| |
Doctors Spend 30% of Their Time With Patient
|
| |
| |
Download the PDF here
Download the PDF here
Sometimes It Feels like Doctors Have No time To Spend With Patients, are EHR helping or harming patient Care
6 December 2016
Allocation of Physician Time in Ambulatory Practice: A Time and Motion Study in 4 Specialties
Christine Sinsky, MD; Lacey Colligan, MD; Ling Li, PhD; Mirela Prgomet, PhD; Sam Reynolds, MBA; Lindsey Goeders, MBA; Johanna Westbrook, PhD; Michael Tutty, PhD; George Blike, MD
Our finding that physicians interact with an EHR during 37.0% of the time they spend with patients is consistent with other studies, using different methods, that showed that one third of patient time is spent using an EHR (32, 33). The burden of EHR and desk work and administrative tasks (10, 12, 31, 34–36) and increases in documentation time after EHR introduction have been described (1).
Results:
During the office day, physicians spent 27.0% of their total time on direct clinical face time with patients and 49.2% of their time on EHR and desk work. While in the examination room with patients, physicians spent 52.9% of the time on direct clinical face time and 37.0% on EHR and desk work. The 21 physicians who completed after-hours diaries reported 1 to 2 hours of after-hours work each night, devoted mostly to EHR tasks.
Conclusion:
For every hour physicians provide direct clinical face time to patients, nearly 2 additional hours is spent on EHR and desk work within the clinic day. Outside office hours, physicians spend another 1 to 2 hours of personal time each night doing additional computer and other clerical work.
Use of EHRs has brought the promise of many advances in patient care, although recent analyses have shown a gap between expectations and outcomes (27–29). Increasing demands associated with EHRs and meaningful use requirements can produce unintended negative consequences (1, 2). For example, one might hypothesize that new EHR activities decrease the time physicians spend engaging with patients. Our data quantify previous survey data showing that physicians report spending substantial work time using the EHR (6, 30). These previous studies have suggested that decreased time with patients and increased workload from EHR tasks are major contributors to career dissatisfaction among physicians. Furthermore, changes in physician work activity patterns are associated with high physician burnout rates that increased rapidly between 2011 and 2014 (5).
In the context of rapid change, dissatisfaction among physicians with how their time and skills are used is widespread and growing. Fifty-four percent of U.S. physicians experience some sign of burnout (5), an increase from 46% (6) over a 3-year period, 2011 to 2014, (P < 0.001). Time spent in meaningful interactions with patients and the ability to provide high-quality care are powerful drivers of physician career satisfaction (4). Conversely, physician dissatisfaction has centered on the changing content of their work, with more time spent on paperwork and the computer (7) and less time available for direct clinical face time with patients (4). Correlations between increases in EHR task load and physician burnout and attrition have also been shown (7, 8).
The observational data reflect both examination room and non–examination room time (for example, workstation or office). Physicians in our study spent 33.1% of this total time on direct clinical face time: 27.0% with patients in the examination room, and 6.1% with staff when the patient was not present (for example, speaking with a nurse in a workstation room) (Table 4).
Nearly half of physicians' total time (49.2%) was spent on EHR and desk work. Of this time, 38.5% was spent on documentation and review tasks, with the remainder spent on test results (6.3%), medication orders (2.4%), and other orders (2.0%). Physicians spent 1.1% of their time on administrative tasks, of which 0.6% involved insurance-related tasks and 0.5% involved scheduling (Table 4).
Physicians in our sample spent 47.7% of their time in the examination room with patients (205 hours). During this time, they spent 52.9% of their time on direct clinical face time with patients, 37.0% on EHR and desk work, 9.3% on administrative tasks, and 0.8% on other tasks.
Our results suggest that documentation support with either dictation or assistant services may increase direct clinical face time with patients. This is consistent with studies demonstrating benefits from sharing documentation and order entry tasks with team members, including saving physician time (37), boosting productivity (38), increasing capacity and thus access for patients (39), improving quality of documentation (40), and improving patient and provider satisfaction (35, 41). Optimization of documentation support may be achieved through models of advanced teamwork (42–46) or documentation assistants (37, 38, 40, 41, 47).
---------------------------
Electronic Health Record Logs Indicate That Physicians Split Time Evenly Between Seeing Patients And Desktop Medicine
April 2017
Abstract
Time spent by physicians is a key resource in health care delivery. This study used data captured by the access time stamp functionality of an electronic health record (EHR) to examine physician work effort. This is a potentially powerful, yet unobtrusive, way to study physicians’ use of time. We used data on physicians’ time allocation patterns captured by over thirty-one million EHR transactions in the period 2011–14 recorded by 471 primary care physicians, who collectively worked on 765,129 patients’ EHRs. Our results suggest that the physicians logged an average of 3.08 hours on office visits and 3.17 hours on desktop medicine each day. Desktop medicine consists of activities such as communicating with patients through a secure patient portal, responding to patients’ online requests for prescription refills or medical advice, ordering tests, sending staff messages, and reviewing test results. Over time, log records from physicians showed a decline in the time allocated to face-to-face visits, accompanied by an increase in time allocated to desktop medicine. Staffing and scheduling in the physician’s office, as well as provider payment models for primary care practice, should account for these desktop medicine efforts.
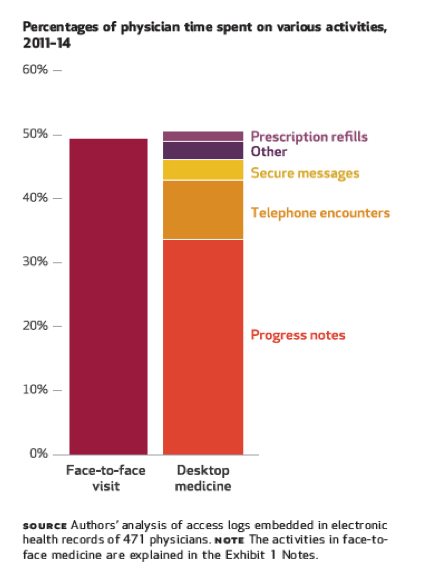
Of the time spent on desktop medicine, an average of 2.82 hours was spent in the clinic, with 1.42 hours spent on patients who were seen on the same day and 1.40 hours spent on other patients ( Exhibit 1 ). An average of 0.35 hour was spent on secure remote computers, 0.14 hour for patients who were seen on the same day and 0.21 hour for other patients. The primary desktop medicine activity both in the clinic and remotely was typing progress notes. Physicians generally spent more time on progress notes in the clinic on visit days. Other desktop medicine activities, in descending order of time allotted, were logging telephone encounters, exchanging secure messages with patients, and refilling prescriptions. Common desktop medicine activities for patients not seen that day were orders for services, chart reviews, letters for external use, and scanned documents.
This is one of the first studies to use EHR access logs that identify discrete, time-stamped activities to account at least partially for how physicians allocate their time. The time recorded for desktop medicine corroborates previous reports of the extensive time spent by physicians on activities outside of direct face-to-face visits. 6 , 9 – 11 Our results suggest that physicians spent comparable time in face-to-face visits (3.08 hours per day) and desktop medicine (3.17 hours per day). If we add three minutes to face-to-face visit time to account for the time between entry and first login and the time between last logout and exit, the average visit length comes to about 18.0 minutes, which is consistent with the literature. 7 Multiplying 18 minutes by 12.3 (the average number of visits per day) gives us an average of 3.69 hours per day spent on face-to-face visits. We acknowledge, however, that this approach omits work efforts that were not captured by log data, such as phone calls and searching for answers to patients’ questions. Findings from a recent direct-observation study of fifty-seven physicians sponsored by the American Medical Association (AMA) showed that about 19.9 percent of physicians’ time per day was spent on tasks other than direct clinical face time, EHR and desk work, and administrative tasks, including personal time, transit time within the clinic, and unobserved work. 6 Combining those results with our findings produces an approximation of how physicians spend time in ambulatory practice in the age of EHRs and patient portals: 40 percent is spent on face-to-face visits, 40 percent on desktop medicine, and 20 percent on other activities that are not logged in the EHR.
Our research provides empirical data that support this change in physician payment policy. Of the 765,129 patients whose EHRs were accessed by the 471 physicians in the four years of our study, only 637,769 had one or more face-to-face visits. The remaining 127,360 patients received desktop medicine service only. Moreover, consumers increasingly prefer services other than face-to-face visits: A recent survey of several thousand Americans found that 74 percent preferred “virtual” encounters to face-to-face office visits. 32 Our results showed that activities associated with virtual encounters included telephone encounters (documenting telephone encounters took up 9 percent of physicians’ logged time), communicating with patients via the secure patient portal (3 percent), and refilling prescriptions (2 percent). Compensation models should make delivering services in ways that meet patients’ preferences the easy thing to do.
CMS has indicated its intention to monitor practices to ensure the delivery of high-quality health care under the Comprehensive Primary Care Plus model. Access logs provide a simple and unobtrusive way for health care delivery systems to examine how their clinicians spend a significant portion of their time. The effective use of such data can help create true learning health systems capable of assessing how best to deploy clinical and other resources to maximize the value of their services to patients.
|
|
| |
| |
|
|
|