 |
 |
 |
| |
COVID in US Made HIV Diagnoses Plunge in 2020-But Why?
|
| |
| |
30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle

Mark Mascolini
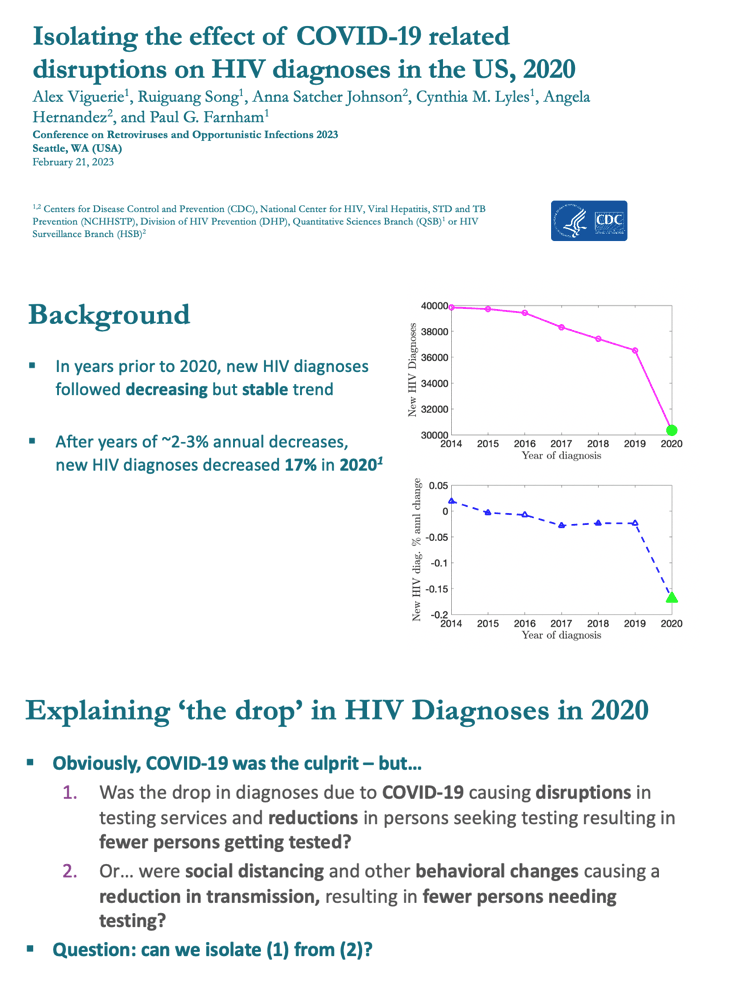
From 2015 to 2019, new diagnoses of HIV infection in the United States dwindled at a steady rate of about 2.3% yearly, researchers from the Centers for Disease Control and Prevention (CDC) estimated [1]. Then, in 2020, the new-diagnosis rate (incidence) stepped off a cliff, plunging 17%.
The arrival of COVID-19 clearly explained this startling statistic, the CDC team said, but why? Did the immense COVID-induced disruption in healthcare services upset testing for HIV and other conditions so much that thousands fewer got an HIV test, so thousands fewer got diagnosed? Or did behavioral changes-including fear-inspired social distancing-slice HIV transmissions so much that thousands fewer got infected? CDC investigators aimed to see if they could figure which explanation makes more sense.
They began with the epidemiologic nugget that two thirds of people who test positive for HIV get diagnosed 1 year or more after getting infected. CD4 counts measured at diagnosis can help estimate time since infection, and the CDC uses CD4 count to estimate HIV incidence. With these facts in hand, the investigators tried to approach the COVID-HIV diagnosis conundrum by counting HIV infections acquired in 2010-2019 that were not diagnosed in 2020 because of COVID-related healthcare disruptions but should have been diagnosed based on prior patterns. They called these missed HIV detections excess missed diagnoses.
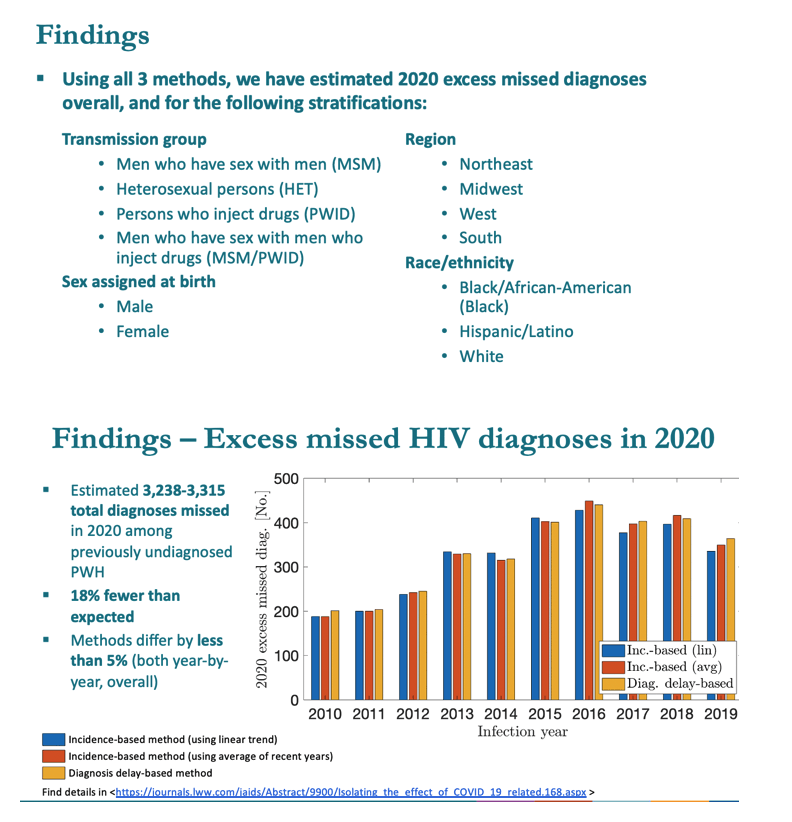
Next the CDC team devised three statistical methods that would let them estimate total 2020 excess missed diagnoses-based on patterns seen from 2010 through 2019-as well as excess missed diagnoses for each HIV transmission group, for female or male sex assigned at birth, for four US regions (Northeast, Midwest, West, South), and for three race/ethnicity groups (black, Hispanic, and white).
These three methods estimated 3238 to 3315 total HIV diagnoses missed in 2020 among previously undiagnosed people infected in 2010-2019. These 3300 missed diagnoses represent 18% fewer than expected HIV diagnoses in 2020. The three statistical methods proved highly consistent in figuring excess missed HIV diagnoses, with less than 5% difference year by year and overall.
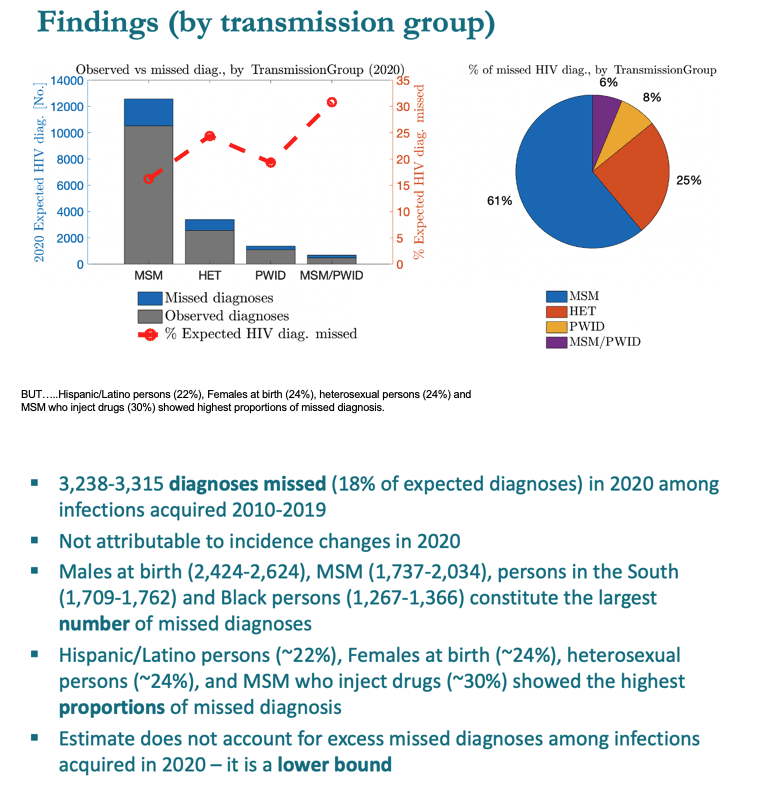
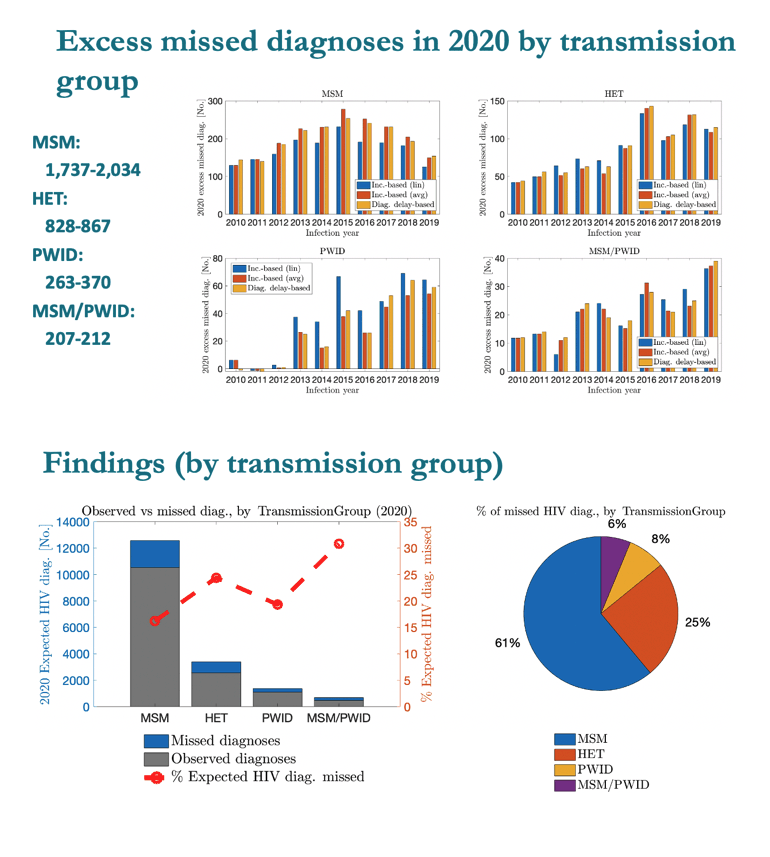
The prediction tools estimated 1737 to 2034 excess missed diagnoses in 2020 for men who have sex with men (MSM), 828 to 867 for people infected heterosexually, 263 to 370 for people who inject drugs, and 207 to 212 for MSM who inject drugs.
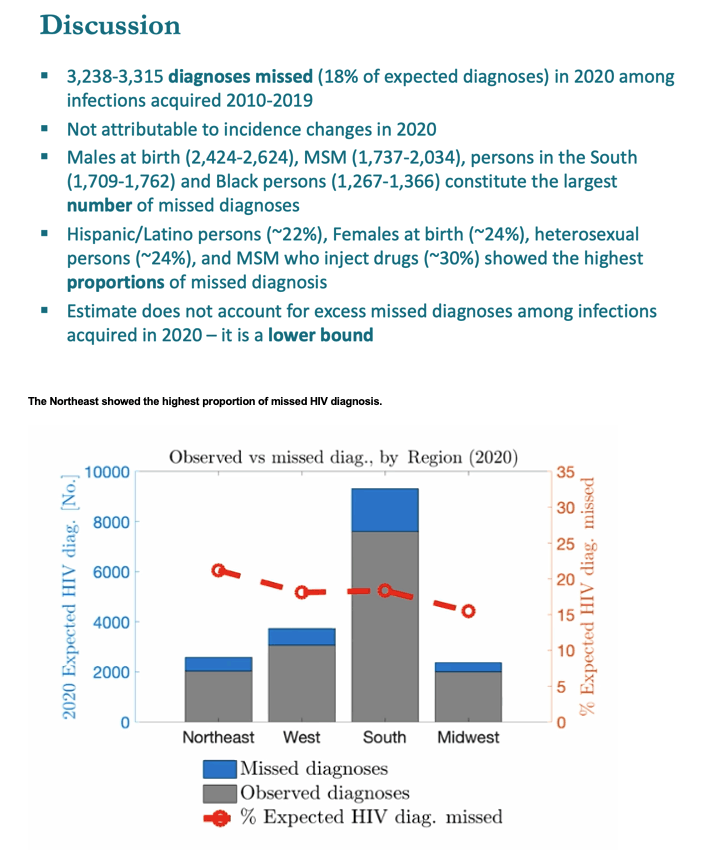
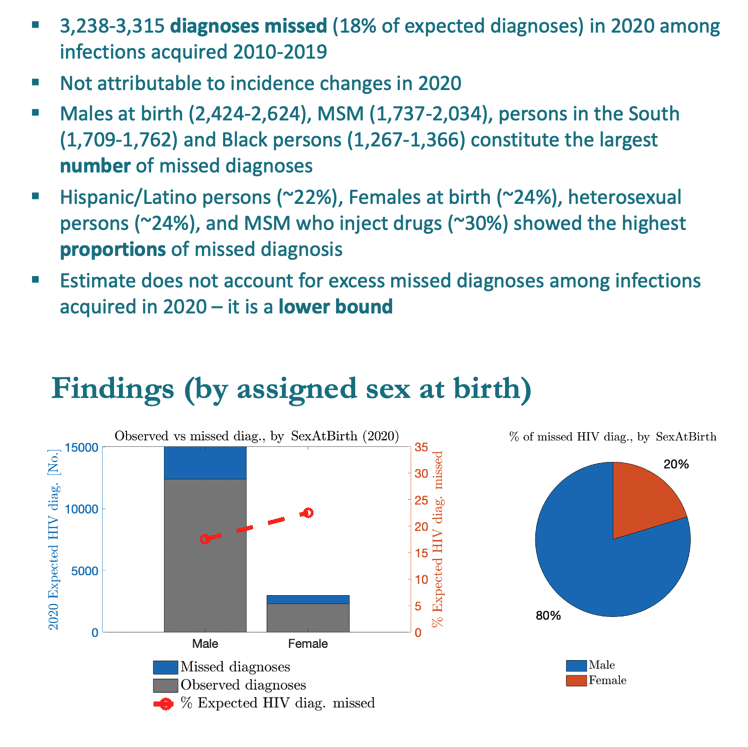
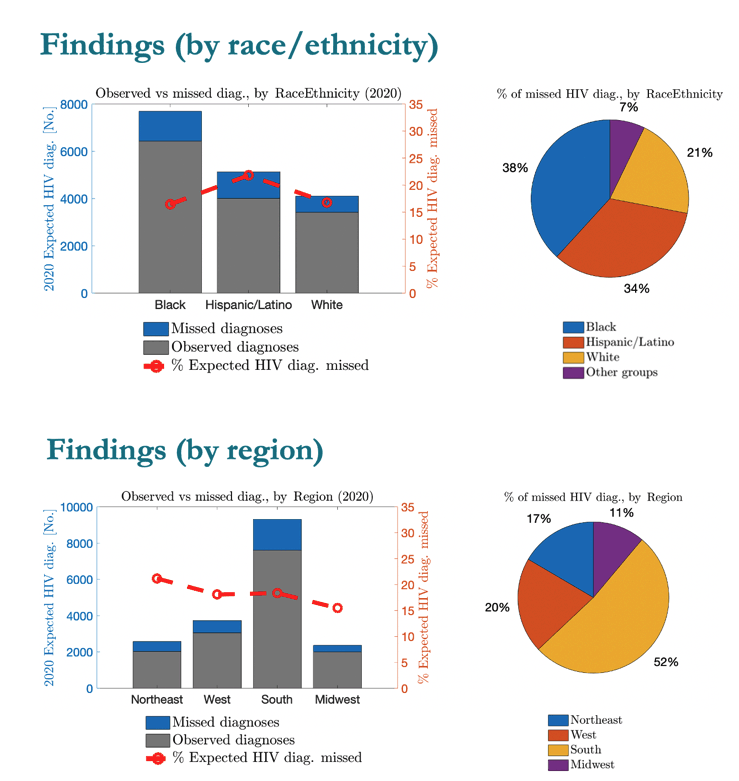
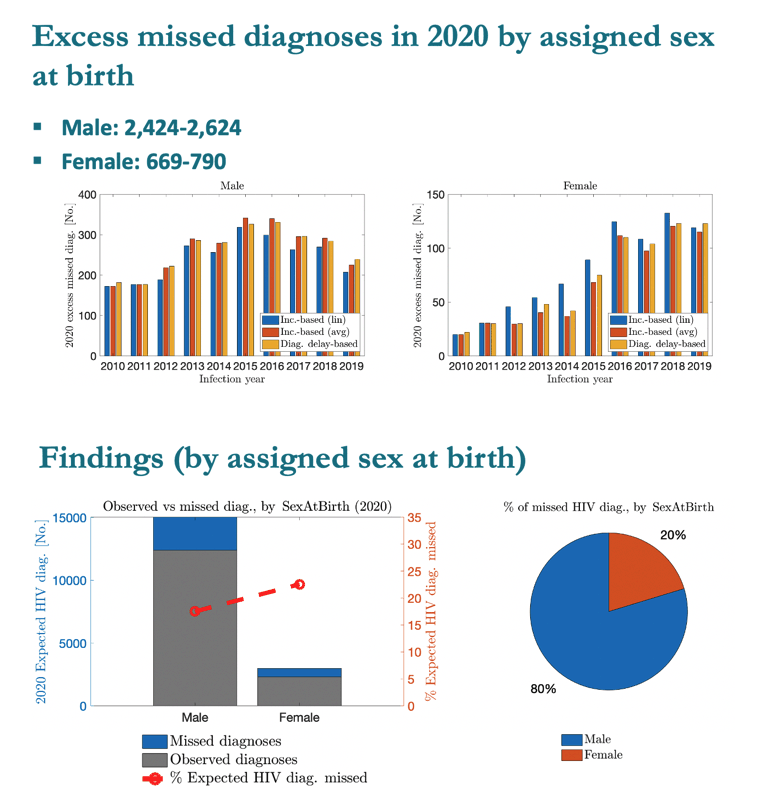
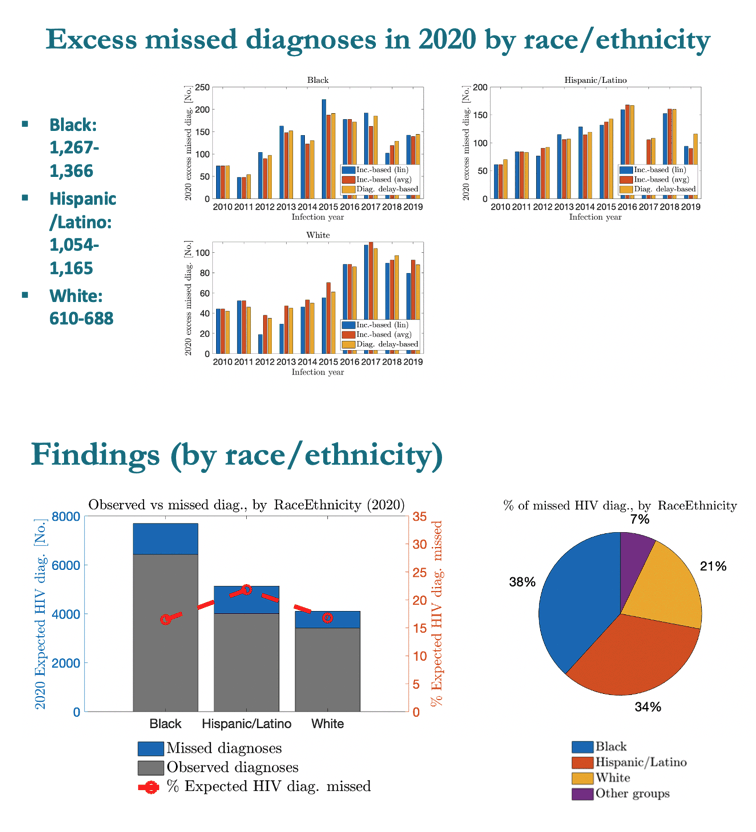
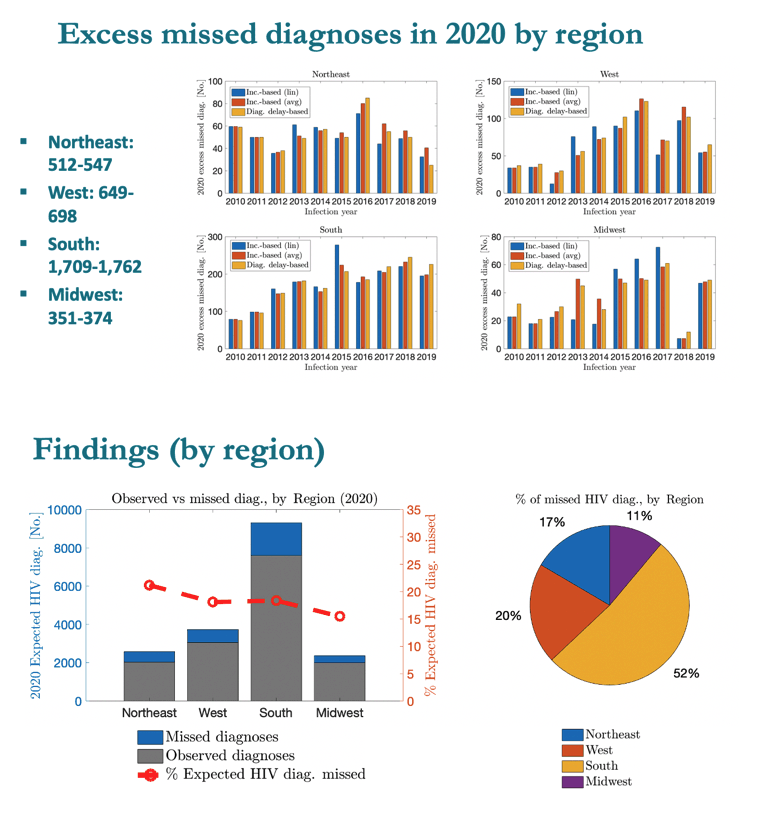
MSM accounted for 61% of excess missed HIV diagnoses, heterosexuals for 25%, people who inject drugs for 8%, and MSM who inject drugs for 6%. People assigned male sex at birth made up 80% of excess missed diagnoses and people assigned female 20%. By race or ethnicity, blacks accounted for 38% of excess missed diagnoses, Hispanics for 34%, whites for 21%, and other groups for 7%. More than half of excess missed diagnoses, 52%, occurred in the US South, 20% in the West, 17% in the Northeast, and 11% in the Midwest.
While MSM compromised the largest number (61%), MSM were the least likely on a per group basis to miss diagnosis, followed by heterosexuals, and PWID & MSM/PWD were proportionally the most likely to miss diagnosis.
BUT ......excess risk is highest in Northeast followed by West & South and then the Midwest.
Females at birth had a substantially higher proportionally missed diagnosis, whites a d Blacks wee less and about the same.
Hispanics showed a notably higher proportionally missed diagnosis.
The CDC team concluded that, among people infected with HIIV in 2010 through 2019, about 3300 HIV diagnoses were missed in 2020, representing 18% of expected diagnoses based on infections acquired from 2010 through 2019. These missed diagnoses cannot be attributed to changes in HIV incidence, the CDC investigators said. They can only be attributed to changes in testing patterns, that is, “a combination of disruption in testing services and reductions in testing behaviors” resulting from the advent of COVID-19 in the United States.
The researchers reminded CROI attendees that the longer time to HIV diagnoses indicated by their calculations inevitably results in lower population viral suppression rates and thus increased HIV transmission. They stressed that “identifying undiagnosed persons with HIV though increased testing efforts is necessary to maintain progress” toward HIV elimination goals.
Reference
1. Viguerie A, Song R, Johnson AS, Lyles C, Hernandez A, Farnham P. Isolating the effect of COVID-19 related disruption on HIV diagnoses in the US, 2020. 30th CROI, Conference on Retroviruses and Opportunistic Infections, February 19-22, 2023, Seattle. Abstract 158.



|
| |
|
 |
 |
|
|