| |
HIV in the Older Adult, Aging/Comorbidities & Death in HIV.......
"Will You Still Treat Me When I'm 64? Care of the Older Adult With HIV Infection"
|
| |
| |
Download the PDF here
(Topics in Antiviral Medicine May/June 2015. IAS/USA......https://www.iasusa.org/tam/mayjune-2015)
HIV infection is associated with chronic immune activation that is superimposed
on immunologic senescence in older adults, resulting in the acquisition
of age-related diseases at younger ages. The incidence of coronary
artery disease is higher among HIV-infected persons than uninfected individuals
matched for age and sex. HIV infection and its treatment have
been associated with premature bone loss. Lung, hepatic, and anal cancers
occur at younger ages in persons with HIV infection. HIV-infected patients
are living longer, and proper attention to the management of comorbidities
in this population is essential. This article summarizes an IAS-USA continuing
education webinar presented by Howard Libman, MD, in January 2015.
Aging/Comorbidities & Death in HIV
Reported by Jules Levin, NATAP
(Table 1. HIV Primary Care Recommendations From the HIV Medicine Association of the Infectious Diseases Society of America........Figure 2. Midpoint life expectancy estimates for individuals diagnosed with HIV infection)
"In general, aging is associated with loss of the physiologic reserves needed to cope with challenges to homeostasis, and all organ systems are affected to some degree"
-------------------
Is HIV a Model of Accelerated or Accentuated Aging? [yes]
http://www.natap.org/2015/HIV/060115_01.htm
J Gerontol A Biol Sci Med Sci (2013)
Sophia Pathai,1,* Hendren Bajillan,2,* Alan L. Landay,3,4 and Kevin P. High5
------------------
"HIV-infected individuals generally acquire age-related diseases at younger chronologic ages than the general population, and it is hypothesized that increased immune activation and long-term chronic inflammation contribute to such premature aging."
"HIV infection, even when controlled, in older adults is associated with chronic immune activation superimposed on immunologic senescence. In the setting of IL-2 downregulation and thymic dysfunction, older HIV-infected individuals may have delayed immune reconstitution. Chronic immune activation has been shown to result in accelerated aging of T cells, and it is unclear if these changes are reversed by antiretroviral therapy.1"
"Additional clinical characteristics of HIV infection in older persons include acquiring age-related diseases at younger ages than uninfected persons. Neurocognitive dysfunction, some non-AIDS-defining cancers, and a wide range of pulmonary diseases are also more prevalent in older HIV-infected individuals. It is hypothesized that increased immune activation and long-term chronic inflammation contribute to premature aging in this population.
With regard to premature aging, a case-control study involving 2854 HIV-infected patients and 8562 uninfected controls treated at Modena University in Italy from 2002 to 2009 examined noninfectious comorbidities, including cardiovascular disease (CVD), hypertension, diabetes, bone fractures, and renal failure.8 Independent predictors of polypathology (P < .001) included older age (odds ratio [OR], 1.11), male sex (OR, 1.77), CD4+ cell count nadir below 200/μL (OR, 4.46), and duration of antiretroviral therapy (OR, 1.01). The prevalence of polypathology among HIV-infected patients aged 41 years to 50 years was similar to that among uninfected participants aged 51 years to 60 years, suggesting that comorbidities occur in HIV-infected individuals approximately 10 years earlier than in their uninfected counterparts.
With regard to cognitive dysfunction, epidemiologic findings indicate that older age is a risk factor for HIV-associated dementia, although there have been few studies in this regard. In a longitudinal study comparing 106 HIV-infected individuals older than 50 years with 96 HIV-infected individuals aged 20 years to 39 years, with multivariate analysis there was a 3-fold higher risk of dementia in the older group after adjusting for race, education level, presence of depression, substance use, antiretroviral therapy status, CD4+ cell count, and viral load.9
With regard to malignancy risk, data from observational studies have suggested that lung, hepatic, and anal cancers occur at younger ages in HIV-infected adults than in uninfected adults. In an analysis of age at diagnosis of non-AIDS-defining cancer using data from 15 HIV and cancer registry databases in the United States, which included data on 212,055 persons with AIDS, lung and anal cancers were found to occur earlier in persons with AIDS than in persons without AIDS (median age 50 years and 54 years, respectively; P < .001) than in the general population.10 In an analysis of 33,420 HIV-infected individuals and 66,840 uninfected controls matched for age, sex, race, and ethnicity in the Veterans Aging Cohort Study, chronic obstructive pulmonary disease, lung cancer, pulmonary hypertension, and pulmonary fibrosis were more frequent among the HIV-infected individuals.11
The incidence of CAD is higher in HIV-infected individuals than in uninfected individuals matched for age and sex, with studies showing increases in both subclinical atherosclerosis (e.g., carotid intima media thickness) and clinical endpoints (eg, acute myocardial infarction [MI]). HIV infection is associated with increased soluble and cellular markers of inflammation, endothelial dysfunction, and altered coagulation, all of which contribute to risk of CVD.
Available data suggest a 50% increased risk of acute MI among middle-aged or older HIV-infected individuals compared with uninfected individuals of the same age.
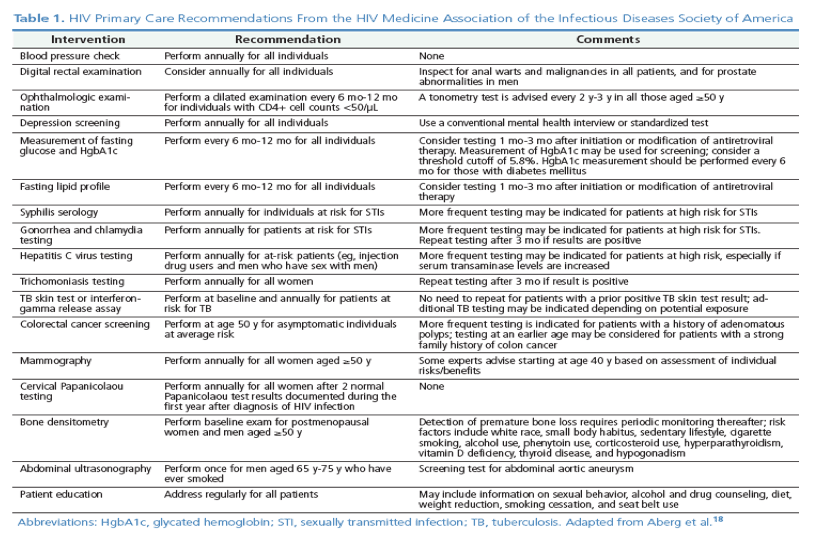
Premature Bone Loss: Current HIV primary care guidelines from the HIV Medicine Association of the Infectious Diseases Society of America (IDSA) recommend bone densitometry screening for men aged 50 years or older and for postmenopausal women.18 Radiography or magnetic resonance imaging for avascular necrosis of the hips should be performed for symptomatic patients only.
Osteopenia, osteoporosis, and pathologic fractures have been described in the context of HIV infection. Osteoporosis may present with fractures of vertebrae, forearms, or hips. HIV infection itself, use of tenofovir or protease inhibitors, alterations in metabolism of vitamin D, and lactic academia related to use of older nRTIs may be contributing factors to premature bone loss.
Immobility, cigarette smoking, excessive alcohol use, chronic renal disease, hypogonadism, hyperparathyroidism, hyperthyroidism, and steroid use accentuate bone loss. The optimal use of bone densitometry as a screening test for HIV-infected individuals is uncertain. Calcium and vitamin D supplements should be given to high risk patients, and regular exercise and smoking cessation should be advised."
"Lung, hepatic, and anal cancers occur at younger ages in HIV-infected adults than in uninfected adults. The incidence of CAD is higher among HIV-infected individuals than among uninfected individuals matched for age and sex. Results of CAD risk calculation should be interpreted in the context of this increased risk. HIV infection and its treatments have been associated with premature bone loss. Age-related immunizations and screening tests for cancers and other conditions should be addressed. Mortality in HIV-infected persons has decreased substantially over the past 2 decades, with non-AIDSrelated conditions now accounting for the majority of deaths."
"Available data on mortality trends include those from the D:A:D (Data Collection on Adverse Events of Anti-HIV Drugs) study, which has been ongoing since 1999. There have been 3909 deaths observed in the study among 49,731 patients followed up through 2011, and the overall crude mortality rate is 12.7 per 1000 person-years, although it decreased from 16.9 per 1000 person-years to 9.6 per 1000 person years over the follow-up period. Twenty-nine percent of deaths were attributable to AIDS-related causes, 15% to non-AIDS-related cancers, 13% to liver disease, and 11% to CVD [from Jules: so comorbidities related deaths surpass AIDS-related deaths: 39% vs 29%]. Over the course of follow-up, the proportion of deaths attributable to AIDS-related events has decreased from 34% to 22% and the proportion attributable to non-AIDS-defining malignancies has increased from 9% to 23%.24"
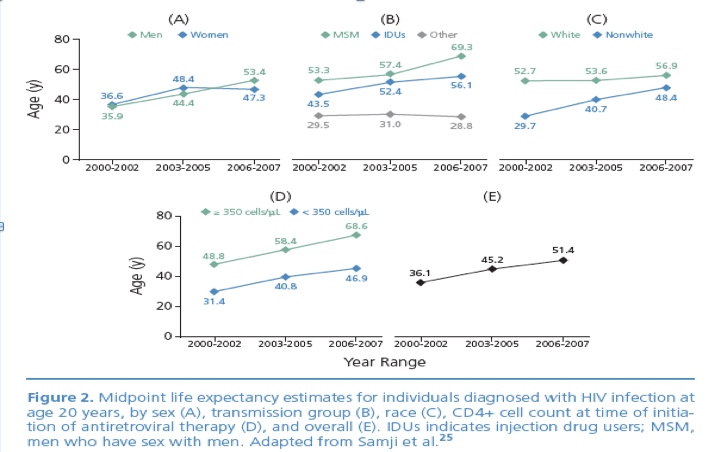
Figure 2. Midpoint life expectancy estimates for individuals diagnosed with HIV infection at
age 20 years, by sex (A), transmission group (B), race (C), CD4+ cell count at time of initiation
of antiretroviral therapy (D), and overall (E). IDUs indicates injection drug users; MSM,
men who have sex with men. Adapted from Samji et al.25
|
|
| |
| |
|
|
|