 |
 |
 |
| |
Therapeutic Vaccine (BRII-179 Plus siRNA (BRII-835) Stir T-Cell Response Tied to Lower HBsAg
|
| |
| |
EASL Congress 2024, June 5-8, 2004, Milan
Mark Mascolini
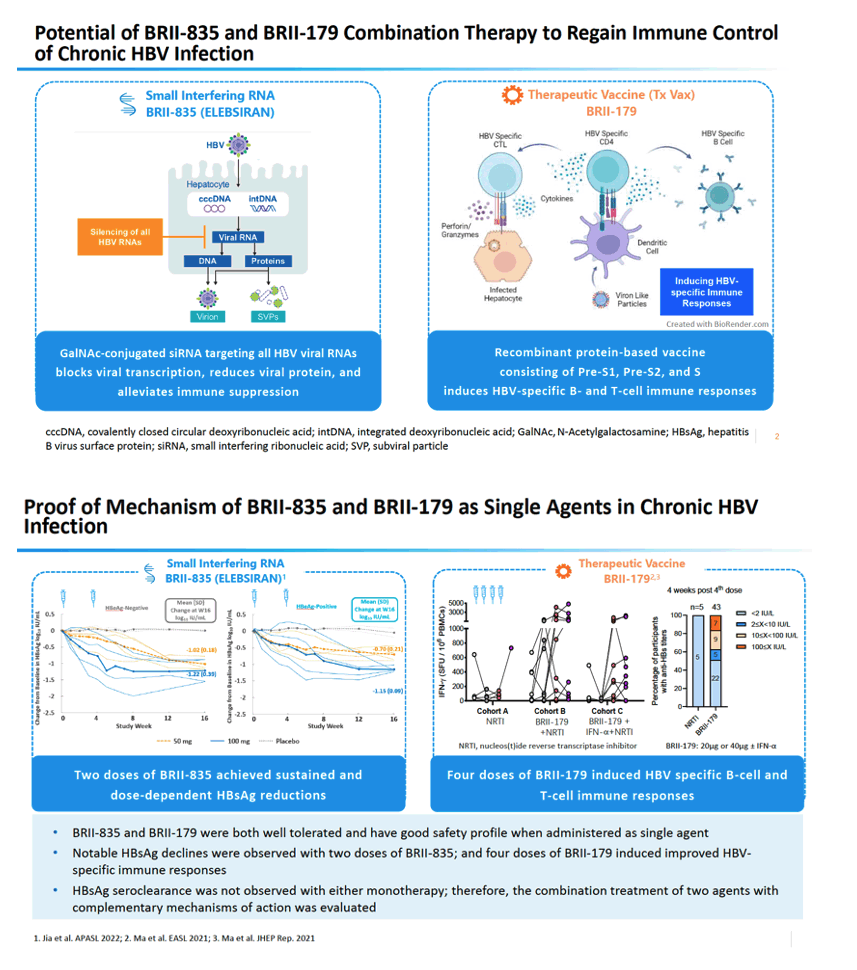
BRII-179, a candidate therapeutic vaccine, provoked a specific T-cell response when combined with the small interfering (si)RNA BRII-835 in certain trial participants with chronic HBV infection [1]. This T-cell response targeting a region adjacent to the NTCP binding site correlated with lower HBsAg in this 11-person analysis. (The sodium taurocholate cotransporting polypeptide, NTCP, swathes the blood side of liver cells and sucks up bile acid [2].)
Derived from the third generation of the prophylactic HBV vaccine PreHevbri, BRII-179 is a particle-based immunotherapeutic containing all 3 HBV surface envelope proteins, Pre-S1, Pre-S2, and S [3]. With about 180 people with chronic HBV infection given up to 9 doses of BRII-179 in 3 phase 1 and 2 clinical trials, the therapeutic vaccine has proved generally safe and well tolerated [3].
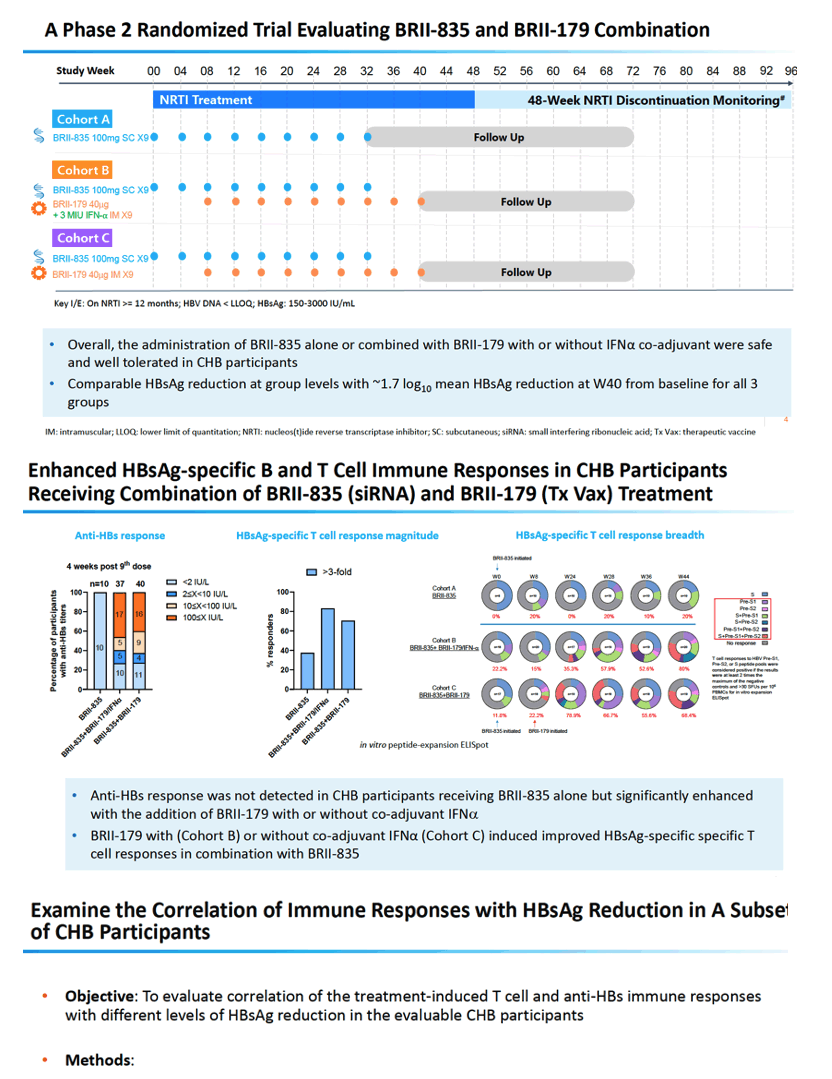
A phase 2 trial randomly assigned 90 people with chronic HBV infection to receive 9 monthly doses of the siRNA BRII-835 (100 mg subcutaneously) alone or in combination with BRII-179 (40 ug) with or without IFNα coadjuvant [4]. Immunologic responses did not differ much between study groups, but they did differ according to how much HBsAg fell.
In the analysis presented as EASL 2024, researchers from Brii Biosciences and collaborators aimed to learn whether specific profiles of treatment-induced anti-HBs and T-cell immune responses correlate with HBsAg decline[1]. The ultimate goal of this ongoing work is to see if combining BRII-179 and BRII-835 will help people regain control of chronic HBV infection.
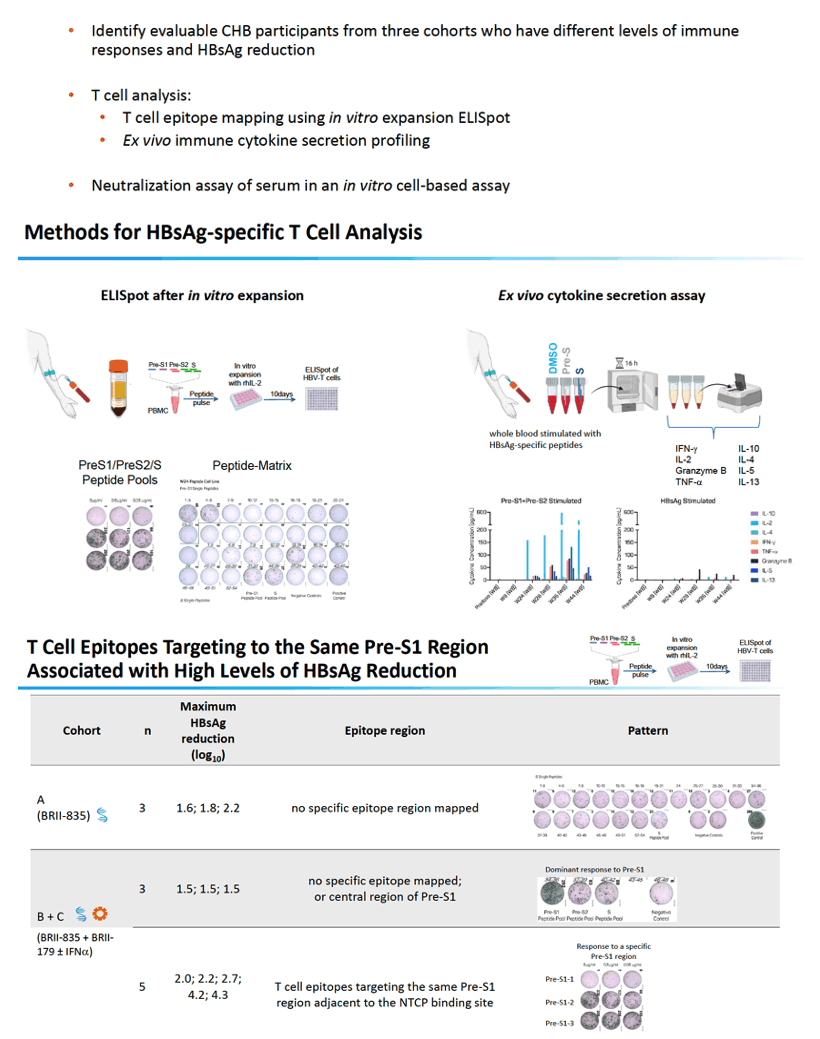
Researchers identified people with chronic HBV infection who differed in levels of immune response to HBsAg reduction. They collected peripheral blood mononuclear cells from (1) 3 people who had taken BRII-835 but not BRII-179 and attained maximum HBsAg drops of 1.6, 1.8, and 2.2 log10, (2) 8 people who had taken BRII-179 with BRII-835, with or without IFNα, who attained maximum HBsAg declines of 1.5, 1.5, 1.5, 2.0, 2.2, 2.7, 4.2, and 4.3 log10.
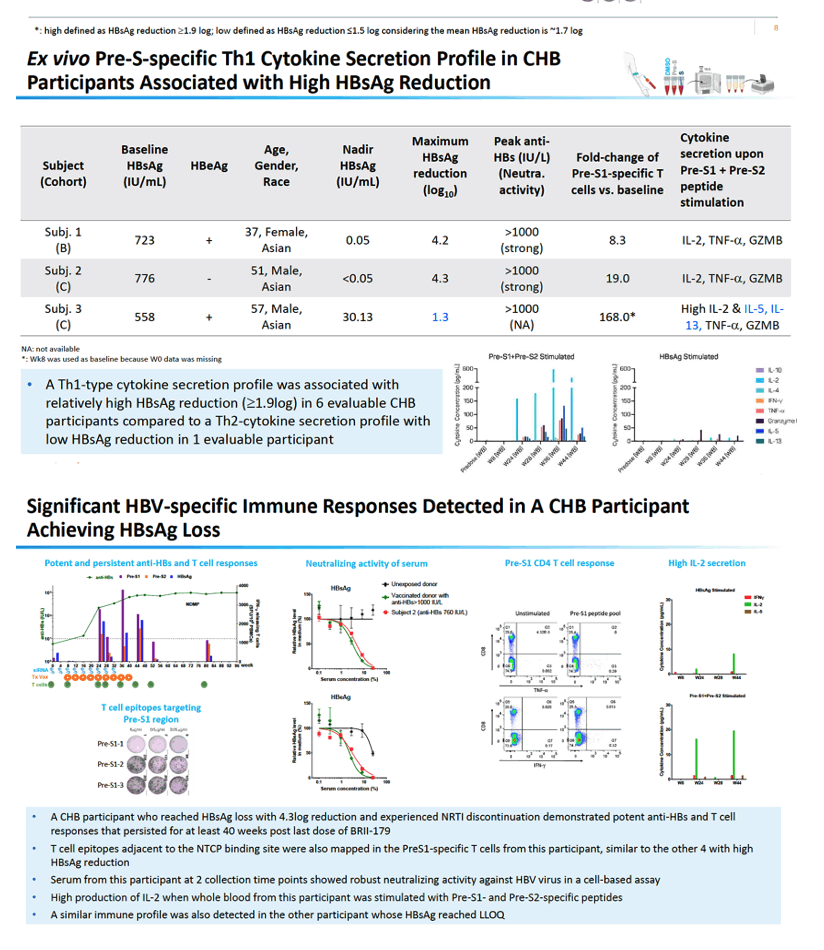
Five participants with T-cell epitopes targeting the same Pre-S1 region near the NTCT binding site had the largest HBsAg drops: 2.0, 2.2, 2.7, 4.2, and 4.3 log10. All of these people got BRII-835 plus BRII-179 with or without IFNα. In 6 study participants, ex vivo analysis linked a pre-S-specific Th1 cytokine secretion profile to bigger declines in HBsAg (at or above 1.9 log10), whereas a Th2-cytokine secretion profile correlated with a lower drop in HBsAg in 1 evaluable participant.
The researchers went on to detect significant HBV-specific immune responses in a person with chronic HBV infection whose HBsAg level plunged 4.3 log10 (more than 10,000-fold). This individual stopped nucleos(t)ide therapy and had potent anti-HBs and T-cell responses lasting for at least 40 weeks after the last dose of BRII-179. Similar to the other 4 people who had large drops in HBsAg, this person also had T-cell epitopes targeting the Pre-S1 region adjacent to the NTCP binding site. Serum sampled from this participant at 2 points demonstrated strong neutralizing activity against HBV in a cell-based assay. The investigators mapped a similar immune profile in another participant whose HBsAg became undetectable.
Brii researchers and collaborators concluded that a Pre-S1-specific T-cell response targeting a region next to the NTCP binding site is tied to large drops in HBsAg in certain people receiving the siRNA BRII-835 and the therapeutic vaccine BRII-179. Ex vivo analysis detected Pre-S1-specific Th1-type cytokines (such as IL-2) in people with bigger falls in HBsAg, but Th2-type responses did not correlate with waning HBsAg. The investigators believe their work shows that the therapeutic vaccine BRII-179 has potent anti-HBV neutralizing activity in people with greater HBsAg reduction and HBsAb induction.
References
1. Ji Y, Le Bert N, Lee A, et al. Therapeutic vaccine (BRII-179) induced immune response associated with HBsAg reduction in a subset of chronic hepatitis B participants. EASL Congress 2024, June 5-8, 2004, Milan. Abstract OS-050. https://www.briibio.com/media/bk0masen/179-835-001_easl-2024-oral.pdf
2. Solvo Biotechnology. NCTP. https://www.solvobiotech.com/transporters/ntcp
3. Gao Z, Yan L, Li J, et al. Functional HBsAb responses induced by BRII-179, a novel HBV therapeutic vaccine, are strongly associated with improved HBsAg loss. Brii Biosciences. Literature archive. Annual Meeting of the Asian-Pacific Association for the Study of the Liver. March 28, 2023. https://www.briibio.com/media/ucsj5igw/mar-28-clinical-12-o-0135-functional-hbsab-responses-induced-by-brii-179-are-strongly-associated-with-improved-hbsag-loss.pdf
4. Ji Y, Le Bert N, Ma H, et al. BRII-179 induced distinct anti-HBs antibody responses in chronic hepatitis B subjects with diverse underlying impairment of humoral immunity. AASLD The Liver Meeting. November 13, 2023.

|
| |
|
 |
 |
|
|