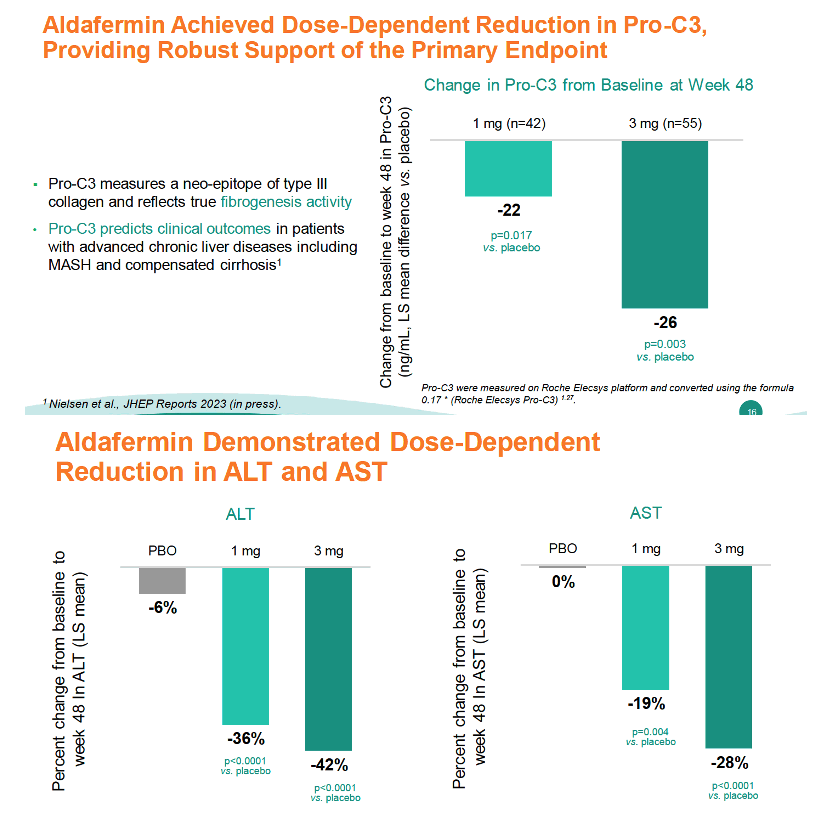
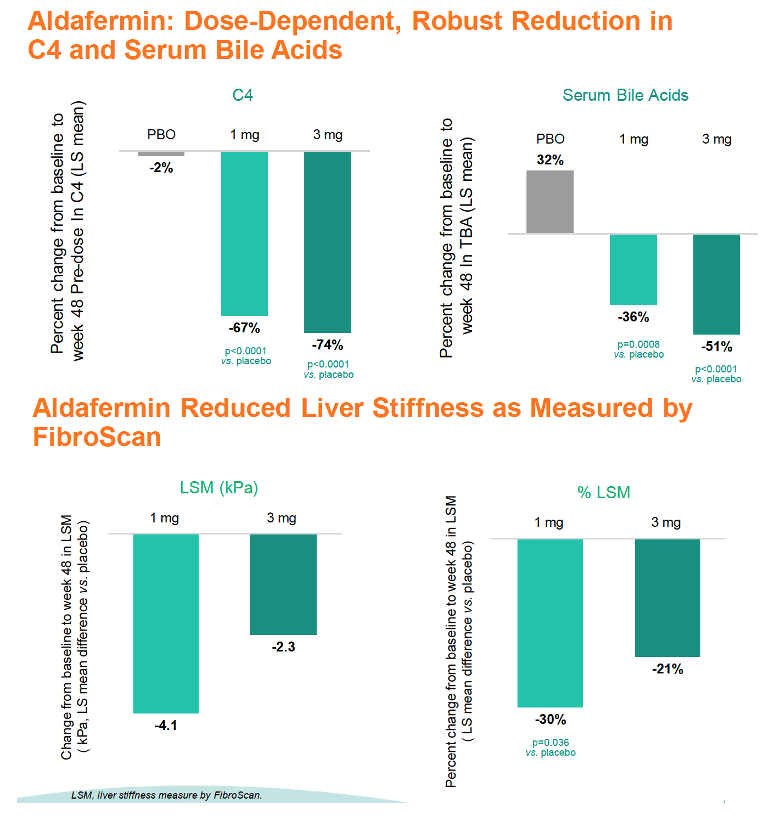
The ALPINE-4 team recorded ELF regression from above to below 9.8 by week 48 in 18% randomized to 3 mg of aldafermin versus 6% randomized to 1 mg and 0% randomized to placebo. ELF progression from below to above 11.3 occurred in 18% taking placebo, 10% taking 1 mg of aldafermin, and 3% taking 3 mg. The researchers also recorded dose-dependent trends to fibrosis improvement of 1 NASH stage or more and of 1 NASH stage or more without NASH worsening. The investigators interpreted a dose-dependent drop in Pro-C3 (a fibrogenesis-based NASH biomarker that predicts clinical outcomes with advanced chronic liver disease including MASH) as "robust support of the primary endpoint (-26 with 3 mg, P = 0.003 vs placebo, and -22 with 1 mg vs placebo, P = 0.017 vs placebo). These Pro-C3 declines correspond to about a 60% relative reduction with 3 mg of aldafermin and about 50% with 1 mg. Aldafermin also reduced ALT, AST, C4, and serum bile acids in a dose-dependent manner. And the drug eased FibroScan-calculated liver stiffness measure (LSM), but more so with 1 mg (-30%, P = 0.036 vs placebo) than with 3 mg (-21%, not significant vs placebo).
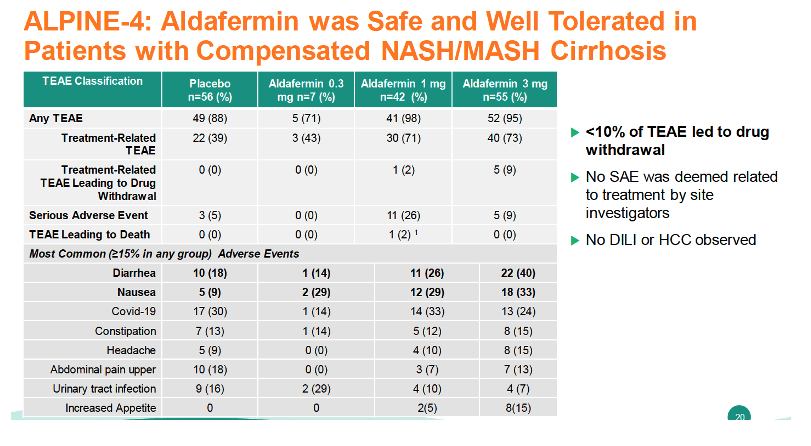
Fewer than 10% of ALPINE-4 participants had a treatment-emergent adverse event that led them to stop therapy. Site investigators recorded no serious adverse events related to treatment. They counted 5 treatment-related adverse events in the 3-mg arm (9% of 55), 1 in the 1-mg arm (2% of 42) and none in the 0.3-mg or placebo arms. No cases of hepatocellular carcinoma or drug-induced liver injury emerged.
The trial did not demonstrate significant histologic improvement with aldafermin through 48 weeks, but the investigators noted that ALPINE-4 was not statistically powered to detect significant histologic changes.
References
1. Rinella ME, Lieu HD, Kowdley K, et al. Positive results from the ALPINE-4 study: a randomized, double-blind, placebo-controlled, multicenter, phase 2b trial evaluating multiple doses of the FGF19 analogue aldafermin in patients with compensated cirrhosis due to nonalcoholic steatohepatitis. AASLD 2023, The Liver Meeting, November 10-14, 2023, Boston.
2. Sanyal AJ, Shankar SS, Yates KP, et al. Diagnostic performance of circulating biomarkers for non-alcoholic steatohepatitis. Nat Med. 2023;29:2656-2664. doi: 10.1038/s41591-023-02539-6. https://www.nature.com/articles/s41591-023-02539-6
3. Rinella ME, Lieu HD, Kowdley KV, et al. A randomized, double-blind, placebo-controlled trial of aldafermin in patients with nonalcoholic steatohepatitis and compensated cirrhosis. Hepatology. 2023 Sep 21. doi: 10.1097/HEP.0000000000000607. https://journals.lww.com/hep/abstract/9900/a_randomized,_double_blind,_placebo_controlled.577.aspx


|
| |
|
 |
 |
|
|