 |
 |
 |
| |
Black Race, Perceived Stress Affect CVD Risk Conditions in PLHIV
|
| |
| |
IDWeek 2023, October 11-15, 2023, Boston
Mark Mascolini
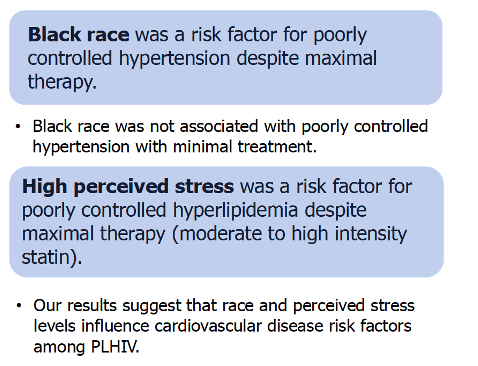
Black race tripled the odds of poor hypertension control despite maximal antihypertensive therapy in a 371-person study in three US academic HIV clinics [1]. High perceived stress boosted risk of poor hyperlipidemia control 3.5-fold in people with maximal treatment of hyperlipidemia. And the study group had high health literacy.
Higher risk of cardiovascular disease (CVD) in people living with HIV (PLHIV) is well documented, noted Duke University researchers who conducted this study. And two key CVD risk factors-hypertension and hyperlipidemia-often get suboptimal management in the HIV population.
The Duke team aimed to analyze both control of hypertension and hyperlipidemia in PLHIV and treatment intensity for these conditions, so there could be four outcomes: poor control with minimal treatment, poor control with maximal treatment, good control with minimal treatment, and good control with maximal treatment. The investigators hypothesized that people "with adverse social determinants of health profiles would be more likely to fall in the poor control/minimal treatment group." They focused on an array of social determinants of health: race, sex, measures of economic stability, education level, health insurance, health literacy, social deprivation index by zip code, and psychosocial stress measures.
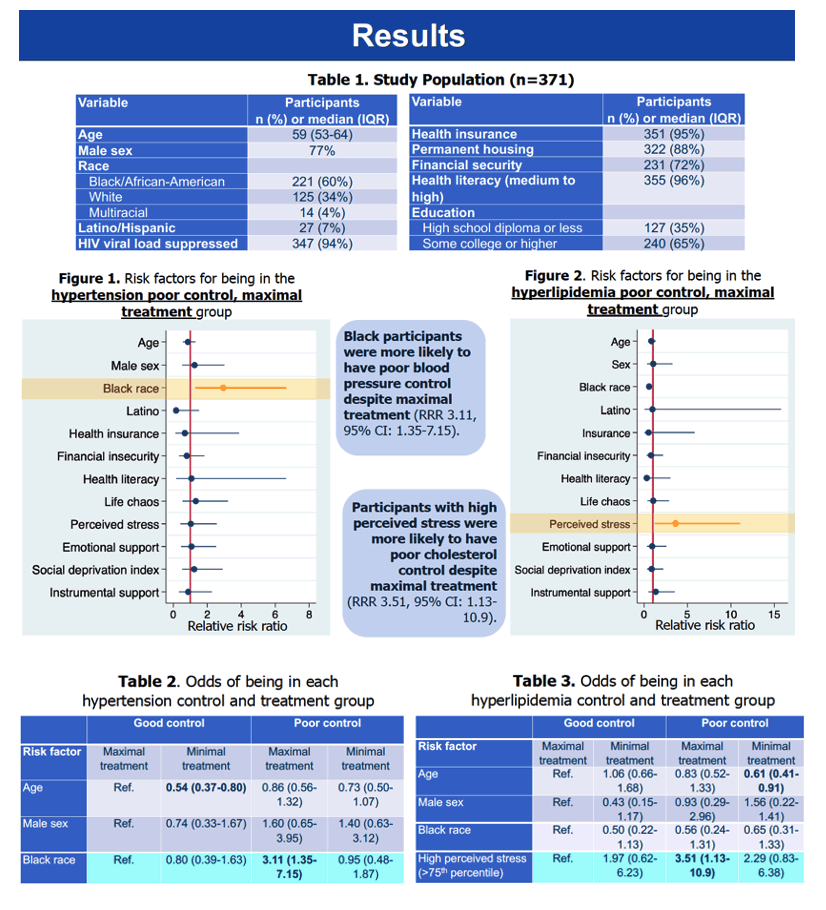
The 371 study participants came from one clinic in Durham, North Carolina and two clinics in Cleveland, Ohio. Median age stood at 59 years, 77% of participants were men, 60% black, 34% white, 4% multiracial, and 7% Hispanic. A large majority, 94%, had an undetectable viral load. High percentages of the study group had health insurance (95%), medium to high health literacy (96%), and permanent housing (88%). Lower fractions, but still majorities, had financial security (72%) and at least some college education (65%).
Multinomial logistic regression that adjusted for age, sex, and race determined that black race more than tripled the relative risk of poor hypertension control despite maximal treatment (relative risk ratio [RRR] 3.11, 95% confidence interval [CI] 1.35 to 7.15. But being black did not affect risk of poorly controlled hypertension in people getting minimal treatment for hypertension. The researchers defined maximal and minimal treatment of hypertension according to a treatment intensity score proposed by Phillip Levy and colleagues [2]; maximal treatment means a score above 1 and minimal treatment means a score of 1 or lower.
People with high perceived stress (above the 75th percentile) had a 3.5-fold higher relative risk of poor cholesterol control despite maximal treatment of hyperlipidemia (RRR 3.51, 95% CI 1.13 to 10.9). Maximal treatment of hyperlipidemia meant using a moderate- to high-intensity statin.
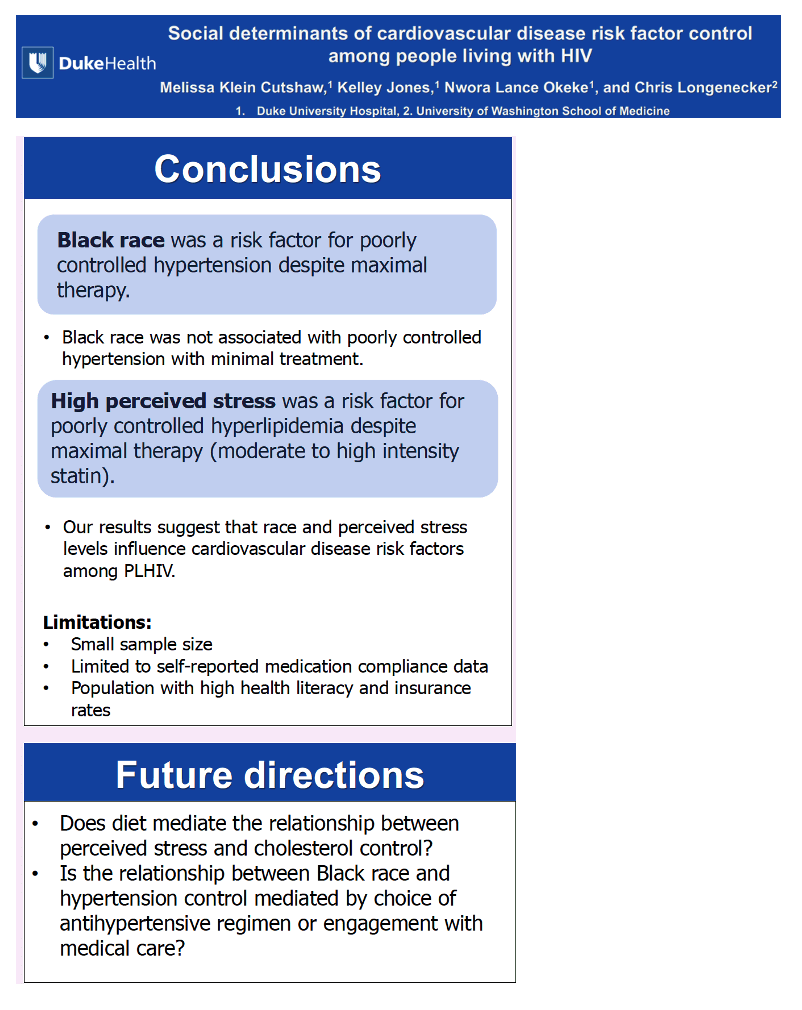
The researchers suggested their findings support the ideas that black race or high perceived stress influence major risk factors for cardiovascular disease in people with HIV-hypertension and hyperlipidemia-even when people receive maximal treatment for hypertension and hyperlipidemia. They proposed that these two finding raise other questions, such as:
"Does diet mediate the relationship between perceived stress and cholesterol control?"
"Is the relationship between Black race and hypertension control mediated by choice of antihypertensive regimen or engagement with medical care?"
The investigators cautioned, though, that their study sample was small and may not represent other HIV populations because of their high health literacy and insurance rates. Also, the study relied on self-reports to gauge treatment adherence.
References
1. Cutshaw MK, Jones K, Okeke NL, Longenecker C. Social determinants of cardiovascular disease risk factor control among people living with HIV. IDWeek 2023, October 11-15, 2023, Boston.
2. Levy PD, Willock RJ, Burla M, et al. Total antihypertensive therapeutic intensity score and its relationship to blood pressure reduction. J Am Soc Hypertens. 2016;10:906-916. doi: 10.1016/j.jash.2016.10.005.
https://www.sciencedirect.com/science/article/abs/pii/S1933171116305496?via%3Dihub


|
| |
|
 |
 |
|
|