 |
 |
 |
| |
Bulevirtide Monotherapy Lowers Risk of Decompensation But Not HCC
|
| |
| |
EASL Congress 2024, June 5-8, 2004, Milan
Mark Mascolini
Bulevirtide monotherapy for 24 months cut risk of liver-related events and liver decompensation-but not hepatocellular carcinoma (HCC)-when compared with untreated controls from earlier decades [1]. Overall and liver-related survival proved similar in the two groups.
Clinical trials and cohort studies show that bulevirtide lowers HDV RNA load and produces favorable biochemical responses, but how bulevirtide affects clinical outcomes remained largely unknown until this case-control study. Researchers throughout Italy planned this analysis to gauge the impact of bulevirtide monotherapy on liver-related events and mortality in people with HDV-related compensated cirrhosis compared with a historical cohort of untreated controls with HDV cirrhosis.
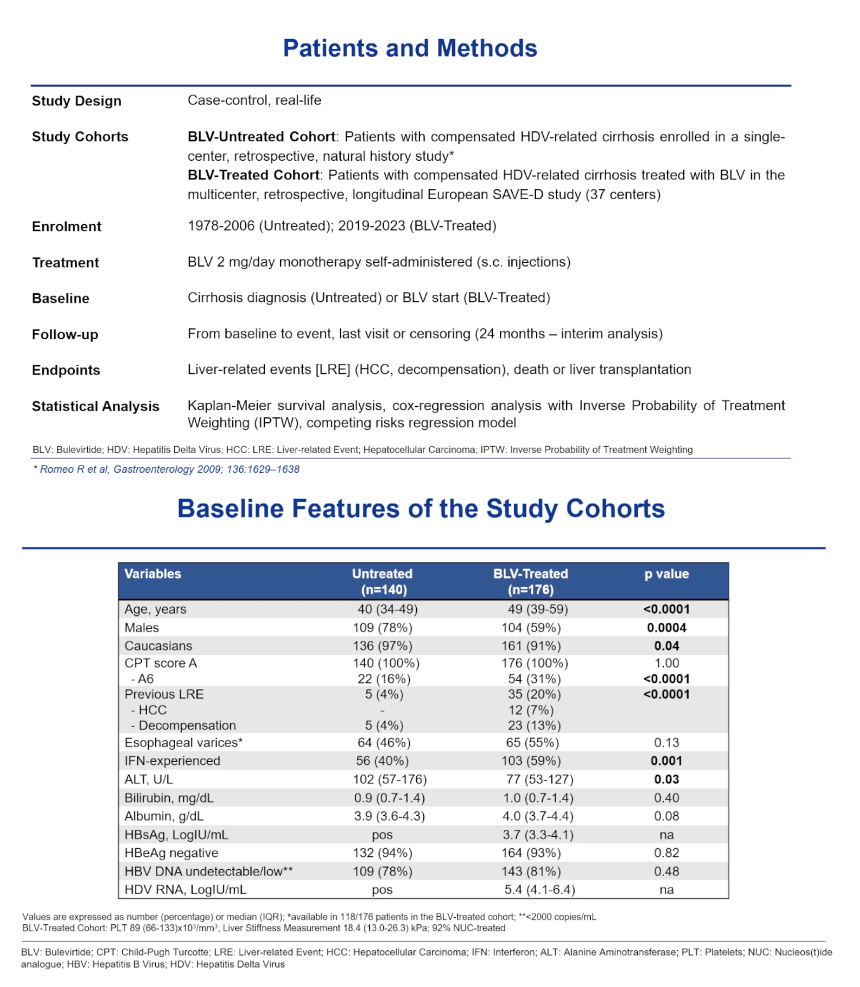
Treated participants took 2 mg of bulevirtide daily by self-administered subcutaneous injection in the 37-center retrospective longitudinal European SAVE-D study (2019-2023). Untreated controls came from a single-center retrospective natural history study of HDV (1978-2006) [2]. Baseline date was the day bulevirtide started or (in controls) the day of cirrhosis diagnosis. Follow-up ran from baseline to a clinical event or the last visit or for 24 weeks.
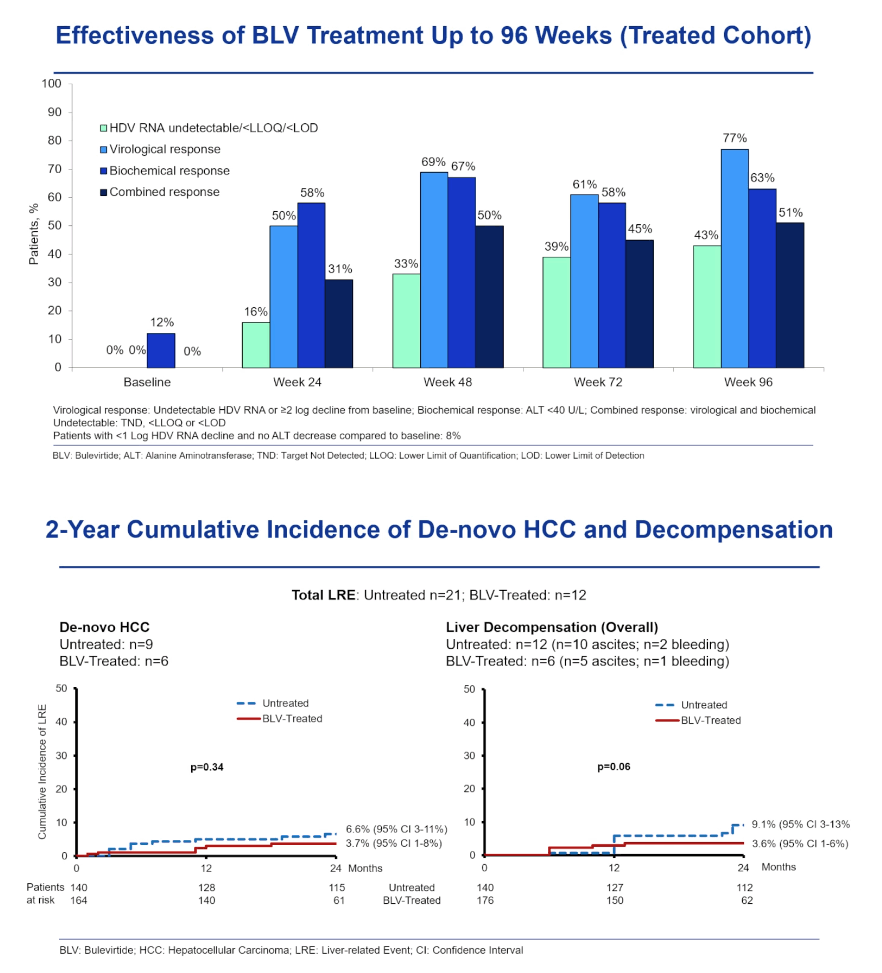
Compared with 140 untreated controls, the 176-person bulevirtide group was older (median 49 vs 40, P < 0.001), included fewer men (59% vs 78%, P = 0.004), and had a higher proportion with prior HCC or decompensation (20% vs 4%, P < 0.0001). Through 24 and 96 weeks of treatment, 16% and 43% of the bulevirtide group reached an undetectable HDV RNA load.
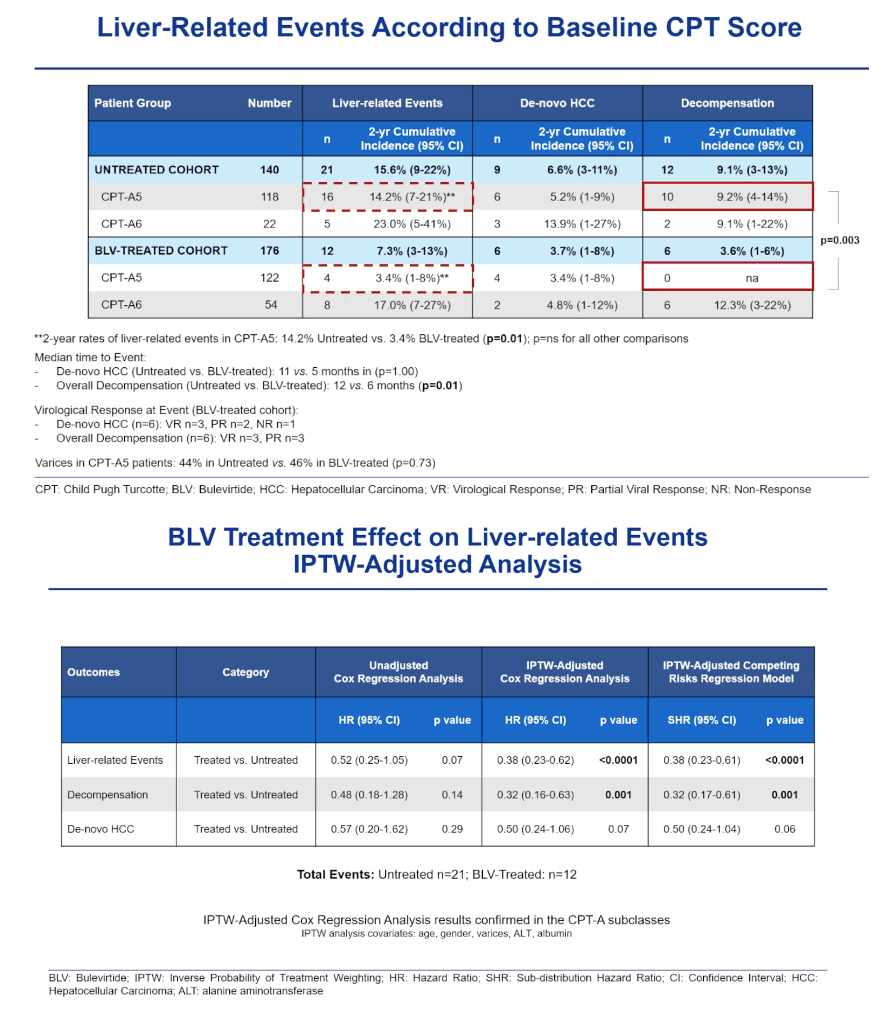
Two-year cumulative incidence of liver decompensation was significantly lower in people taking bulevirtide than in untreated controls (3.6% vs 9.1%, P = 0.04), but rates of newly diagnosed HCC did not differ significantly between the two groups. Inverse probability of treatment weighting (IPTW) Cox regression analysis determined that people taking bulevirtide had about a 60% lower risk of liver-related events (hazard ratio [HR] 0.38, 95% confidence interval [CI] 0.23 to 0.62, P < 0.0001), and an IPTW competing risks model echoed that result. IPTW Cox modeling saw almost a 70% lower risk of decompensation with bulevirtide (HR 0.32, 95% CI 0.16 to 0.63, P = 0.001), again a result virtually mirrored by the competing risks model.
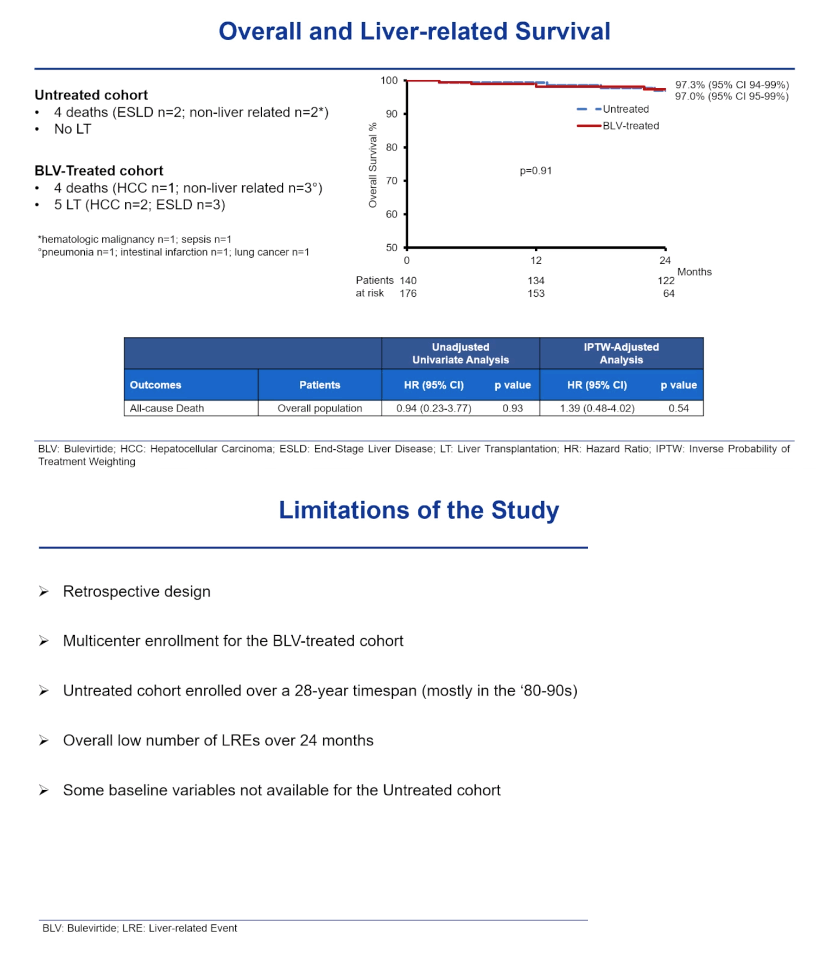
Neither model found an advantage for bulevirtide in new-HCC rate. With 4 deaths in each study group, overall and liver-related survival did not differ between the two study groups.
The researchers noted that the analysis is limited by the 28-year enrollment of untreated controls, mostly in the 1980s and 1990s, by the overall low number of liver-related events in the 24-month study window, and by absence of some baseline variables in the control group. With those caveats in mind, they believe this preliminary analysis "suggests that a 24-month course of bulevirtide monotherapy may prevent decompensation but not HCC in patients with compensated HDV-related cirrhosis."
References
1. Degasperi E, De Silvestri A, Anolli MP, et al. Bulevirtide monotherapy prevents liver decompensation and reduces mortality in patients with HDV-related cirrhosis: a case control study with propensity score weighted analysis. EASL Congress 2024, June 5-8, 2004, Milan. Abstract OS-120.
2. Romeo R, Del Ninno E, Rumi M, et al. A 28-year study of the course of hepatitis Delta infection: a risk factor for cirrhosis and hepatocellular carcinoma. Gastroenterology. 2009;136:1629-38. doi: 10.1053/j.gastro.2009.01.052. https://pubmed.ncbi.nlm.nih.gov/19208358/
-------------------------------
there were a number of critical comments during Q&A saying this study is preliminary in its findings due to limitations of the study, saying we cannot conclude the LREs outcomes found here. better comparison, follow-up is needed. In my opinion that does not mean these findings are not true, it just means a better study design & longer followup is needed to prove it, the results are plausible. Jules

|
| |
|
 |
 |
|
|