| |
Analysis of Severe Illness After Postvaccination COVID-19 Breakthrough Among Adults With and Without HIV in the US - CD4 <350 Increased Risk for Post Vaccine Severe Breakthrough
|
| |
| |
Download the PDF here
Prior CIVETs collaboration analyses4 showed a 28% increase in breakthrough COVID-19 among PWH vs PWoH. The findings of this cohort study showed that the risk of severe illness (requiring hospitalization) after COVID-19 breakthrough was low (6.8% of 3649 vaccinated PWH and PWoH) and did not differ by HIV status overall. PWH with lower CD4 cell counts (<350 cells/μL), however, had higher risk of severe COVID-19 breakthrough illness compared with PWoH, suggesting a role of immune dysfunction in the increased risk. The lack of difference in severe COVID-19 breakthrough illness risk between PWoH and PWH with higher CD4 cell counts may be associated with engagement in medical care, different health care-seeking behaviors, and reduced comorbidities among the PWH included compared with PWoH. The increased risk of severe COVID-19 breakthrough illness for PWH with moderate immune suppression (ie, CD4 cell count 200-349 cells/μL)27 (1) suggests that the recommendation for additional primary series vaccination doses should be expanded to PWH with moderate immune suppression, (2) supports the current recommendation of a first booster, and (3) suggests counseling on risk-reduction strategies among those with moderate immune suppression.
earlier publication
Greater risk of post-vaccination breakthrough severe COVID-19 illness in people with HIV and CD4 <350 - (06/13/22)
Key Points
Question - In 2021, among fully vaccinated people with breakthrough COVID-19 illness, was the risk of severe illness higher for people with HIV (PWH) compared with people without HIV (PWoH)?
Findings - In this cohort study of 3649 patients with breakthrough COVID-19, there was no overall difference in risk of severe disease between PWH and PWoH. PWH with CD4 cell count less than 350 cells/μL had a 59% increased risk of severe breakthrough illness compared with PWoH.
Meaning - Although vaccinations effectively reduce the risk of severe COVID-19 illness in both PWH and PWoH, these findings suggest that PWH with moderate or severe immune suppression (CD4 cell count <350 cells/μL) could be at higher risk of severe breakthrough infection compared with PWoH, and PWH with moderate immune suppression should be considered for additional vaccine dosages and other risk-reduction measures.
Current US Centers for Disease Control and Prevention (CDC) guidelines recommend risk reduction behaviors (ie, mask wearing), an additional COVID-19 primary series vaccine dose, and a second booster dose for PWH with "advanced or untreated HIV infection."21,22 PWH with partially recovered CD4 cell counts (>200 cells/μL) and moderate immune suppression are not currently recommended for an additional or second booster dose. Our objective was to determine whether HIV infection was associated with increased severe COVID-19 illness among fully vaccinated adults with a breakthrough SARS-CoV-2 infection and to identify the factors associated with severe COVID-19 breakthrough illness among PWH, including level of immune suppression and HIV viral replication.
Abstract
Importance Understanding the severity of postvaccination SARS-CoV-2 (ie, COVID-19) breakthrough illness among people with HIV (PWH) can inform vaccine guidelines and risk-reduction recommendations.
Objective To estimate the rate and risk of severe breakthrough illness among vaccinated PWH and people without HIV (PWoH) who experience a breakthrough infection.
Design, Setting, and Participants In this cohort study, the Corona-Infectious-Virus Epidemiology Team (CIVET-II) collaboration included adults (aged ≥18 years) with HIV who were receiving care and were fully vaccinated by June 30, 2021, along with PWoH matched according to date fully vaccinated, age group, race, ethnicity, and sex from 4 US integrated health systems and academic centers. Those with postvaccination COVID-19 breakthrough before December 31, 2021, were eligible.
Exposures HIV infection.
Main Outcomes and Measures The main outcome was severe COVID-19 breakthrough illness, defined as hospitalization within 28 days after a breakthrough SARS-CoV-2 infection with a primary or secondary COVID-19 discharge diagnosis. Discrete time proportional hazards models estimated adjusted hazard ratios (aHRs) and 95% CIs of severe breakthrough illness within 28 days of breakthrough COVID-19 by HIV status adjusting for demographic variables, COVID-19 vaccine type, and clinical factors. The proportion of patients who received mechanical ventilation or died was compared by HIV status.
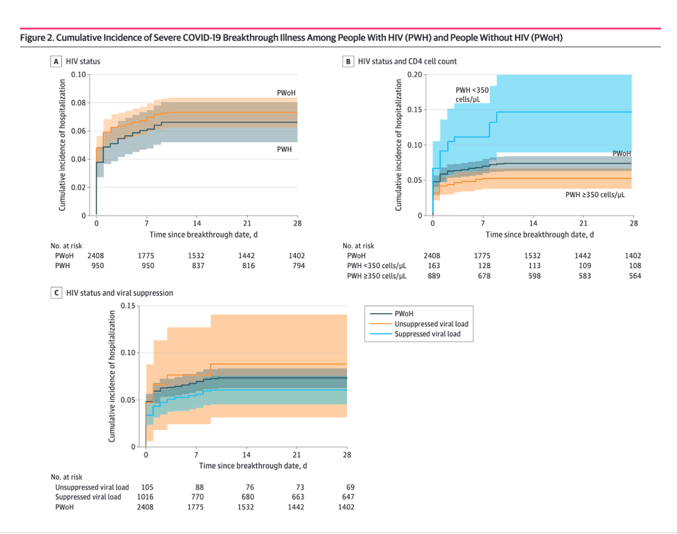
Results Among 3649 patients with breakthrough COVID-19 (1241 PWH and 2408 PWoH), most were aged 55 years or older (2182 patients [59.8%]) and male (3244 patients [88.9%]). The cumulative incidence of severe illness in the first 28 days was low and comparable between PWoH and PWH (7.3% vs 6.7%; risk difference, -0.67%; 95% CI, -2.58% to 1.23%). The risk of severe breakthrough illness was 59% higher in PWH with CD4 cell counts less than 350 cells/μL compared with PWoH (aHR, 1.59; 95% CI, 0.99 to 2.46; P = .049). In multivariable analyses among PWH, being female, older, having a cancer diagnosis, and lower CD4 cell count were associated with increased risk of severe breakthrough illness, whereas previous COVID-19 was associated with reduced risk. Among 249 hospitalized patients, 24 (9.6%) were mechanically ventilated and 20 (8.0%) died, with no difference by HIV status.
Conclusions and Relevance In this cohort study, the risk of severe COVID-19 breakthrough illness within 28 days of a breakthrough infection was low among vaccinated PWH and PWoH. PWH with moderate or severe immune suppression had a higher risk of severe breakthrough infection and should be included in groups prioritized for additional vaccine doses and risk-reduction strategies.
|
|
| |
| |
|
|
|