 |
 |
 |
| |
Each Higher Sedative Burden Unit Boosts Odds of Physical Frailty With HIV 35%
|
| |
| |
IAS 2023, July 23-26, 2023. Brisbane
Mark Mascolini
Each higher unit on an established sedative burden scale boosted odds of physical frailty by 35% in a study of 824 adults with HIV [1]. Use of any sedative on this scale made odds of frailty 84% higher.
People with HIV infection may be prescribed many drugs with sedative properties, including medications for anxiety, pain, insomnia, muscle spasms, and seizures, noted McGill University researchers who conducted this study. And research links these drugs to frailty in a general population of older men [2]. Because frailty tends to develop at an earlier age in people with HIV, the McGill team in Montreal completed a cross-sectional study to weigh the impact of sedative burden on concurrent frailty in people with HIV.
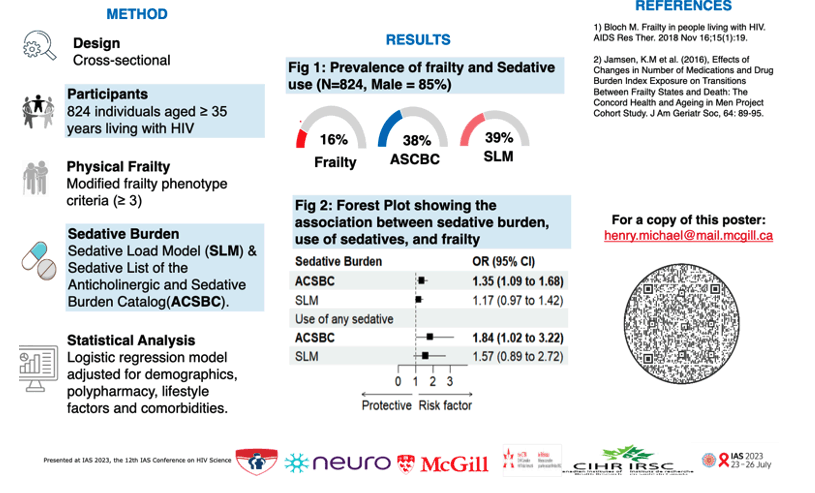
The study population included 824 people with HIV in Canada, all of them at least 35 years old and 85% of them men. The researchers defined physical frailty as 3 or more of the 5 components of the standard frailty phenotype [3]. They determined sedative burden by two methods, the Sedative Load Model (SLM) and the sedative list of the Anticholinergic and Sedative Burden Catalog (ACSBC) [4]. They defined sedative burden as a cumulative score of all the sedative burdens of individual medications (a score of 0 to 3 representing no sedative activity, low activity, moderate activity, and high activity (see "The Comprehensive Review Table" in reference 4). To identify predictors of frailty, they used a logistic regression model adjusted for demographics, polypharmacy (multiple drugs besides antiretrovirals), lifestyle factors, and comorbidities.
Among these 824 people, 16% had frailty. Logistic regression determined that each one-unit higher sedative burden score on the ACSBC predicted 35% higher odds of frailty (adjusted odds ratio [aOR] 1.35, 95% confidence interval [CI] 1.09 to 1.68). Each unit higher sedative burden on the SLM boosted odds of frailty 17%, but that association stopped short of statistical significance (aOR 1.17, 95% CI 0.97 to 1.42). Use of any ACSBC medication independently raised odds of frailty 84% (aOR 1.84, 95 CI 1.02 to 3.22). But the analysis did not link use of any sedative on the SLM to higher odds of frailty (aOR 1.57, 95% CI 0.89 to 2.72).
The McGill team believes their findings contribute evidence to support a composite sedative burden scale like the ACSBC. They encouraged HIV clinicians to minimize use of drugs with sedative effects. But only longitudinal studies, they added, can determine if trimming sedative drug burden in people with HIV prevents or reverses frailty.
References
1. Michael HU, Brouillette M-J, Tamblyn R, Fellows LK, Mayo N. Sedative drug burden is associated with concurrent physical frailty in people aging with HIV in Canada: findings from the Positive Brain Health Now Study (+BHN). IAS 2023, July 23-26, 2023. Brisbane. Abstract MOPEB20.
2. Jamsen KM, Bell JS, Hilmer SN, et al. Effects of changes in number of medications and drug burden index exposure on transitions between frailty states and death: the Concord Health and Ageing in Men Project Cohort Study. J Am Geriatr Soc. 2016;64:89-95. doi: 10.1111/jgs.13877. https://agsjournals.onlinelibrary.wiley.com/doi/10.1111/jgs.13877
3. Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146-56. doi: 10.1093/gerona/56.3.m146. https://pubmed.ncbi.nlm.nih.gov/11253156/
4. Al Rihani SB, Deodhar M, Darakjian LI, et al. Quantifying anticholinergic burden and sedative oad in older adults with polypharmacy: a systematic review of risk scales and models. Drugs Aging. 2021;38:977-994.doi: 10.1007/s40266-021-00895-x. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8592980/


|
| |
|
 |
 |
|
|