 |
 |
 |
| |
Non-AIDS Defining Malignancy Mortality In People Living
With HIV; CD4 is biggest risk factor, next is smoking
|
| |
| |
CROI 2023 Feb 20-23
Marta Rava1,2, Félix Gutierrez3,2, José A. Pérez-Molina4,2, Inés Suarez-García5, 2, Francisco Jesús-Vera6, Fernando Baigorria7, Mar Masiá3,2, Juan Macías8,2, Gemma Navarro9, Santiago Moreno4,2, Inma Jarrin1,2 for the CoRIS cohort 1Carlos III Health Institute (ISCIII), Madrid, Spain, 2CIBERINFEC, ISCIII, Madrid, Spain, 3Hospital General Universitario de Elche, Alicante, Spain, 4Hospital Ramón y Cajal, Madrid, Spain, 5Hospital Universitario Infanta Sofía, Madrid, Spain, 6Hospital General Universitario Santa Lucía, Cartagena, Spain, 7Complejo Hospitalario de Navarra, Pamplona, Spain, 8Hospital Universitario Virgen de Valme, Sevilla, Spain, 9Parc Taulí Hospital Universitari; Barcelona, Spain

program abstract
Background: Our aim was to evaluate rate and prognostic factors of mortality due to non-AIDS defining malignancies (NADM) among persons living with HIV (PLWH) from the cohort of the Spanish AIDS Research Network (CoRIS) during 2004-2020.
Methods:We included antiretroviral-naive individuals aged ≥ 20 years at enrolment, recruited during 2004-2020. NADM deaths were all deaths due to cancer, except those due to AIDS defining malignancies such as Kaposi sarcoma, certain types of non-Hodgkin lymphomas and cervical cancer. We estimated mortality rates and standardised mortality ratios (SMRs) using NADM mortality rates from the Spanish general population. We applied cause-specific Cox proportional hazard models, accounting for competing risk, and age as time-scale to identify prognostic factors for NADM mortality.
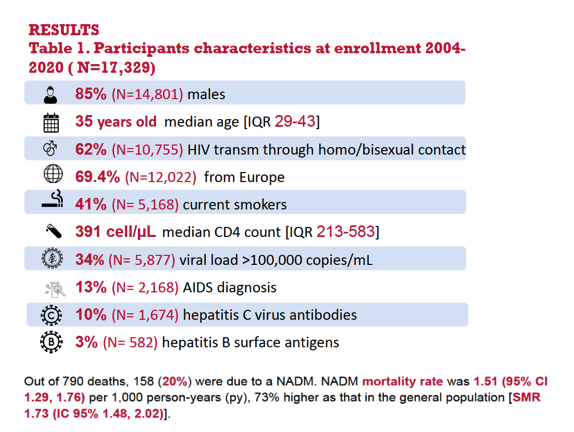
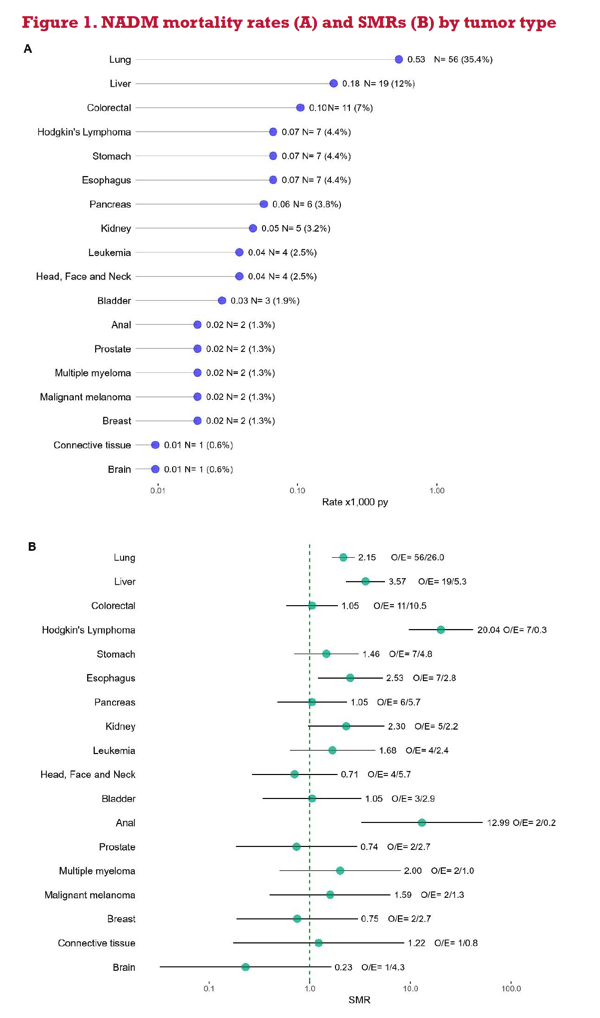
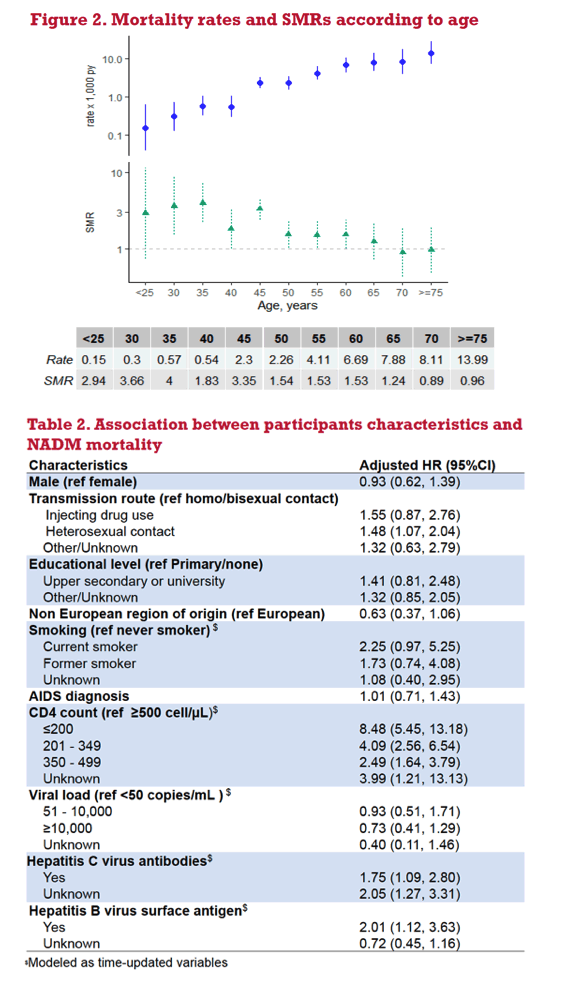
Results: Of the 17,329 study participants, 85% were men and median age was 35 years. The overall mortality rate was 1.53 (95% confidence interval: 1.32, 1.79) per 1,000 person-years (PY), 76% higher as that in the general population (SMR: 1.76, 95% CI 1.51, 2.06). The highest mortality rates were found for lung (0.56 per 1,000 PY; 95%CI 0.44, 0.73) and liver cancer (0.18 per 1,000 PY, 95%CI 0.12, 0.28). Mortality rates increased with age, whereas SMRs decreased from 3.42 (95%CI 1.63, 7.18) at ≤35 years to 0.92 (95%CI 0.56, 1.53) at ≥70 years. Risk of NADM mortality was higher in participants that acquired infection through heterosexual contact (Hazard Ratio: 1.48; 95%CI 1.07, 2.03) and injection drug use (HR: 1.54 (0.87, 2.76), compared to men who have sex with men. Time-varying prognostic factors for NADM mortality were: active smoking (HR: 2.23; 95%CI 0.96, 5.18), presence of hepatitis C virus antibodies (HR: 1.74; 95%CI 1.09, 2.78) or hepatitis B surface antigen (HR: 2.02; 95%CI 1.12, 3.66) and decreasing CD4 count (HR: 8.49; 95%CI 5.46, 13.20 for CD4< 200 cells/μl, HR: 4.10; 95%CI 2.57, 6.55 for CD4 200-349 cells/μl;HR: 2.50; 95%CI 1.64, 3.80 for CD4 350-499 cells/μl compared to CD4≥500 cells/μl).
Conclusion: Mortality due to NADM in PLWH is higher than in the general population, mainly at younger ages. Smoking, viral hepatitis coinfections and immunosuppression independently increased risk of death due to NADM.


|
| |
|
 |
 |
|
|