| |
Sex and Race Disparities in Mortality and Years of
Potential Life Lost Among People With HIV:
A 21-Year Observational Cohort Study
|
| |
| |
Download the PDF here
Jan 2023
Comment: I don't think the authors did a good job explaining what these statistics mean. I think the main issue is that, from this, we can't estimate the years lost for a single person, so it's hard to interpret. What we really want to know is how many years does HIV take off your life and how many year does it differ in two people in different demographic groups (eg black women vs white males).
Our analysis found that of individuals who have died, Black women with HIV were particularly impacted by increased years of potential life lost.
Most health disparities are a result of social determinants of health. Indeed, in our study we observed differences by race and sex with regards to burden of noninfectious comorbidities and health insurance at clinic entry, clinical factors often closely associated with adverse social determinants of health and mortality [25-27].
The challenges experienced by women and Black Americans require an intersectional approach to addressing the social determinants of health that create and reinforce these inequities, and further investigation into how underlying societal and structural determinants of health continue to drive disparities in long-term outcomes of PWH are needed.
Results
Among 6531 individuals (51% non-Hispanic [NH] White race, 40% NH Black race, 21% cis-gender women, 78% cis-gender men) included, 956 (14.6%) died. In adjusted analysis, PWH alive in the most recent calendar era (2014-2018) had decreased risk of mortality compared with those in the earliest calendar era (1998-2003; aIRR, 0.22; 95% CI, 0.17-0.29), and women had increased risk of death compared with men (aIRR, 1.31; 95% CI, 1.12-1.54).
Of those who died, Black women had the highest aYPLL (aIRR, 592.5; 95% CI, 588.4-596.6), followed by Black men(aIRR, 470.7; 95% CI, 468.4-472.9), White women (aIRR, 411.5; 95% CI, 405.6-417.4), then White men (aIRR, 308.6; 95% CI, 308.0-309.2). In adjusted models, higher YPLL remained associated with NH Black race and cis-gender women, regardless of HIV risk factor.
Conclusions
Despite marked improvement over time, sex disparities in mortality as well as sex and race disparities in YPLL remained among PWH in this cohort.
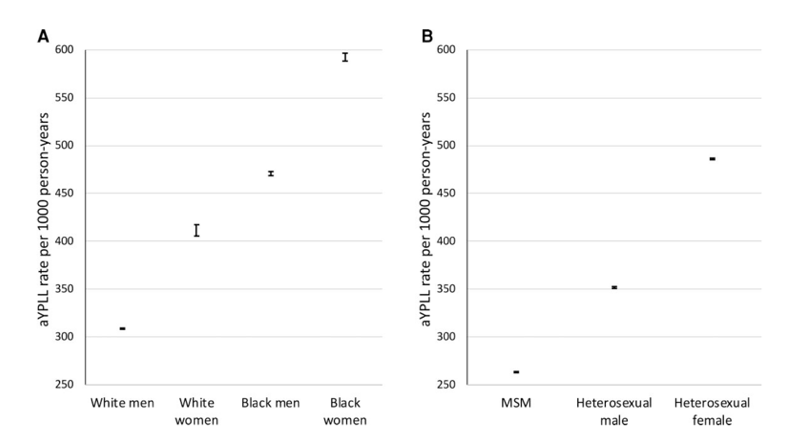
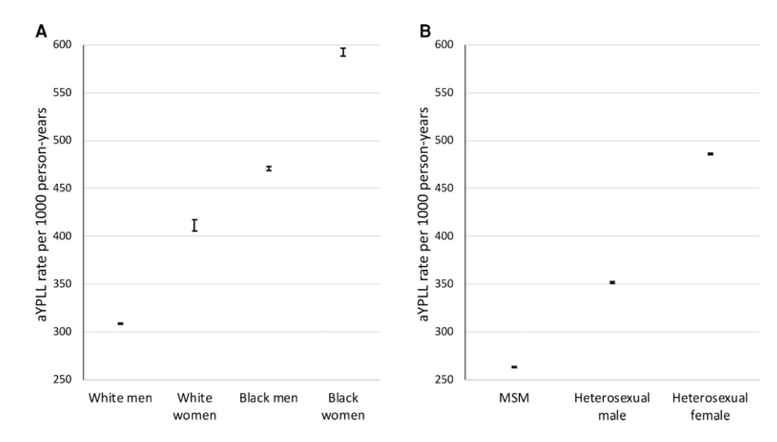
Figure 2. Age-adjusted years of potential life lost rates (95% CI) among individuals cared for at the VCCC who died during the study period (1998-2018), by (A) sex and race/ethnicity and (B) HIV acquisition risk factor. Abbreviations: aYPLL, age-adjusted years of potential life lost; MSM, men who have sex with men; VCCC, Vanderbilt Comprehensive Care Clinic
Years of Potential Life Lost
For the premature mortality analysis, 96 individuals, 29 of whom died during the study period, did not have a date of HIV diagnosis available and were excluded, leaving 6435 individuals and a total of 927 deaths available for YPLL analyses. Age-standardized YPLL per 1000 person-years were significantly higher for females than males (606.9; 95% CI, 604.7-609.1; vs 366.8; 95% CI, 365.8-367.9). Overall, aYPLL were higher for non-Hispanic Black individuals compared with non-Hispanic White individuals (509.7; 95% CI, 508.2-511.2; vs 395.1; 95% CI, 393.1-397.2). Crude YPLL results are shown in Supplementary Table 3. When the cohort was stratified by race/ethnicity and sex, Black women had the highest aYPLL (592.5; 95% CI, 588.4-596.6), followed by Black men (470.7; 95% CI, 468.4-472.9), White women (411.5; 95% CI, 405.6-417.4), and lastly White men (308.6; 95% CI, 308.0-309.2) (Figure 2). For these calculations, 55 White women in the ≥50-years age group were excluded because their years of life lost was greater than the person-years they contributed after HIV diagnosis, artifactually yielding negative aYPLL for this group. Furthermore, after excluding those with unknown or other HIV risk factors, aYPLL were higher for heterosexual women (486.1; 95% CI, 485.2-486.9) than for men regardless of their sexual HIV acquisition risk factor. Among men, heterosexual men had higher aYPLL when compared with men who have sex with men (351.8; 95% CI, 350.9-352.7; vs 263.3; 95% CI, 262.7-263.8). In multivariable linear regression (Table 3), after adjusting for age at HIV diagnosis, CD4 cell count at clinic entry, HIV RNA at clinic entry, any history of HCV coinfection, and year of clinic entry, increased YPLL were associated with non-Hispanic Black individuals and cis-gender women, regardless of HIV acquisition risk factor.
as previously reported:
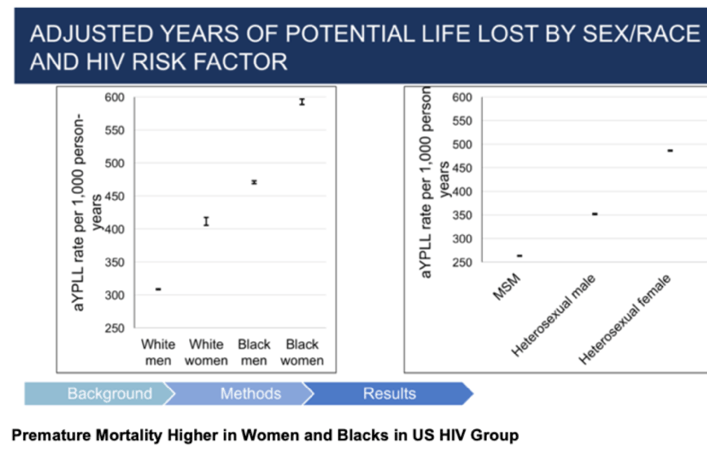
Premature Mortality Higher in Women and Blacks in US HIV Group IDWeek, September 29-October 3, 2021
|
|
| |
| |
|
|
|