 |
 |
 |
| |
Potential impact and efficiency of doxy-PEP among people with or at risk of HIV
|
| |
| |
Michael Traeger, Kenneth Mayer, Douglas Krakower, Sy Gitin, Samuel Jenness, Julia Marcus
CROI, Seattle
February 20th 2023
Michael Traeger, Fellow, Department of Population Medicine, Harvard Medical School

Press conference summary - 2-3 minutes
Study aim:
• Doxycycline post-exposure prophylaxis was recently shown to be highly efficacious for preventing bacterial STIs among people with HIV or using PrEP, but decision-making about doxyPEP prescribing is complicated by concerns about potential harms of widespread antibiotic use.
• The aim of our study was to identify doxyPEP prescribing strategies that would minimize overall doxycycline use, while maximizing impact on STIs, to help inform the implementation of doxyPEP in clinical practice.
Study methods:
• To do this, we utilized STI testing data from electronic health records of more than 10,500 patients accessing care at Fenway Health, a large health centre in Boston specialising in care for sexual and gender minorities.
• We explored 10 hypothetical doxyPEP prescribing strategies. Some strategies would prescribe doxyPEP to specific patient groups, for example PrEP users or people with HIV. Other strategies would prescribe doxyPEP to patients following one or more STI diagnoses - for example, after a rectal STI diagnosis or after 2 STI diagnoses within 12 months.
• We evaluated these prescribing strategies by retrospectively examining STI testing data from 2015 to 2020. We assumed that doxyPEP would have been prescribed and used when patients met the criteria for our hypothetical prescribing strategies, and that STI incidence would have been reduced by efficacy estimates from a previous clinical trial.
Main findings:
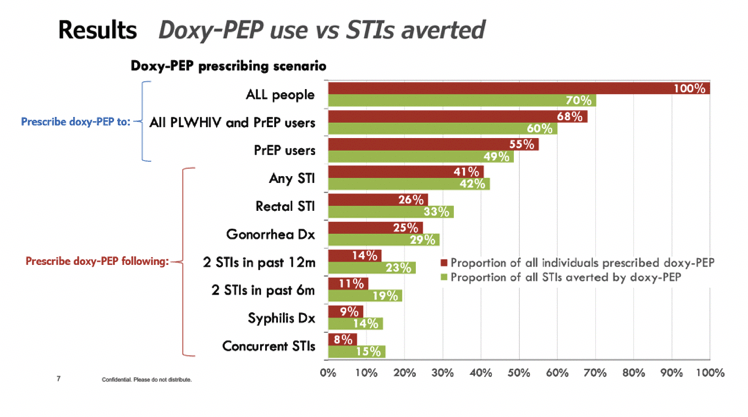
• Overall, our data suggested that prescribing doxyPEP for 12 months at a time to people with an STI diagnosis could avert 42% of subsequent STIs.
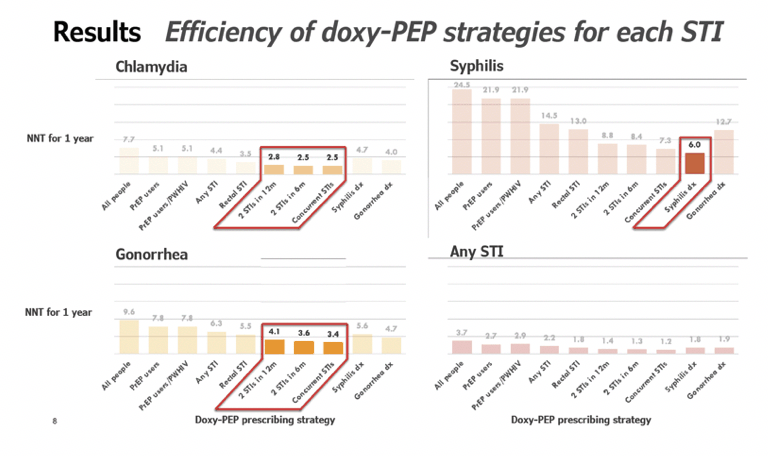
• We found that strategies that involved prescribing doxyPEP for 12 months following an STI diagnosis would be more efficient than prescribing doxyPEP to all PrEP users or people with HIV - that is to say, fewer people would need to be prescribed doxyPEP to prevent the same number of STIs.
• The potential impact and efficiency of prescribing strategies varied across STIs. In one strategy, prescribing doxyPEP to people diagnosed with syphilis could avert up to 25% of subsequent syphilis infections, with only 9% of all people needing to use doxyPEP.
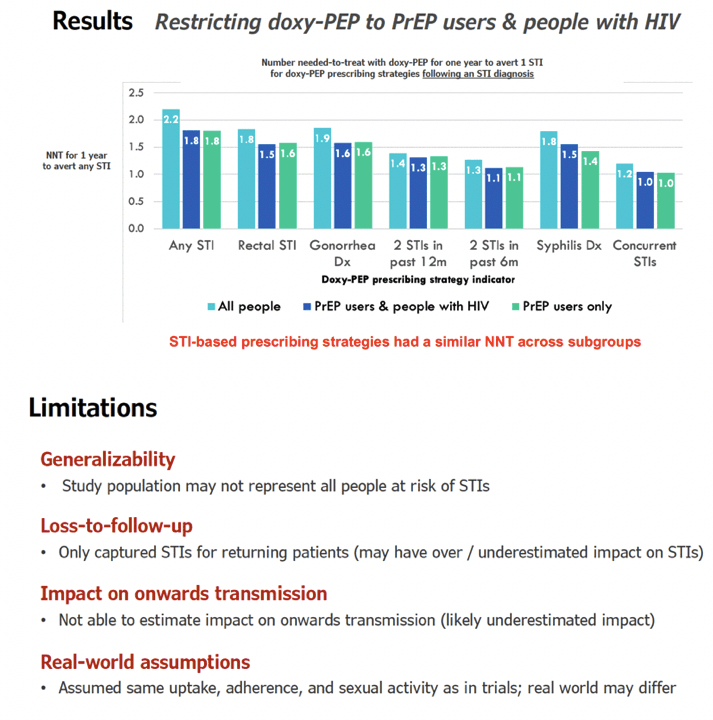
• We found that if doxyPEP were prescribed following an STI diagnosis, it would have a similar efficiency among people with HIV, PrEP users and non-PrEP users, suggesting that restricting doxyPEP to subgroups of people with STIs may not be warranted.
• Limitations of our study were that we could not estimate the impact of doxyPEP on preventing onward transmission to sexual partners, and that our assumptions about doxyPEP uptake, adherence and sexual activity were taken from a clinical trial setting and may differ during real-world implementation.
In closing:
• Our findings can help inform clinical guidelines for doxyPEP prescribing that balance potential benefits and harms of use. Specifically, our analysis suggests that the most efficient doxyPEP prescribing strategies are based on STI history rather than PrEP use or HIV status.
• Additional research will be needed to understand and optimize real-world implementation of doxyPEP, including access, uptake, adherence, impact on STI incidence, and patient-reported outcomes.





|
| |
|
 |
 |
|
|