 |
 |
 |
| |
Multinational randomized trial to investigate the efficacy of tenofovir alafenamide in reducing adverse clinical events in chronic hepatitis B patients who are beyond treatment indications by current guidelines (ATTENTION trial): first interim analysis
TAF Slices Serious Liver Outcomes 80% in People Without High ALT
|
| |
| |
EASL Congress 2024, June 5-8, 2004, Milan
Mark Mascolini
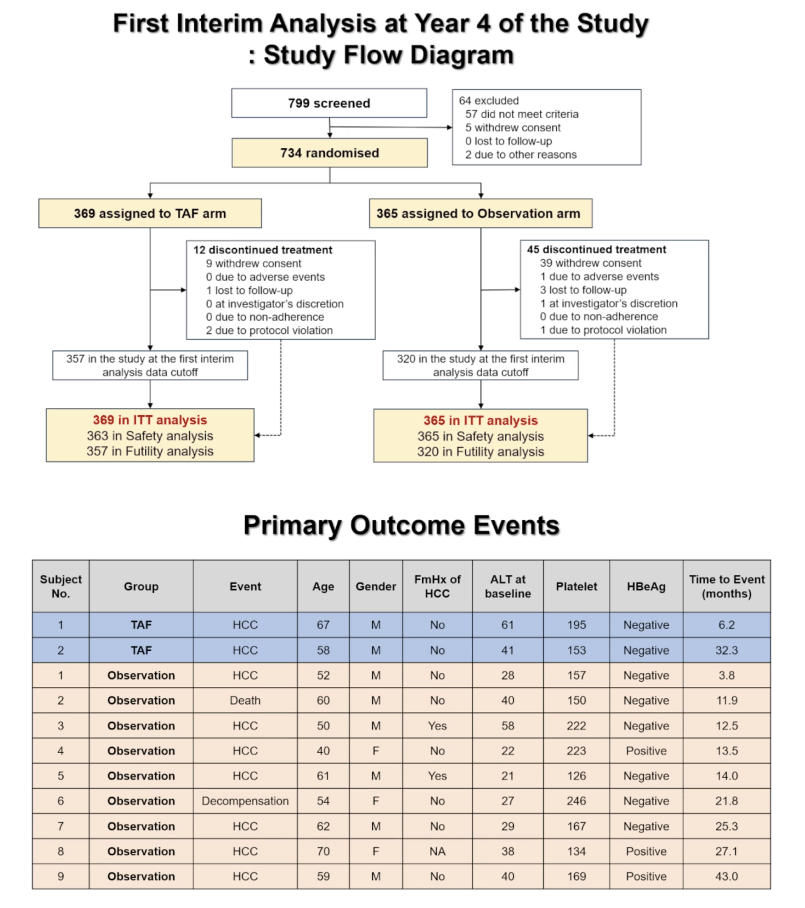
Serious adverse liver outcomes proved significantly less frequent with tenofovir alafenamide (TAF) than with no treatment in adults with HBV and moderate viremia who do not meet current treatment criteria because their alanine aminotransferase (ALT) has not climbed into the red zone [1]. That finding emerged from an interim analysis of an ongoing randomized trial that had enrolled 734 adults in Korea and Taiwan at the time of this analysis.
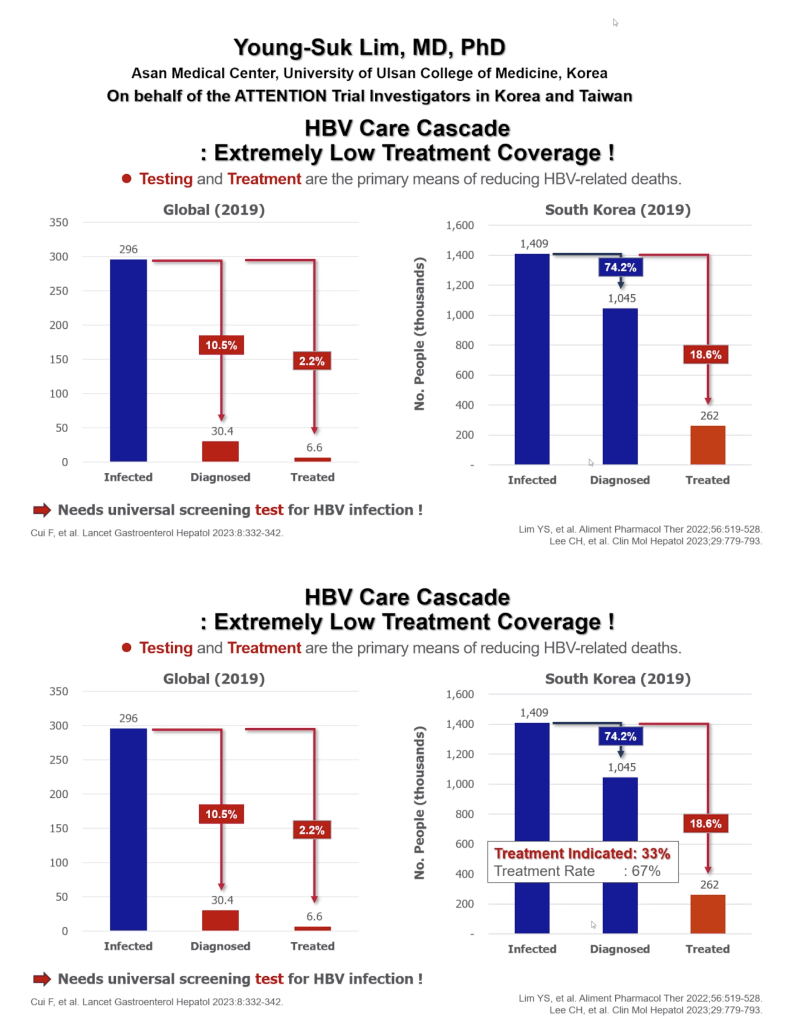
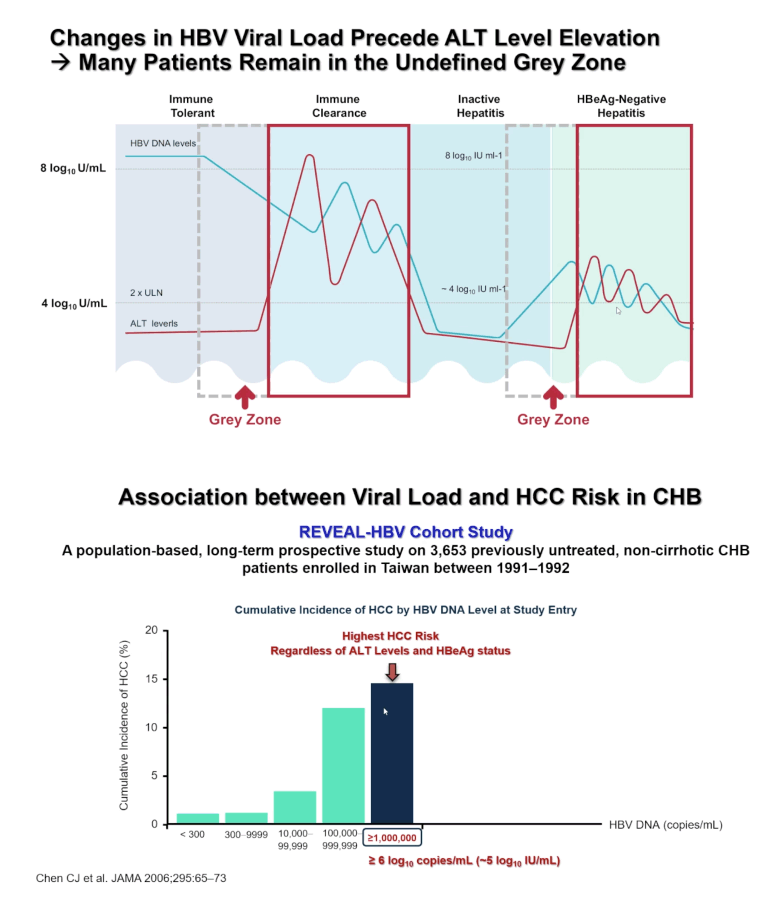
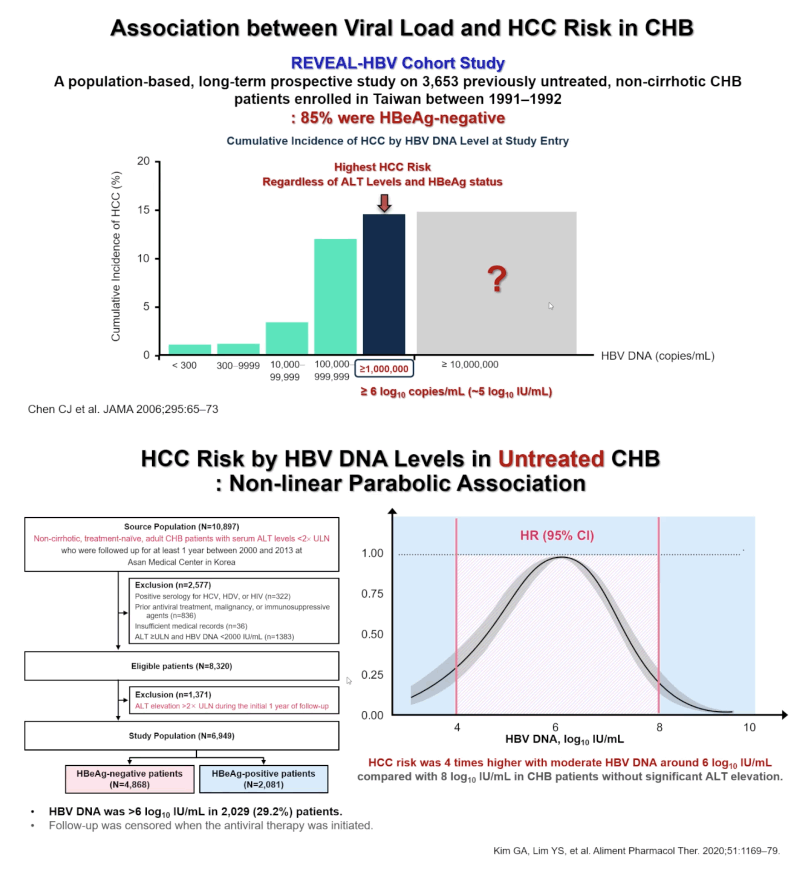
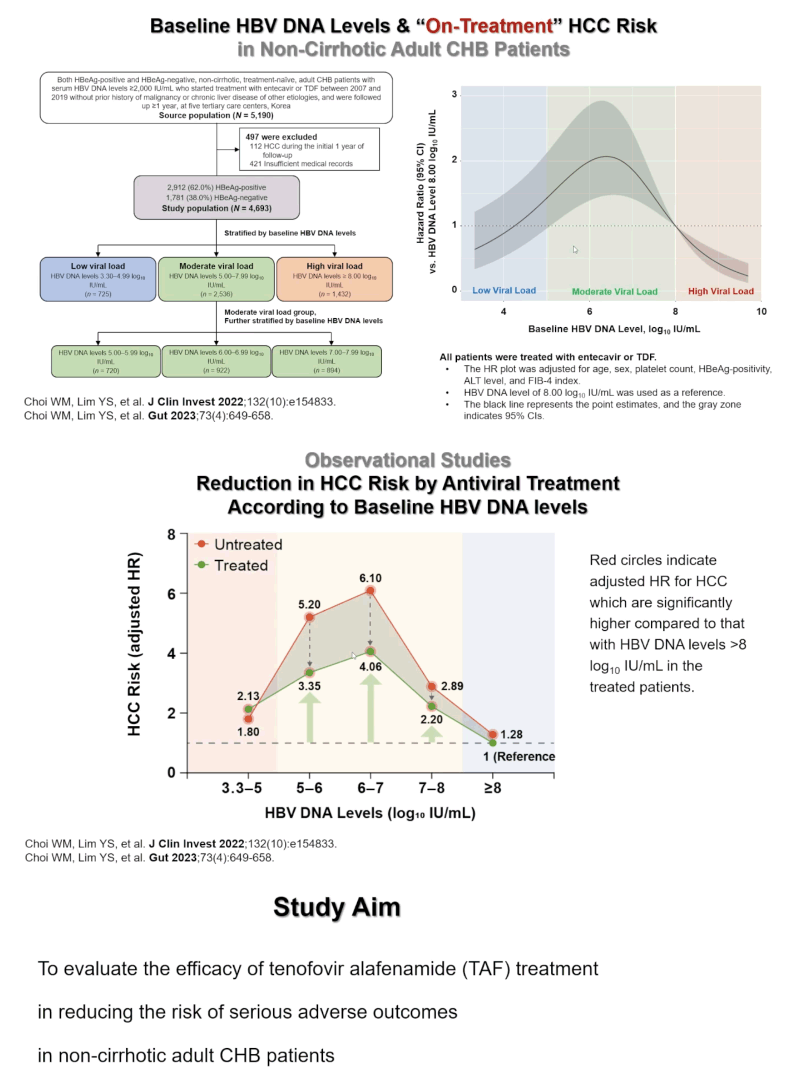
Young-Suk Lim (University of Ulsan, Korea) and colleagues throughout Korea and Taiwan reminded EASL attendees that treatment of HBV remains "extremely low:" 18.6% of HBV-infected people in South Korea & Taiwan (countries with high diagnosis rate), for example, and 2.2% of infected people globally. The reason is the current Guidelines in recommending treatment, only 33% are eligible, but treatment acceptance rate was high, 67%. Observational studies by investigators conducting the TAF randomized trial found that untreated people with higher pretreatment HBV loads ran a significantly greater risk of a notable serious liver outcome, hepatocellular carcinoma (HCC) [2,3].
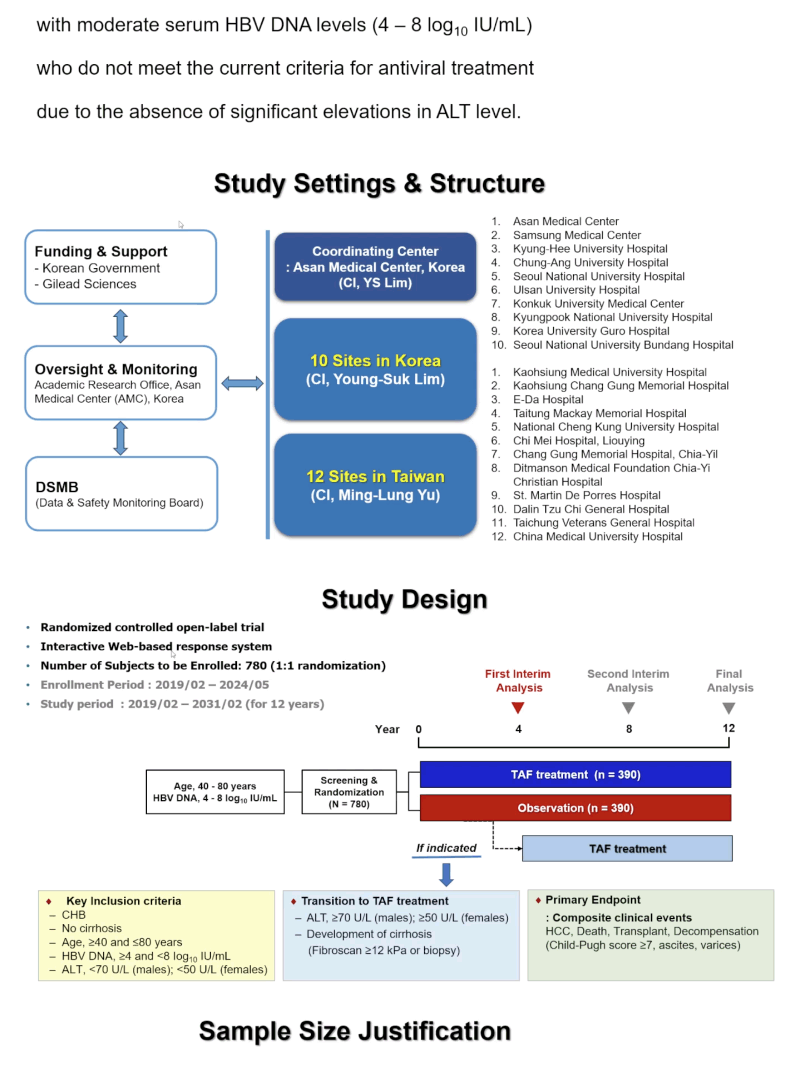
To determine whether TAF would have a clinical impact in people not eligible for the drug because of moderate ALT levels, the Taiwan-Korea team planed a randomized controlled open-label trial in 40- to 80-year-olds with chronic HBV infection, without cirrhosis, with a moderate HBV DNA level (4 to 8 log10 IU/mL) who do not meet local antiviral treatment criteria because they lack "significant elevations" in ALT. From February 2019 to May 2024 they enrolled 780 people and randomized them evenly to TAF or to observation with transition to TAF if ALT rose to or above 70 U/L in men and 50 U/L in women or if biopsy or a Fibroscan of 12 kPa or more indicated fibrosis. The composite primary endpoint includes HCC, death, transplant, and hepatic decompensation (Child-Pugh score 7 or higher, ascites, varices).
Statisticians determined that if the absolute value of test statistics comparing outcomes in the two study arms exceeds 4.17084 at the first interim analysis or 2.8458 at the second interim analysis, the null hypothesis (that treating with TAF has no more clinical value than not treating) is rejected and efficacy of treating this population with TAF is declared. If the absolute value of test statistics is less than 4.17084 at the first interim analysis or 2.8458 at the second interim analysis, the trial continues.
The researchers randomized 369 people to take TAF and 365 to stay off treatment unless the noted signals of clinical progression arose. When the trial began, the TAF group did not differ significantly from the observation group in age (median 52 and 54), proportion of men (45.8% and 47.1%), family history of HCC (22.0% and 24.1%), ALT (31 and 31 U/L), HBV DNA (4.8 and 5.0 log10 IU/mL) and follow-up months (17.7 and 17.7).
During follow-up, 2 primary outcomes emerged in the TAF group (both HCC) and 9 in the observation group (7 cases of HCC, 1 hepatic decompensation, 1 death). Baseline ALT tended to be higher in the 2 TAF takers (41 and 61 U/L) than in the 9 members of the observation group (21, 22, 27, 28, 29, 38, 40, 40, and 58 U/L). Time to event did not appear to differ between these two small groups, and everyone in both groups was negative for HBeAg.
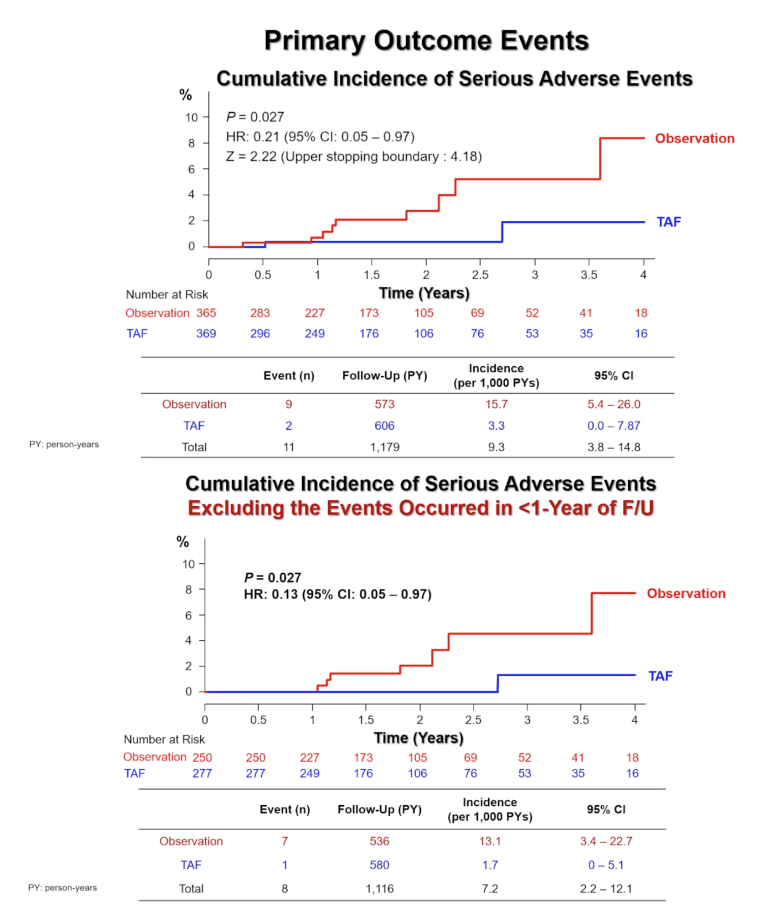
Cumulative incidence of primary outcome events was significantly greater in the observation group than in the TAF group (15.7 vs 3.3 per 1000 person-years [p-y], P = 0.027). These results meant people starting TAF immediately had an 80% lower risk of a primary outcome (hazard ratio [HR] 0.21, 95% confidence interval [CI] 0.05 to 0.97). But the Z statistic was 2.22, well below the 4.17 upper boundary that would stop the trial because immediate TAF outperformed observation in preventing primary events. So the trial continues.
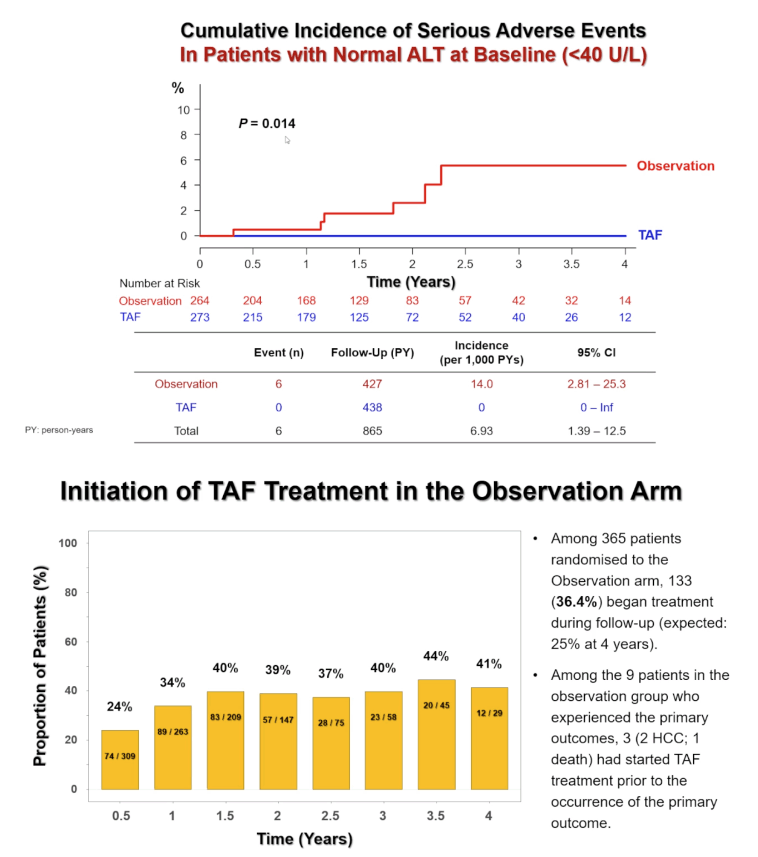
Cumulative incidence of serious events when excluding events that happened in the first year of follow-up stood at 13.1 per 1000 p-y in the observation group versus 1.7 per 1000 p-y in the TAF group (HR 0.13, 95% CI 0.05 to 0.97, P = 0.027). And cumulative incidence of these events in people with a normal baseline ALT (below 40 U/L) measured 14.0 in the observation group and 0 in TAF takers (P = 0.014).
The researchers projected that 25% of people in the observation arm would have to start TAF during the trial's first 4 years (for the reasons explained in the third paragraph above). But in fact 133 people (36.4%) had to begin TAF during the first 4 years of follow-up. Three of 9 people in the observation group who reached a primary event (2 with HCC and 1 who died) had started TAF before the event arose.
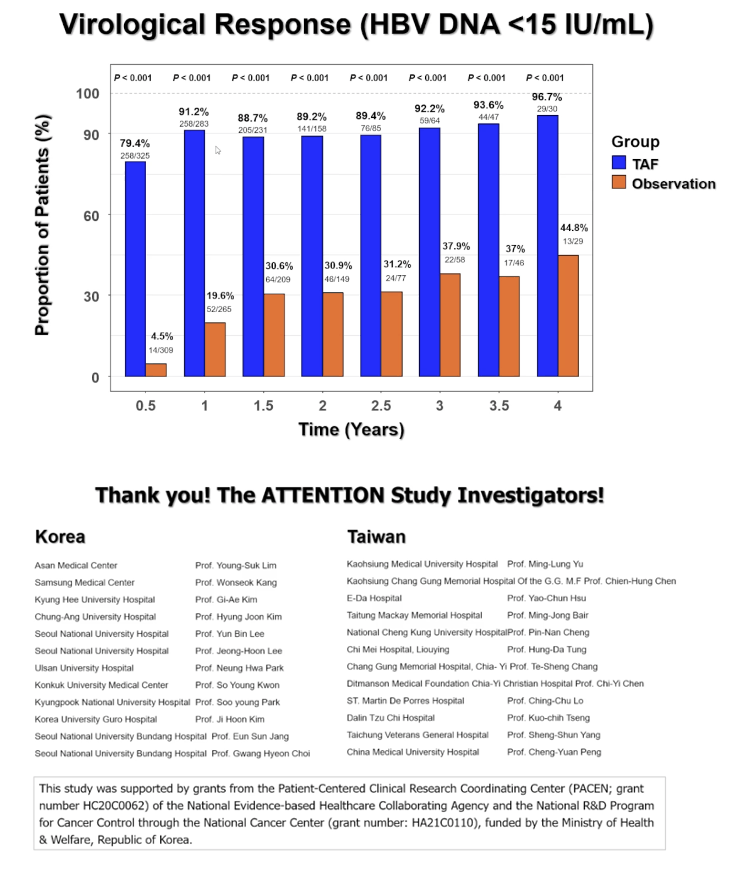
At each 6 months of follow-up, the proportion of people taking TAF who had a virologic response (HBV DNA below 15 IU/mL) significantly exceeded that proportion in the observation group. These proportions of virologic responders in the TAF arm rose from 79.4% at the first 6-month checkup to 96.7% at the 4-year point. In the observation group the proportion of responders climbed from 4.5% at the first 6-month study visit to 44.8% at the 4-year visit (P < 0.001 for all comparisons between the TAF arm and the observation arm).
The investigators believe these interim findings "highlight the potential benefit of proactive therapy" in people like those in this trial.
References
1. Lim YS, Choi J, Choi WM, et al. Multinational randomized trial to investigate the efficacy of tenofovir alafenamide in reducing adverse clinical events in chronic hepatitis B patients who are beyond treatment indications by current guidelines (ATTENTION trial): first interim analysis. EASL Congress 2024, June 5-8, 2004, Milan. Abstract OS-12.
2. Choi WM, Kim GA, Choi J, Seungbong H, Lim YS. Increasing on-treatment hepatocellular carcinoma risk with decreasing baseline viral load in HBeAg-positive chronic hepatitis B. J Clin Invest. 2022;132:e154833. oi: 10.1172/JCI154833. .
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9106348/
3. Choi WM, Kim GA, Choi J, et al. Non-linear association of baseline viral load with on-treatment hepatocellular carcinoma risk in chronic hepatitis B. Gut. 2024;73:649-658. doi: 10.1136/gutjnl-2023-330225. https://gut.bmj.com/content/73/4/649.long


|
| |
|
 |
 |
|
|