| |
Several cases of Apparent Mpox Reinfection in Europe
|
| |
| |
Download the PDF here - A Case of Mpox Reinfection
Download the PDF here - Supplementary appendix
Download the PDF here - Case of apparent mpox reinfection
Download the PDF here - Second clinical episode of hMPX virus in a man having sex with men
Download the PDF here - Two individuals with potential monkeypox virus reinfectio
Download the PDF here - A tale of potential mpox reinfection
see below for these cases in several European cities
---------------
Risk Assessment of Mpox Resurgence and Vaccination Considerations
If mpox reintroduction occurs and no additional vaccination or sexual behavior adaptations occur, the risk of a resurgent mpox outbreak is greater than 35% in most jurisdictions in the United States. Resurgent outbreaks in these communities could be as large or larger than the 2022 outbreak. This is because immunity is relatively low in populations who are highly affected, including sexually active men who have sex with men (MSM) in these jurisdictions. In jurisdictions where immunity is higher in these populations, the risk is anticipated to be low over the next year, although a renewed outbreak could occur. These jurisdictions include most jurisdictions that had large mpox outbreaks in 2022, such as California, the District of Columbia (DC), Illinois, and New York.
https://www.cdc.gov/poxvirus/mpox/response/2022/risk-assessment-of-resurgence.html
--------------------------
US cases remain low
As a whole, weekly US mpox cases remain low, with the country averaging about one or two new cases per day over the past several weeks, according to data from the CDC.
Meanwhile, the Chicago Department of Public Health data show a rise in cases that began at the end of April, with the city averaging about six or seven cases over the past few weeks.
U.S. public health officials want high-risk individuals who haven't been vaccinated for mpox -- previously called monkeypox -- to do so before a potential resurgence of the virus in the coming months.
That surge could be worse than last year, federal modeling has found, but only about 23% of those at high risk for the virus have received vaccines, according to a report released Thursday by the U.S. Centers for Disease Control and Prevention.
Most communities have had too few people vaccinated to avoid a potential outbreak and have a "greater than 35%" risk of the virus resurging, the CDC said.
"It's not us saying get more people vaccinated because we think it's a good idea. We need to get more people vaccinated because we know there's a linear relationship between how many people are vaccinated and the chance of not having an outbreak," Dr. Demetre Daskalakis, deputy coordinator for the White House's mpox response, told CBS News.
People who survived previous mpox infections may have some protection already, according to the CDC. The risk of reinfection could grow for those individuals, however, over time and if the virus mutates, the report noted.
"This is the time to do that little health check, that tune-up before we get into summer to make sure that we have all our ducks in a row," Daskalakis said.
Now is a good time to get the Jynneos mpox vaccine while cases are down, he added.
"People with two doses should feel pretty confident that they're protected. But then always remember, if you have a lesion that's concerning, you should get tested because nothing is perfect," Daskalakis said.
Mpox cases are now reported at about one case a day throughout the United States. At their peak last August, there were 450 daily reported infections.
In its efforts to curb the virus, the CDC has created a new webpage that provides an mpox vaccine locator. To find a site near you, visit the MPOX vaccine locator.
"This is getting embedded into the fabric that we do to prevent sexually transmitted infections, like HIV. So it's moved back into a space that's more routine," Daskalakis said.
The study findings were published March 31 in the CDC's Morbidity and Mortality Weekly Report
----------------------
UK reports more mpox cases, urges vaccination
May 26, 2023
Some UK patients have travel histories, vaccination gaps
In a statement, the HSA said it received reports of 10 more cases over the past 4 weeks, putting the number for the year at 20.
Half of the new cases were in unvaccinated people, and two in the group had received only one vaccine dose. Four patients likely contracted their infections abroad, and the source for one person is still undetermined.
https://www.cidrap.umn.edu/mpox/uk-reports-more-mpox-cases-urges-vaccination
--------------------------------
WHO
This report presents a summary of possible cases of reinfection with mpox reported in peer-reviewed
literature since the start of the outbreak. Overall, these few reported cases of mpox recurrence or re-
infection underscore the importance of ongoing data collection and reporting globally, particularly as our
understanding of mpox continues to evolve.
This is the 23rd situation report for the multi-country outbreak of mpox, which provides details on the latest epidemiology, special focus on reinfection with mpox from published literature articles and summary of mpox cases among vaccinated persons. The report also contains an update from the WHO South- East Asia Region.
https://www.who.int/docs/default-source/coronaviruse/situation-reports/20230526_mpox_external-sitrep-23.pdf?sfvrsn=66cef768_5&download=true
-------------------------------
Several cases of Apparent Mpox Reinfection in Europe
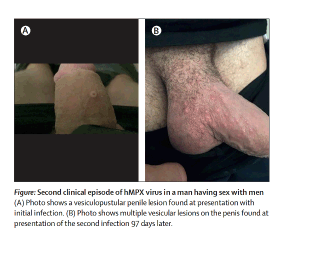
Second clinical episode of hMPX virus in a man having sex with men
Lancet March 24, 2023
Pdf attached
A 36-year-old man attended our hospital with an 8-day history of two vesiculopustular lesions on his penis (figure); he reported no fever or inguinal lymphadenopathy. The patient had no previous history of note; he had not been immunised against smallpox. Over the past 3 years he said that he regularly took pre-exposure prophylaxis (PrEP) against HIV.
4 weeks before the lesions appeared, the patient reported having condomless penetrative and receptive anal intercourse with approximately 30 male partners. None of his known partners had notified him of having developed similar symptoms.
On examination he was well; his temperature was 38·0°C. PCR of a sample of one of the penile lesions confirmed human monkeypox (hMPX) virus infection: MPX-virus PCR cycle threshold (Ct) 20·5. Tests for bacterial sexually transmitted infections-including gonorrhoea, chlamydia, and syphilis-were negative on oral, anal, and urine samples. The patient was isolated at home for 3 weeks and was prescribed symptomatic treatment for pain. During isolation, he experienced no other symptoms, but developed additional vesicular lesions on his trunk and upper and lower limbs. The course of the disease was uneventful, and all lesions disappeared completely within 30 days. In accordance with French recommendations, the patient was not vaccinated.
97 days after the first consultation, 50 vesicular lesions, associated with very painful inguinal lymphadenopathy, developed over 24 h on the patient's penis (figure); he reported no prodromal symptoms. 2 days later, he developed an influenza-like illness with a fever-temperature 38·5°C-fatigue, myalgias, and headache; the symptoms resolved spontaneously 9 days after onset. Laboratory investigations showed negative HIV serology and HIV-1 RNA PCR was less than 20 copies per mL, but immunoglobulin G against hepatitis A and hepatitis B, Epstein-Barr virus, and cytomegalovirus were positive. PCR on a sample from a penile swab was negative for herpes simplex virus types 1 and 2, and varicella zoster virus, although a concurrent pharyngeal gonorrhoea infection was found. Two hMPX virus PCRs on samples of cutaneous swabs obtained at the second-episode consultation (Ct 30·3) and 7 days later (Ct 33·21) confirmed the diagnosis. During the month preceding the second episode, the patient reported having unprotected sex with approximately 50 male partners from European countries, where he had attended mass gatherings and sex parties. Facing a potential hMPX reinfection, neutralising antibodies against the hMPX virus (appendix) were measured; the titers were weakly positive (index 20·3) and abnormally low for a person with a documented hMPX virus infection 3 months earlier. Samples from both the first and second episodes were whole-genome hMPX virus sequenced (appendix) and the isolates were found to belong to hMPX virus subtype IIb, lineage B.1, which has been previously described in the European outbreak. Comparisons between the sequences from the different episodes showed the viruses differed at 14 single nucleotides, one DNA sequence insertion, and one DNA sequence deletion (appendix). Phylogenetic analysis clustered the two sequences together (bootstrap value 95%).
In conclusion, we believe our patient was reinfected with a different hMPX. Vaccination may be considered on a case-by-case basis for people at very high risk of repeatedly contracting the disease.
---------------------------
Editorial
Published online 2023 Apr 6
Pdf attached
A tale of potential mpox reinfection
In this issue of The Lancet Infectious Diseases, we report two independent cases of potential mpox (formerly know as monkeypox) reinfection. Two men had PCR-confirmed mpox with typical signs and symptoms. Following resolution, both men had negative PCR tests. After a symptom free interval of 1 and 4 months and condomless sex, one developed proctitis and the other a typical lesion with genital involvement. On further investigation, they tested positive for monkeypox virus again. Unfortunately, it was impossible sequence virus from the second episodes to determine whether the virus was identical (indicating relapse) or different (indicating reinfection) from the first episode. Potentially, PCR could also have picked up lingering virus from the sexual exposure that had not caused infection, although several swabs were positive, making this less likely. Uncertainty remains whether these cases represent true reinfection, relapse or viral remnants.
For the other case of potential reinfection see Sex Transm Infect 2023; published online Jan 27. https://sti.bmj.com/content/early/2023/01/26/sextrans-2022-055736
------------------
Case report
Case of apparent mpox reinfection
STI Jan 2023
Pdf attached
Abstract
We present an apparent second episode of mpox (monkeypox) genital ulcerative disease in a non-immunosuppressed MSM (man who has sex with men) patient who had completely recovered from a primary mpox infection 4 months previously. The patient had also received a complete two-dose course of smallpox vaccination between the two presentations. This case highlights the importance of continuing to include mpox in the differential diagnoses for individuals presenting with genital or mucosal ulceration, regardless of assumed immunity derived from prior infection or vaccination.
Discussion
As far as we are aware, there have not been any other published cases of reinfection during the 2022 mpox outbreak. An alternative explanation to reinfection is that mpox infection persisted following first infection during the intervening period. This is unlikely to explain the new clinical signs and prodromal illness the patient experienced at the second presentation, which could not be attributed to any other investigated STI. Persistence is also unlikely, given that time from infection to viral clearance is typically less than 6 weeks6 and the repeat rectal swab 2 weeks after the second presentation was negative for mpox. Nucleotide sequence comparison of mpox DNA detected in both clinical episodes and additional tests between episodes would be required to shed further light on this. Meanwhile, this case informs the advice health professionals give to patients about mpox and clearly indicates including mpox infection in the differential for patients presenting with mucocutaneous lesions, regardless of prior infection or vaccination status.
------------------
Two individuals with potential monkeypox virus reinfection, Italy
2023 May
Over 80 000 mpox (formerly known as monkeypox) cases have been confirmed worldwide and recovered individuals are considered protected against reinfection.1, 2, 3 However, an individual with apparent reinfection has been recently reported.4 In this Comment we describe two individuals with potential monkeypox virus reinfection at San Raffaele Hospital, Milan, Italy (figure ; see appendix for details on testing and results).
The first individual is a 36-year-old man who has sex with men (MSM) who presented with asthenia, pharyngodynia, and fever with tenesmus and mucorrhoea on May 24, 2022, with symptom onset a week earlier, after attending a large gathering in Spain in early May, during which he had condomless oral intercourse and condomless anal intercourse with several partners. He is on antiretroviral therapy for a known HIV infection (1099 CD4+ cells per μL; HIV-RNA <20 copies per mL since 2015) and had no other medications or comorbidities.
He presented with a perianal ulceration, a pharyngeal lesion, and lymphadenopathy. Monkeypox virus PCR was positive for lesion, rectal, and oropharyngeal swabs with cycle threshold values ranging between 18 and 32, with concurrent chlamydia proctitis. Symptoms and lesions resolved by June 1, 2022, and a monkeypox PCR was negative for plasma, oropharyngeal, and anal swabs.
On Aug 23, 2022, he presented with oral and cutaneous non-ulcerated erythematous lesions. Mpox was excluded with oropharyngeal, anal, and lesion swabs, and chlamydia urethritis was detected, which resolved after doxycycline treatment (100 mg twice per day for 7 days).
On Sept 27, 2022, he presented with a single, umbilicated vesicular lesion on the glans penis following condomless oral intercourse and condomless anal intercourse with several individuals who were later diagnosed with mpox. Lesion swabs and oropharyngeal swabs were positive for monkeypox virus with cycle threshold values of 37 and 34, with concurrent chlamydia proctitis. The lesion resolved by Oct 1, 2022, and all subsequent swabs from several locations were negative for the monkeypox virus. He had not received mpox vaccinations and had antibody titre of 1/40 after the first episode. This titre remained stable after the second episode.
The second individual is a 33-year-old MSM who uses pre-exposure prophylaxis for HIV with no comorbidities or comedications. He presented with proctitis, a single vesicular lesion on the lower lip, and lymphadenopathy on July 7, 2022, after condomless oral intercourse and condomless anal intercourse with several partners during the previous month. Anoscopy revealed mucosal congestion with erosions and ulcerations, and a rectal swab was positive for both monkeypox virus with a cycle threshold value of 37, and for chlamydia. All other swabs were negative. On July 14, 2022, the proctitis and lesion resolved but he developed pharyngodynia with a positive oropharyngeal swab for monkeypox virus with a cycle threshold value of 25, and a negative rectal swab. On July 20, an oropharyngeal swab, a lesion swab from the right shoulder, and plasma sample were positive for monkeypox virus with cycle threshold values between 22 and 37. Symptoms and lesions resolved by July 26, and swabs from multiple body sites were negative on Aug 2, 2022.
On Aug 22, 2022, he presented with proctitis after a large gathering in Spain (Aug 5–13, 2022), where he had condomless oral intercourse and condomless anal intercourse with several partners. Rectal and oropharyngeal swabs were positive for monkeypox virus at cycle threshold values of 29 and 32, with concurrent gonorrhoea proctitis and SARS-CoV-2 infection of the upper respiratory tract.
Proctitis resolved and only the oropharyngeal swab remained positive on Aug 26. Swabs taken between Aug 31 and Sept 7, 2022 from different body sites were all negative. He was not vaccinated for mpox; after resolution of the first episode he had monkeypox antibody titres of 1/20, which increased to 1/160 after the second episode.
These cases represent two potential monkeypox virus reinfections. Following clinical and virological healing of the first episodes, we observed high cycle threshold values and short-lasting symptoms for both second episodes, with clinical characteristics consistent with mpox, and detectable neutralising antibodies. The cycle threshold values were high for new-onset mpox and suggest low viral loads. Possible alternative explanations to reinfection include relapse from tissue reservoirs or sexual contamination.5, 6 Indeed, potential relapse of infection and persistent monkeypox virus detection have been described previously.7, 8 The second patient, in particular, had episodes relatively close together, which could indicate recrudescence. However, high cycle threshold values and fast healing could also be linked to presence of neutralising antibodies. Furthermore, samples from different sites and different time-points (in the second patient) were positive for monkeypox virus, which makes environmental contamination less likely. Both patients had co-infections, which could have caused or exacerbated symptoms, or could have eased reinfection. We isolated and sequenced monkeypox virus from both patients from samples collected during the first episodes. We could not isolate the virus from samples from the second episodes, probably due to low viral loads as indicated by the high cycle threshold values. SARS-CoV-2 could also have had a negative influence.9, 10 Although genomic data cannot confirm the presence of two distinct viruses, and thus reinfection (in contrast to relapse, which would have presented with the same virus), clinicians need to be aware of potential monkeypox virus reinfections and should investigate with viral culture and sequencing. Furthermore, the potential of monkeypox reinfection has implications for transmission and vaccination policies.
----------------------
A Case of Mpox Reinfection, Swiss case
CID Jan 2023
Pdf attached
Abstract
A healthy young man first diagnosed with mpox in May 2022 presented again in November 2022 with anal proctitis and a positive polymerase chain reaction on a rectal swab for Monkeypox virus after a recent trip to Brazil, where he engaged in condomless sexual intercourse with multiple male partners.
Mpox, caused by Monkeypox virus (MPXV), was considered a sporadic zoonotic disease limited to West and Central African countries until the current worldwide outbreak was declared in May 2022. MPXV belongs to the Orthopoxvirus genus, as do Vaccinia virus, Cowpox virus, and Variola virus, all of which are infectious to humans. MPXV infection generates humoral and cellular immunity that is expected to provide long-term protection against reinfection [1]. These assumptions are based on extensive experience with Variola virus, the agent of smallpox disease [2]. Smallpox infection or vaccination with the attenuated Vaccinia virus provided almost complete protection from infection with Variola virus thanks to cross-immunity [2]. Even years after the last smallpox vaccination, individuals historically vaccinated are considered less likely to be infected by MPXV than nonvaccinated persons and protected from severe disease [3]. MPXV reinfection has only been reported by Golden et al [4], so far suggesting it is at most an infrequent event.
Since 1980, waning immunity against smallpox of historically vaccinated or naturally infected persons and the heightened number of susceptible individuals have been considered the main drivers for the mpox flares in African endemic regions. In the Democratic Republic of Congo, between 1980 and 2007, reported infections with MPXV increased 20-fold. While these studies suggest protective, long-lasting cross-immunity through smallpox vaccination, data on elicited protection after MPXV infection are scarce. Here we report a case of Monkeypox virus reinfection in an otherwise healthy adult.
|
|
| |
| |
|
|
|