 |
 |
 |
| |
INFUSION OF CCR5 GENE-MODIFIED T CELLS
PROVIDES LONG-TERM HIV CONTROL
|
| |
| |
CROI 2023 Feb 20-23
Ana B. Enriquez
Emory University
Atlanta, GA, USA
program abstract
Ashish A. Sharma1*, Joumana Zeidan1*, Ana B. Enriquez1, Gary Lee2, Remi Fromentin3,4, Slim Fourati1, Khader Ghneim1, Gabriela P. Sanchez1, Francesco A. Procopio5, Robert Balderas6, Jacob P. Lalezari7, Nicolas Chomont3,4, Dale Ando2, Steven G. Deeks8, and Rafick-Pierre Sekaly1
1Emory University, Atlanta, GA, USA
2Sangamo Therapeutics, Richmond, CA, USA
3Université de Montréal, Faculty of Medicine, Department of Microbiology, Infectiology, and Immunology, Montréal, Québec, Canada
4Université de Montréal, Centre de Recherche du CHUM, Montréal, Québec, Canada
5Lausanne University Hospital (CHUV), Lausanne, Switzerland
6BD Biosciences, San Jose, CA, USA
7Quest Clinical Research, San Francisco, CA, USA
8University of California, San Francisco and San Francisco General Hospital, San Francisco, CA, USA
Background: Antiretroviral therapy (ART) fails to fully restore immune function and is not curative, therefore more effective therapies are required for people with HIV (PWH). A cure for HIV has previously been observed in several individuals in which bone marrow transfer of CCR5-modified stem cells for leukemia treatment was also found to eliminate HIV. While these results are encouraging, a less invasive and more broadly applicable curative strategy is warranted. Transfer of autologous CCR5-modified CD4 T cells has been found to be safe and well-tolerated in PWH. However, whether this treatment re-programs the immune response to provide long-term viral control is unknown.
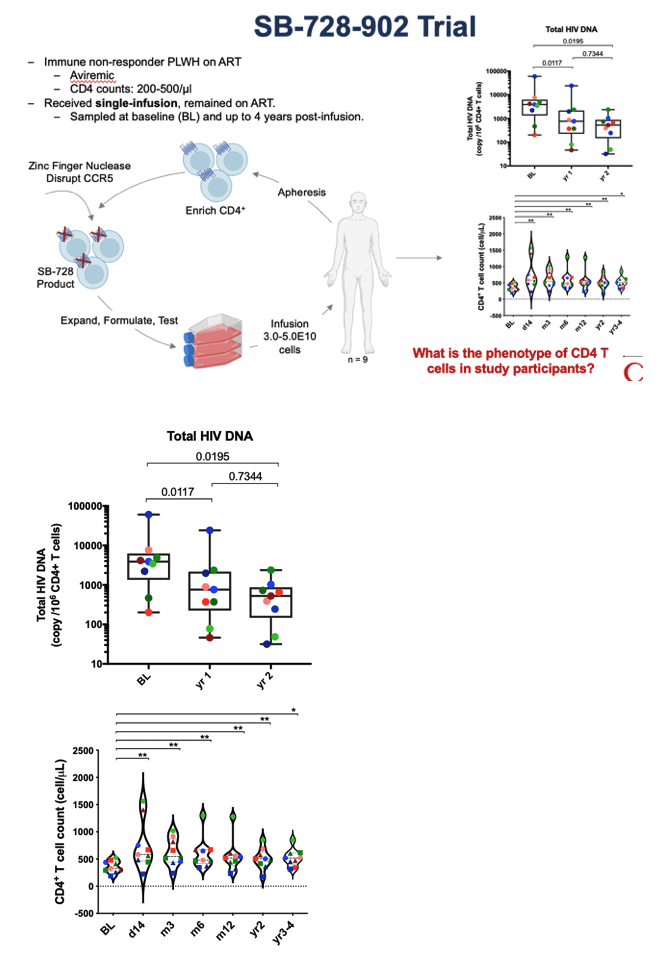
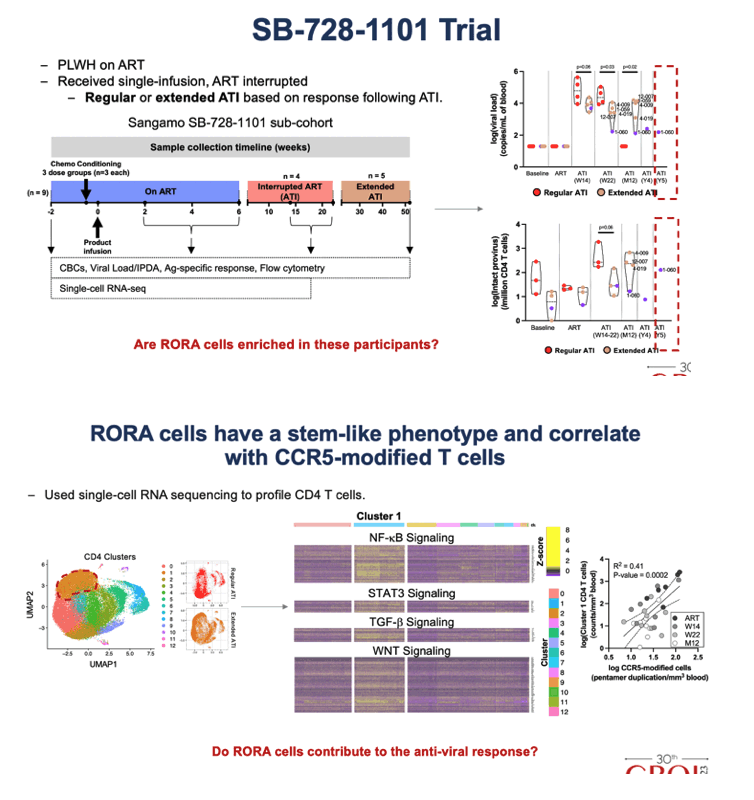
Methods: We performed two clinical studies, SB-728-902 (n = 9) and SB-728-1101 (n = 9), in which participants were provided a single infusion of autologous CCR5-modified T cells and ART was either maintained or interrupted (ATI), respectively. At 3-6 timepoints over 6 years, we collected blood samples and comprehensively profiled the immune response using multi-parameter flow cytometry and single-cell RNA sequencing.
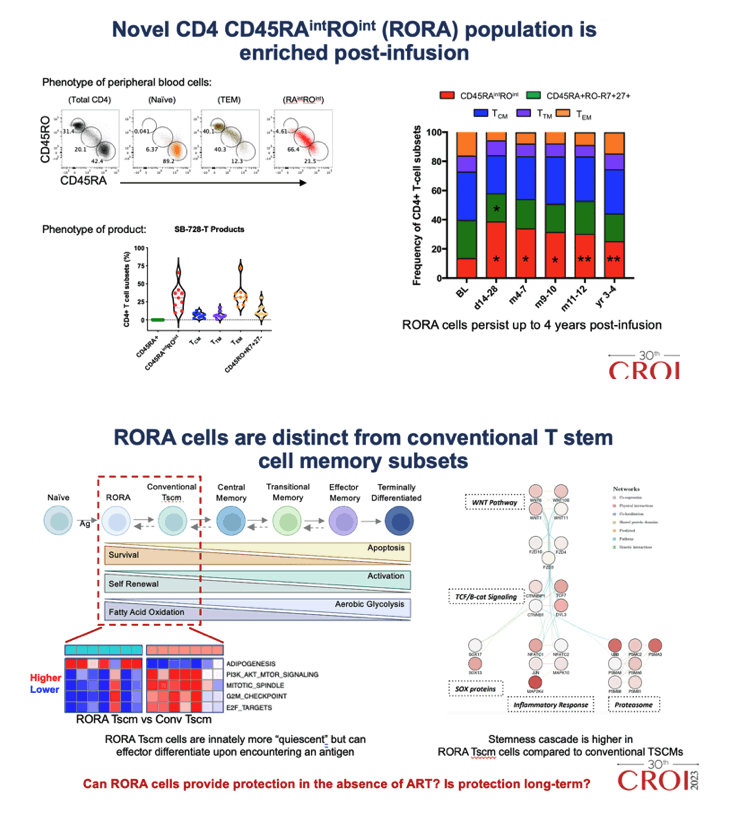
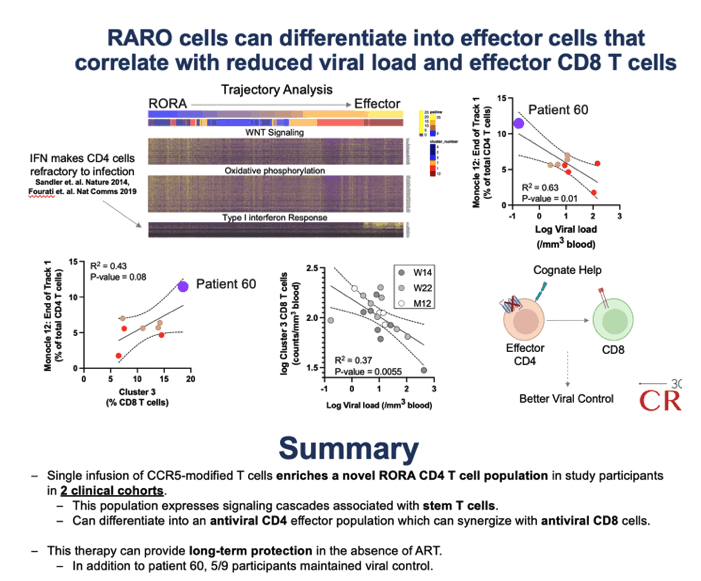
Results: A single infusion of autologous CCR5-modified CD4 T cells led to significant increase in absolute CD4 T cell count (+162 cells/μL, P = 0.02), reduced integrated HIV DNA (P = 0.004) in patients on ART (SB-728-902) and control of plasma viremia (for 1 to 6 years) upon ATI in 5 participants (SB-728-1101). These outcomes were associated with high frequencies of CCR5-modified CD45RAintCD45ROint CD4 T cells that had a quiescent metabolic profile (high oxidative phosphorylation) and were enriched in pathways/markers that regulate stemness (i.e., TCF1 protein, WNT/β-catenin signaling and TGF-β cascades). Single-cell trajectory analyses showed that this population gave rise to an effector CD4 T cell population which expressed high interferon inducible anti-viral genes. Higher frequencies of this subset were associated with both heightened effector CD8 T cell responses and reduced viral load.
Conclusion: Our results indicate that a single infusion of autologous CCR5-modified CD4 T products that are enriched in the novel CD45RAintCD45ROint stem-like phenotype are protected against HIV "re-infection" because they express mutated CCR5, which favors this anti-viral signature. This protection from infection promotes long-lasting effector CD4/8 T cell responses that can control viremia and facilitate a functional cure against HIV.

about 126 CD4 increase in participants from baseline "therapy inducing immune response resulting in reduction in reservoir".

|
| |
|
 |
 |
|
|