 |
 |
 |
| |
Feasibility of Implementing a Low-Barrier Long-Acting Injectable Antiretroviral Program for HIV Treatment & Prevention for People Experiencing Homelessness
|
| |
| |
Download the PDF here
Mehtani, Nicky J. MD MPH1,2,3,a; Strough, Alix RN2; Strieff, Sarah RN2; Zevin, Barry MD2; Eveland, Joanna MD2; Riley, Elise D. PhD MPH3; Gandhi, Monica MD MPH3
While this pilot program represents a small cohort over only a 24-month period, the rate of sustained virologic suppression observed among PWH initiated on LA-ART was high (94%), despite the majority having baseline viremia, and all LA-PrEP patients remained HIV free over the study period. Moreover, the substantial representation of populations underserved in traditional primary care settings-including dual-diagnosed, transgender, Black, and Hispanic patients, in addition to eight PWH who had never previously been virally suppressed as outpatients-supports findings from qualitative studies suggesting the unique potential of LA antiretrovirals in addressing barriers to HIV- and PrEP-related care [19,20]
Abstract
Background:
Long-acting (LA) antiretrovirals may provide meaningful benefit to people who use drugs and people experiencing homelessness (PEH) who face disproportionate structural and psychosocial barriers in adhering to daily oral HIV antiretroviral therapy (ART) or pre-exposure prophylaxis (PrEP), but their use in these populations has not been studied.
Setting:
The Maria X. Martinez Health Resource Center is a low-barrier (e.g., no appointment) community-based clinic serving San Francisco PEH.
Methods:
A multidisciplinary care model with robust monitoring and outreach support was developed to provide LA-ART and LA-PrEP to eligible patients experiencing difficulties adhering to oral antiretrovirals. Feasibility was assessed by evaluating rates of HIV viremia and on-time injections among patients receiving LA antiretrovirals over the first 24 months of program implementation.
Results:
Between November 2021 and November 2023, 33 patients initiated LA-ART or LA-PrEP (median age, 37 years; 27% transgender/non-binary; 73% non-White; 27% street homeless; 52% sheltered homeless; 30% with opioid use disorder; 82% with methamphetamine use disorder).
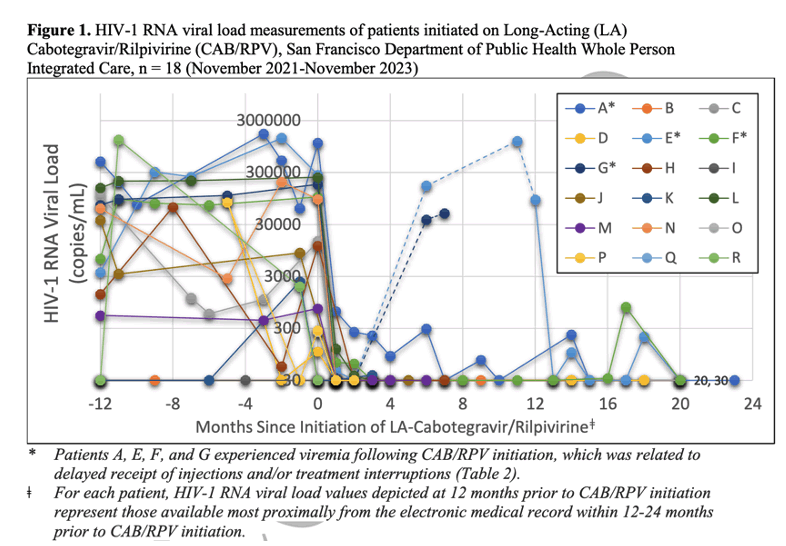
Among 18 patients with HIV, 14 initiated LA-ART injections with detectable viremia (median CD4 count, 340 cells/mm3; mean log10 viral load, 3.53; standard deviation [SD], 1.62), eight had never previously been virally suppressed, and all but one achieved or maintained virologic suppression (mean, 9.67 months; SD, 8.30).
Among 15 LA-PrEP patients, all remained HIV-negative (mean, 4.73 months; SD, 2.89). Of 224 injections administered total, 8% were delayed >7 days.
Discussion:
The implementation of LA antiretrovirals is feasible in low-barrier, highly supportive clinical settings serving vulnerable PEH. Expansion of such programs will be critical to Ending the HIV Epidemic.
|
| |
|
 |
 |
|
|