| |
Life expectancy after 2015 of adults with HIV on
long-term antiretroviral therapy in Europe and North America:
a collaborative analysis of cohort studies
|
| |
| |
Download the PDF here
Lancet HIV March 2023
Although our analyses suggested that factors related to HIV history are less important than age and CD4 cell count, comorbidities during ART are an important predictor of mortality.
Most deaths in people with HIV on ART in high-income countries are now due to non-AIDS causes such as cancer and cardiovascular disease. These comorbidities are more common in people with HIV than in the HIV-negative population, and their importance will increase as the population of people with HIV continues to age.
Therefore, treatment and prevention of comorbidities in people with HIV is important to ensure the quality of remaining years of life.
Adverse markers related to HIV history, such as very low CD4 cell counts before ART initiation and exposure to regimens that are no longer available because of their side-effect profiles or lower effectiveness, continue to predict mortality much later on. Exposure to ART regimens with poor side-effect profiles could have caused unplanned treatment interruptions, leading to increased long-term mortality. However, the associations between these adverse markers and mortality from 2015 onwards were modest after accounting for factors at the start of follow-up.
Our finding that life expectancy of people with HIV in North America and Europe who have been on ART is only somewhat lower than that in the general population will be reassuring for affected people. Our life-expectancy estimates will also be useful for clinicians and might enable improved access to affordable life insurance policies for people with HIV.
Further research should focus on estimating the quality as well as the quantity of life left for people with HIV, with a particular focus on comorbidities that are more common in people with HIV.
COMMENTARY
Finally, increases in life expectancy are not necessarily associated with improvements in quality of life. Marcus and colleagues showed that insured people with HIV in the USA lived for 6⋅8 years less than a matched cohort of people without HIV, but had 9⋅5 years less without major chronic comorbidities. Cohorts are great resources in which to track these outcomes, and in future should incorporate measures of substance use, quality of life, and chronic pain to measure health-adjusted life expectancy, a more comprehensive measure of the true burden of HIV.
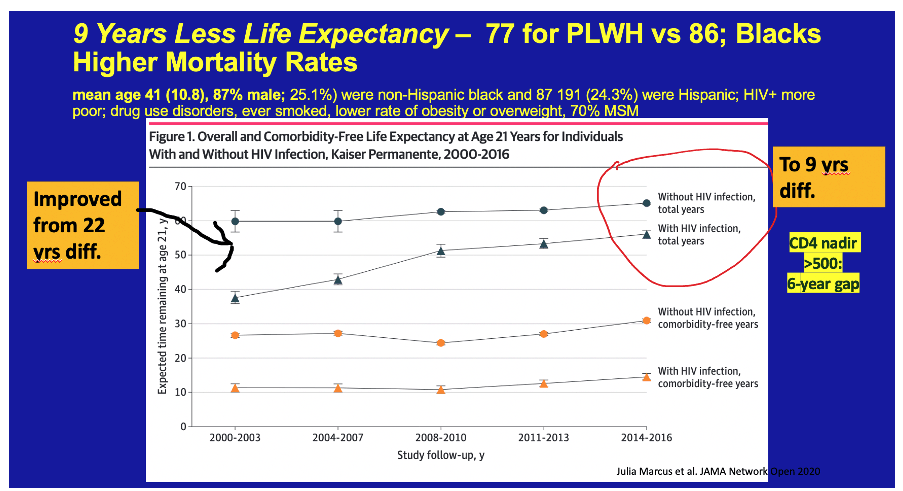
https://www.natap.org/2020/HIV/marcus_2020_oi_200340(1).pdf
In Trickey and colleagues' study, the difference in years of life left at age 40 years between women and men who started ART after 2015 was small (39⋅0 years [95% CI 38⋅5-39⋅5] vs 37⋅0 years [36⋅5-37⋅6]). However, in the general population, women's
life expectancy exceeds that of men in most countries by 4-8 years. For women who started ART after 2015, their estimated life expectancy was still 6⋅8 years lower than that of women in the general population. This difference in life expectancy was substantially greater for women who acquired HIV via injection drug use, whose life expectancy was 11⋅7 years shorter than that of women in the general population, even if they had more than 500 CD4 cells per μL at the start of follow-up, did not have AIDS, and had suppressed viral loads. These results speak to the changing epidemiology of mortality among people with HIV and the devastating consequences of opioid-overdose epidemics occurring worldwide, which will threaten the life-expectancy gains made with HIV and hepatitis C virus therapies if not addressed.
The North American AIDS Cohort Collaboration on Research and Design has similarly found that life expectancy has increased over time among people with HIV taking ART.
However, disparities in survival of approximately a decade persist between Black and white men who have sex with men, and between people with a history of injection drug use and those without a history of injection drug use. These disparities were only partly erased when simulating a 20% reduction in drug-related and alcohol-related mortality, suggesting that other causes of death also need to be addressed.
Life-expectancy gains have also been reported among people with HIV taking ART in low-income and middle-income countries.
In Africa, given the burden of HIV, these gains have helped to reverse overall population declines.
As in North America and Europe, however, not all groups have experienced the same gains in life expectancy (eg, gains in life expectancy have been less substantial among men, people with lower CD4 cell counts, people with tuberculosis, and people with lower levels of education).
|
|
| |
| |
|
|
|