 |
 |
 |
| |
Cocaine Tied to White Matter Lesions With HIV, a Factor in Poor Cognitive Function
|
| |
| |
30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle
Mark Mascolini
Cocaine use in a study of 110 people with HIV predicted white matter lesion burden, and lesion burden correlated with worse cognitive function [1]. These lesions, also called white matter intensities, signal diffuse small-vessel disease in the brain, reflecting decreased blood flow.

Duke University researchers who ran this prospective MRI-based study noted that cocaine use prevalence runs high in certain HIV populations. This potent central nervous system stimulant appears to boost stroke risk in people with and without HIV.
The Duke team recruited 110 adults with chronic HIV infection from infectious disease clinics in the Durham, North Carolina area. Participants had to be taking antiretroviral therapy and have an undetectable viral load. The researchers excluded perinatally infected people and those with a major neurologic disorder, head trauma, severe mental illness, systemic autoimmune disease, or treatment with immunomodulatory drugs. They divided the study group in cocaine users (a history of regular use or any use in the past 90 days) and nonusers (no history of regular use and 0 days of use in the past 90 days).
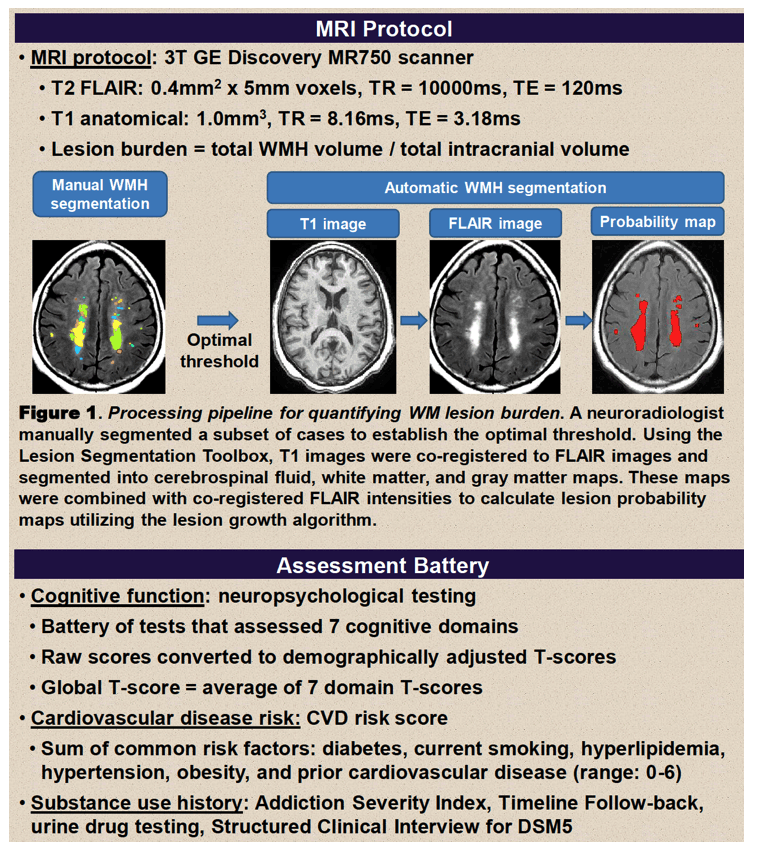
Neuropsychological testing included an array of tests that assessed 7 cognitive domains, yielding raw scores that were converted to demographically adjusted T scores. A global T score represented the average of the 7 domain T scores. Cardiovascular risk score summed common risk factors such as diabetes, current smoking, and hypertension. Magnetic resonance imaging (MRI) spotted white matter hyperintensities. Lesion burden equaled total white matter hyperintensity volume divided by total intracranial volume.
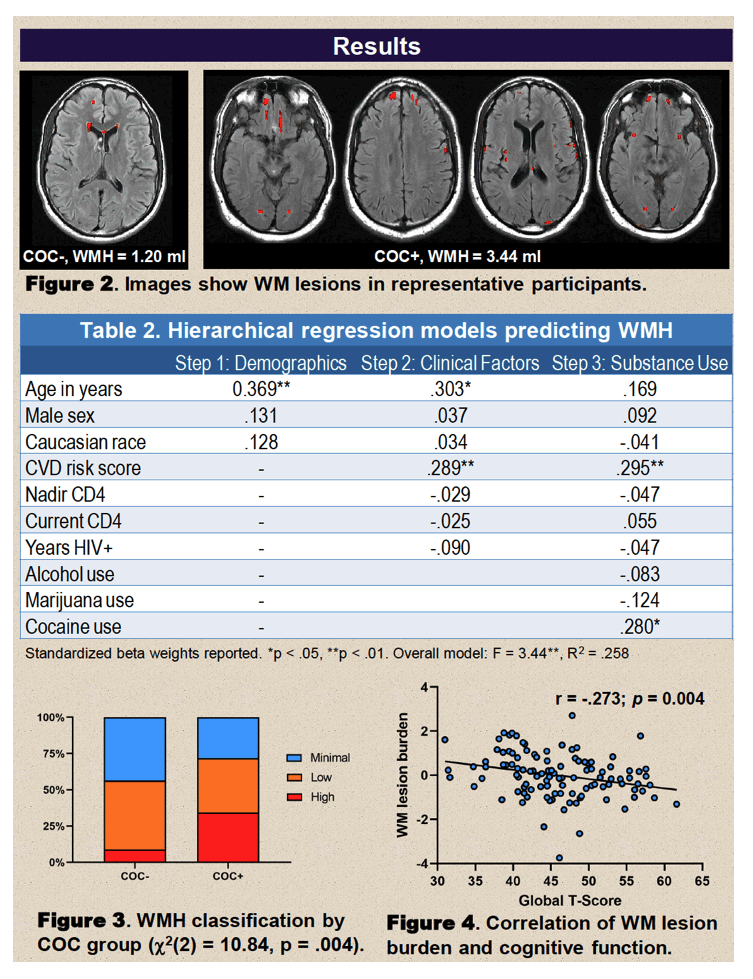
Average age was significantly older in the 32 cocaine users than in the 78 nonusers (50.0 vs 43.5, P < 0.01). The groups did not differ significantly in proportion of women (18.7% and 20.5%), average years since HIV diagnosis (15.0 and 14.4), or cardiovascular disease risk score (1.78 and 1.47). But the cocaine-using group had a significantly higher proportion of blacks (87.5% vs 70.5%, P < 0.001), significantly fewer years of education (12.7 vs 14.3, P = 0.002), and a significantly lower nadir CD4 count (76 vs 238, P = 0.002) and current CD4 count (460 vs 814, P < 0.001). The cocaine group averaged 18.3 years of regular cocaine use and used cocaine 23.8 days in the past 90 days.
A hierarchical regression model adjusted for age, sex, race, and cardiovascular disease risk identified cocaine use as a significant predictor of white matter hyperintensities (beta 0.280, P < 0.05), as was cardiovascular risk score (beta 0.295, P < 0.01). White matter lesion burden correlated inversely with global cognitive function-the greater the white lesion burden, the worse the cognitive function (r = -0.273, P = 0.004).
The Duke team believes their findings "underscore the importance of reducing cocaine use in people with HIV to minimize additional white matter lesions that may exacerbate neurocognitive impairment."
Reference
1. Meade CS, Bell RP, Towe SL, Lascola CD. Cocaine use independently predicts white matter lesion burden in HIV disease. 30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle. Abstract 466.
[ from Jules. White matter hyperintensities (WMHs) are brain white matter lesions that are hyperintense on fluid attenuated inversion recovery (FLAIR) magnetic resonance imaging (MRI) scans. Larger WMH volumes have been associated with Alzheimer's disease (AD) and with cognitive decline. White matter hyperintensities (WMHs) are commonly seen on brain MRI in older people, and result from chronic ischaemia associated with cerebral small vessel disease; white matter hyperintensities are more common and extensive in patients with cardiovascular risk factors and symptomatic cerebrovascular disease. White matter hyperintensities proliferate as the brain ages and are associated with increased risk for cognitive decline as well as Alzheimer's disease and related dementias. As such, white matter hyperintensities have been targeted as a surrogate biomarker in intervention trials with older adults. Our results demonstrate that a link between white matter hyperintensities and early signs of cognitive decline is detectable decades before clinical symptoms of dementia emerge. Thus, white matter hyperintensities may be a useful surrogate biomarker for identifying individuals in midlife at risk for future accelerated cognitive decline and selecting participants for dementia prevention trials. While WMHs are uncommon in adults before age 30 (Habes et al., 2016), they are detectable in <90% of individuals by age 65 (Longstreth et al., 1996). In older adults, WMHs are associated with multiple dementia risk factors, including increasing age, hypertension, stroke, brain atrophy and cognitive ability (Prins and Scheltens, 2015). Longitudinal studies in older adults have reported that the spread of WMHs contributes to elevated risk for ADRD and coincides with age-related cognitive decline (Debette and Markus, 2010). Furthermore, baseline WMH load at mean age 62 can predict the onset of dementia up to 20 years later (Coker et al., 2019).https://academic.oup.com/braincomms/article/1/1/fcz041/5670525 ]




|
| |
|
 |
 |
|
|