 |
 |
 |
| |
Mortality 1 Year After ICU Admission Falls Over 20 Years in HIV Group
|
| |
| |
30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle
Mark Mascolini
Risk of dying 1 year after intensive care unit (ICU) admission fell 10% yearly over 20 years in a single-center UK group with HIV [1]. University College London and Royal Free Hospital researchers believe their findings add to evidence that HIV infection should not in itself be a factor in determining which patients get admitted to the ICU.
In-ICU and in-hospital mortality have dropped sharply in people with HIV, noted researchers who conducted this study. This improvement can be traced to changing reasons for ICU admission among people with HIV and to improvements in ICU care [2]. Because less is known about long-term outcomes in ICU patients with HIV, the London team conducted this retrospective study.
The analysis focused on people with HIV admitted to an ICU at the Royal Free Hospital, an HIV referral center, in the two decades spanning 2000-2019. Researchers calculated 1-year mortality from the time of initial ICU admission to the date of death, including deaths in the hospital. Follow-up lasted 365 days from the day of admission in people who remained alive for 1 year, and follow-up lasted for 7 days in people lost to follow-up after ICU discharge.
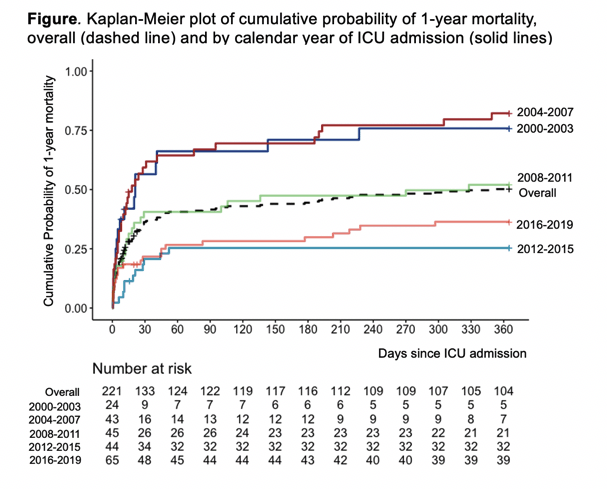
The study cohort included 221 people, 72% of them male. Just under half of this group (108 people, 48.9%) died within 1 year of ICU admission. Median survival reached 349 days and cumulative 1-year survival 50%.
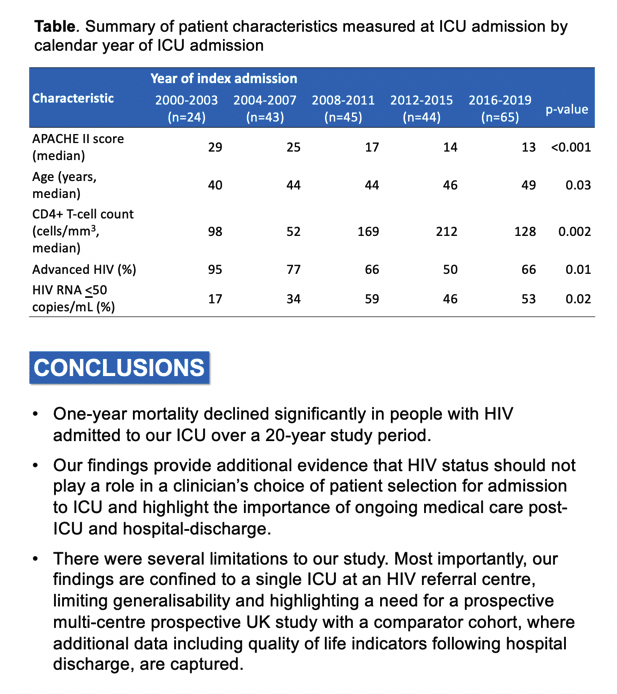
Median age stood at 40 years in people admitted to the ICU in 2000-2003, 44 in those admitted in 2004-2007, 44 in the 2008-2011 group, 46 in the 2012-2015 cohort, and 49 in the 2016-2019 group (P = 0.03). Respective median APACHE II scores (a standard measure of disease severity in ICU patients [3]) were 29, 25, 17, 14, and 13 (P < 0.001) and CD4 counts 98, 52, 169, 212, and 128 (P = 0.002). Respective proportions with a viral load at or below 50 copies were 17%, 34%, 59%, 46%, and 53% (P = 0.02).
Kaplan-Meier analysis of cumulative probability of 1-year mortality proved best for the 2012-2015 group, followed by 2016-2019, 2008-2011 (whose survival probability curve virtually overlapped that of the whole cohort), and 2000-2003, whose survival curve virtually overlapped 2004-2007. Log-rank test determined that cumulative survival rose significantly in more recent study-year cohorts (P = 0.001). Risk of 1-year mortality fell 10% with each more recent year (hazard ratio 0.90, 95% confidence interval 0.87 to 0.93). Analysis adjusted for demographic and clinical factors figured that 1-year mortality risk fell 7% with each more recent year (adjusted hazard ratio 0.93, 95% confidence interval 0.89 to 0.98).
The London team argued that their findings bolster evidence that clinicians should not consider HIV status when contemplating ICU admission. At the same time, they added, these results stress the importance of ongoing care for people with HIV after discharge from the ICU and hospital. Study limitations include the focus on a single ICU at an HIV referral center. And the study did not consider the possible impact of gender, race, socioeconomic status, and comorbidities common in people with HIV infection.
References
1. Balewell N, Sabin CA, Kanitkar T, et al. One-year mortality of people with HIV after intensive care unit admission. 30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle. Abstract 874.
2. Ford N, Patten G , Rangaraj A , Davies MA, Meintjes G, Ellman T. Outcomes of people living with HIV after hospital discharge: a systematic review and meta-analysis. 2022;9:e150-e159. doi: 10.1016/S2352-3018(21)00329-5.
https://www.thelancet.com/journals/lanhiv/article/PIIS2352-3018(21)00329-5/fulltext
3. mdcalc.com. APACHE II score. https://www.mdcalc.com/calc/1868/apache-ii-score




|
| |
|
 |
 |
|
|