 |
 |
 |
| |
LIVER STEATOSIS AND FIBROSIS IN WOMEN WITH HIV BY INTEGRASE INHIBITOR USE
|
| |
| |
CROI 2023 Feb 20-23
Cecile D. Lahiri1, Michael A. Yu 1, Logan G. Gerig2, C. Christina Mehta1, Joffi Musonge-Effoe1, Jennifer C. Price3, Phyllis C. Tien3, Amanda B. Spence4, Svenja Albrecht5,
Maria L. Alcaide6, Adaora A. Adimora7, Audrey L. French8,Michael H. Augenbraun9, Kathryn Anastos10, Jessica A. Alvarez1
1Emory University School of Medicine, Atlanta, GA, USA; 2Emory University, Rollins School of Public Health, Atlanta, GA, USA; 3University of California San Francisco School of Medicine,, San Francisco, CA, USA; 4Georgetown University Medical Center, Washington, DC, USA; 5University of Mississippi Medical Center, Jackson, MS, USA;
6University of Miami, Miller School of Medicine, Miami, FL, USA; 7University of North Carolina School of Medicine, Chapel Hill, NC, USA; 8Stroger Hospital of Cook County Health, Chica


program abstract
Background: Nonalcoholic fatty liver disease is prevalent in persons with HIV and can lead to hepatic fibrosis. Integrase strand-transfer inhibitors (INSTIs), first-line agents in antiretroviral therapy (ART), are associated with increased body mass index (BMI), particularly in women with HIV (WWH). We evaluated hepatic steatosis and fibrosis in WWH who did and did not switch to INSTIs.
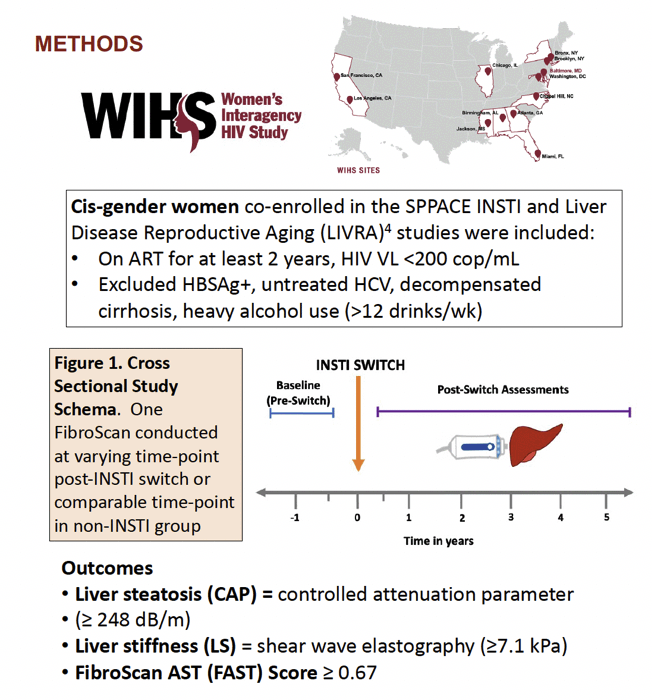
vMethods: We used clinical and FibroScan data collected between 2014-2018 in virally-suppressed WWH enrolled in the Liver Disease and Reproductive Aging substudy of the Women’s Interagency HIV Study. WWH who switched to or added an INSTI to ART were included if they had clinical data and a FibroScan obtained post-switch and compared to women on non-INSTI ART
(Control). Follow-up time was defined as time since switch visit (or comparable visit in Controls). Outcomes included differences between INSTI and Control group estimates of hepatic steatosis via controlled attenuation parameter
(CAP≥248 dB/m), fibrosis via liver stiffness (LS≥7.1 kPa), and steatohepatitis with significant disease activity and fibrosis via FibroScan-aspartate aminotransferase scores (FAST ≥0.67). Adjusted regression and mixed-effects models compared each outcome by group.
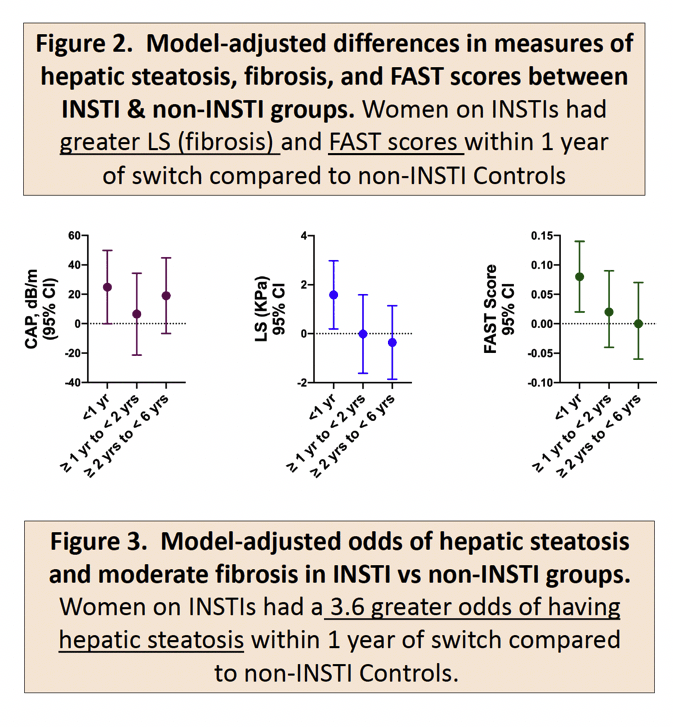
Results: 257 WWH (123 INSTI, 134 Control) were included. Overall, mean age was 50 years (SD 8), 74% were Non-Hispanic Black, BMI was 32 (8) kg/m2, CD4 count was 796 (305) cells/mm3. WWH who switched to INSTIs had a 3.7 greater odds of having hepatic steatosis within 1 year compared to non-INSTI Controls (Table 1), but this difference was not seen at later periods of follow up. The model-adjusted difference between WWH switching to INSTIs vs Controls within 1 year was +1.62 KPa (95% CI 0.24, 2.99) for LS and +0.07 (0.01, 0.13) for FAST scores. However, there was little difference between groups in the odds of having fibrosis and only 4(1.6%) WWH had steatohepatitis by FAST score at any time-point.
Conclusion: WWH switching to INSTIs had a greater odds of having hepatic steatosis but not fibrosis within the 1st year of follow-up compared to women on non-INSTI ART, possibly reflecting early BMI gain with INSTIs. LS and FAST scores in WWH switching to INSTIs were minimally higher at 1 year, but the clinical significance is unclear. A larger study with longitudinal assessments of hepatic steatosis and fibrosis measures is warranted. Patients starting INSTIs need close monitoring of metabolic changes and low thresholds to pursue noninvasive liver fibrosis testing.
Adjusted model estimates of hepatic steatosis and fibrosis differences between groups





|
| |
|
 |
 |
|
|