| |
Pitavastatin to Prevent Cardiovascular Disease in HIV Infection
|
| |
| |
Download the PDF here
Download the PDF here
for the REPRIEVE Investigator
Abstract
Background
The risk of cardiovascular disease is increased among persons with human immunodeficiency virus (HIV) infection, so data regarding primary prevention strategies in this population are needed.
Methods
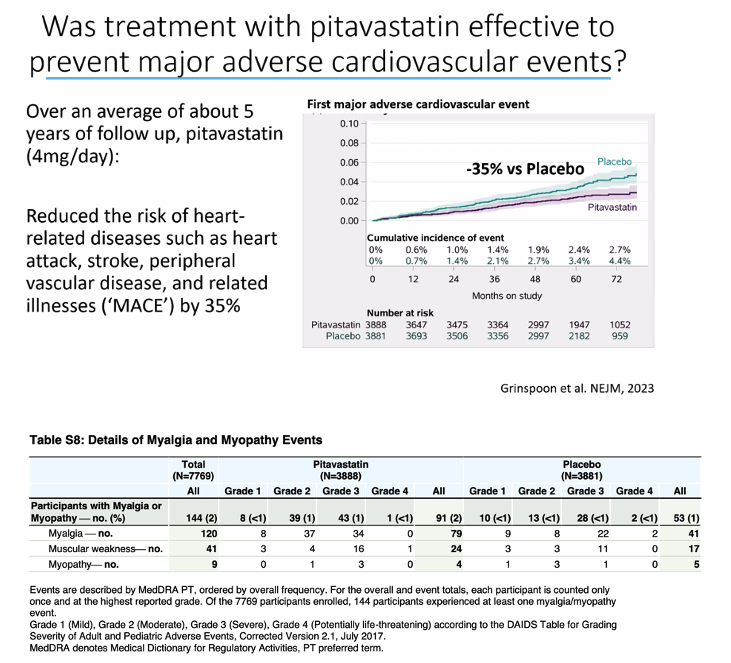
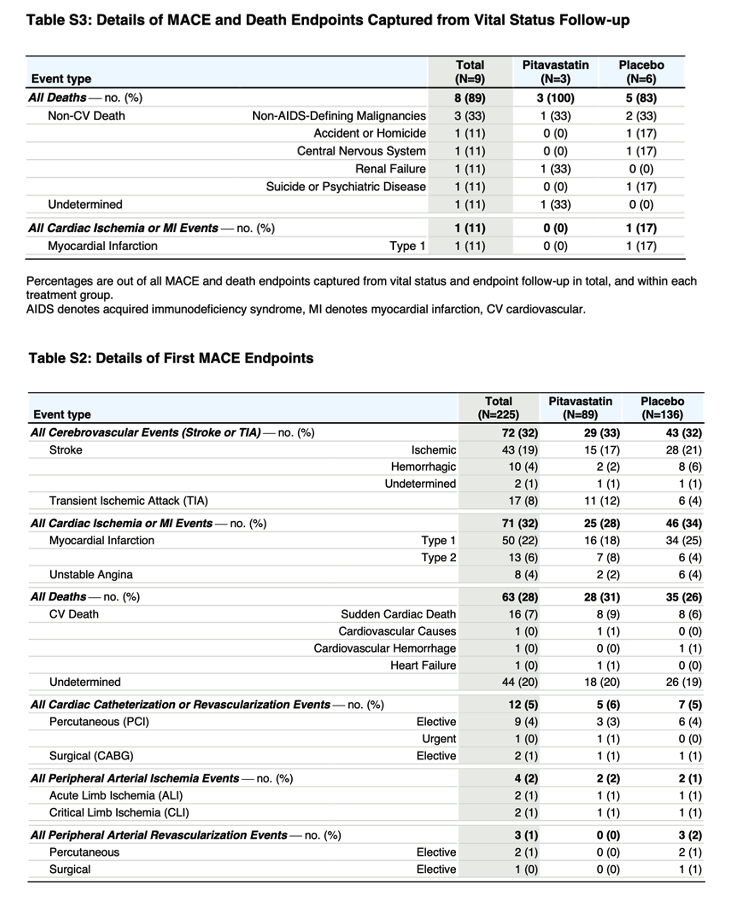
In this phase 3 trial, we randomly assigned 7769 participants with HIV infection with a low-to-moderate risk of cardiovascular disease who were receiving antiretroviral therapy to receive daily pitavastatin calcium (at a dose of 4 mg) or placebo. The primary outcome was the occurrence of a major adverse cardiovascular event, which was defined as a composite of cardiovascular death, myocardial infarction, hospitalization for unstable angina, stroke, transient ischemic attack, peripheral arterial ischemia, revascularization, or death from an undetermined cause.
Results
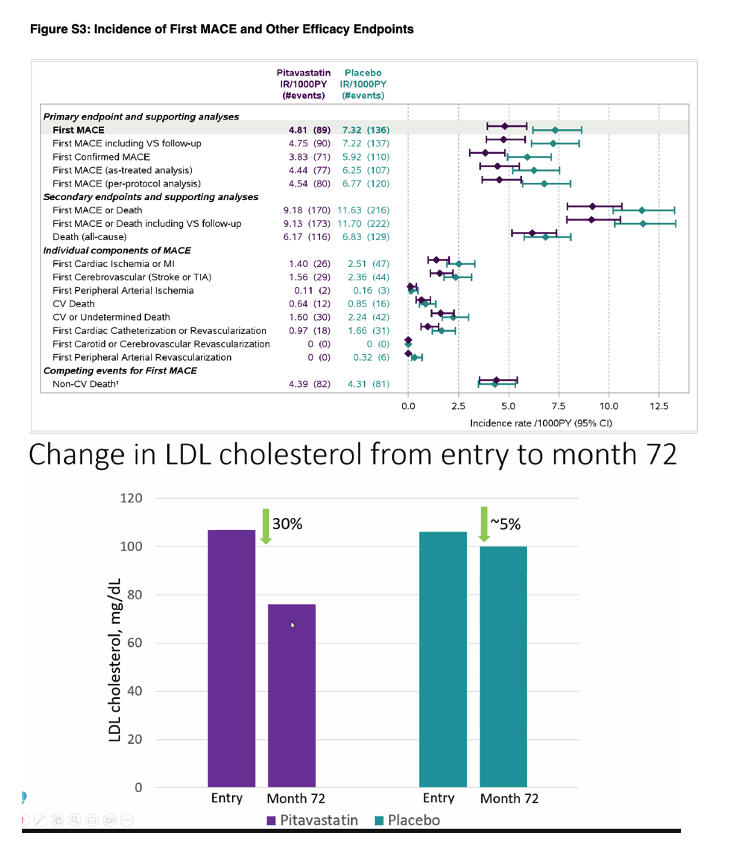
The median age of the participants was 50 years (interquartile range, 45 to 55); the median CD4 count was 621 cells per cubic millimeter (interquartile range, 448 to 827), and the HIV RNA value was below quantification in 5250 of 5997 participants (87.5%) with available data. The trial was stopped early for efficacy after a median follow-up of 5.1 years (interquartile range, 4.3 to 5.9). The incidence of a major adverse cardiovascular event was 4.81 per 1000 person-years in the pitavastatin group and 7.32 per 1000 person-years in the placebo group (hazard ratio, 0.65; 95% confidence interval [CI], 0.48 to 0.90; P=0.002). Muscle-related symptoms occurred in 91 participants (2.3%) in the pitavastatin group and in 53 (1.4%) in the placebo group; diabetes mellitus occurred in 206 participants (5.3%) and in 155 (4.0%), respectively.
Conclusions
Participants with HIV infection who received pitavastatin had a lower risk of a major adverse cardiovascular event than those who received placebo over a median follow-up of 5.1 years. (Funded by the National Institutes of Health and others)
Safety Events
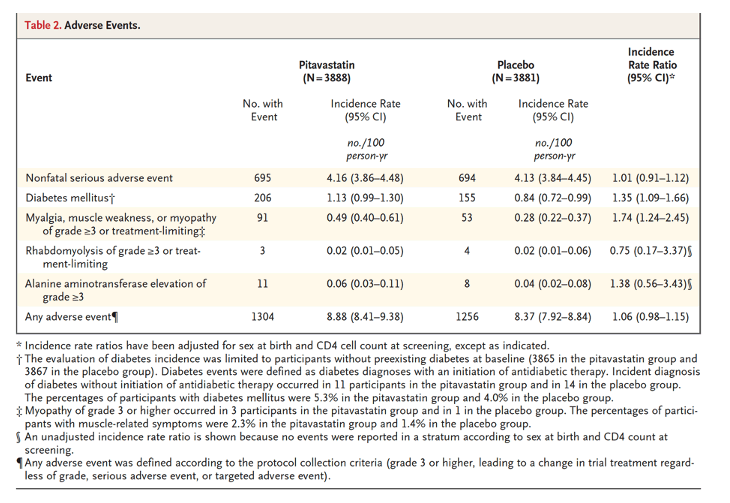
The incidence of nonfatal serious adverse events appeared to be similar in the two groups (Table 2 and Tables S6 and S7). Among targeted adverse events, a higher rate of diabetes mellitus was seen in the pitavastatin group (incidence rate ratio, 1.35; 95% CI, 1.09 to 1.66). One participant in the pitavastatin group and two in the placebo group withdrew because of the development of diabetes mellitus. There was no apparent treatment effect on glucose levels (Fig. S6).
A higher frequency of myalgia or myopathy with a severity of grade 3 or higher or that resulted in a change in treatment occurred in the pitavastatin group (incidence rate ratio, 1.74; 95% CI, 1.24 to 2.45). The majority of muscle-related symptoms in the two groups were myalgias and low-grade muscle weakness with a low incidence of myopa-thy (Table S8 and Fig. S7). Muscle-related symp-toms led to withdrawal in 44 participants (1.1%) in the pitavastatin group and in 21 (0.5%) in the placebo group. Myopathy, rhabdomyolysis, and liver dysfunction (grade 3 or higher ALT level) occurred rarely and had similar frequencies in the two groups.
| |
| |
| |
|
|
|