| |
Use of nucleoside reverse transcriptase inhibitors and risk of myocardial infarction in HIV-infected patients enrolled in the D:A:D study: a multi-cohort collaboration
|
| |
| |
Download the PDF here
D:A:D Study Group
Published:April 02, 2008
Summary
Background
Whether nucleoside reverse transcriptase inhibitors increase the risk of myocardial infarction in HIV-infected individuals is unclear. Our aim was to explore whether exposure to such drugs was associated with an excess risk of myocardial infarction in a large, prospective observational cohort of HIV-infected patients.
Methods
We used Poisson regression models to quantify the relation between cumulative, recent (currently or within the preceding 6 months), and past use of zidovudine, didanosine, stavudine, lamivudine, and abacavir and development of myocardial infarction in 33 347 patients enrolled in the D:A:D study. We adjusted for cardiovascular risk factors that are unlikely to be affected by antiretroviral therapy, cohort, calendar year, and use of other antiretrovirals.
Findings
Over 157 912 person-years, 517 patients had a myocardial infarction. We found no associations between the rate of myocardial infarction and cumulative or recent use of zidovudine, stavudine, or lamivudine. By contrast, recent-but not cumulative-use of abacavir or didanosine was associated with an increased rate of myocardial infarction (compared with those with no recent use of the drugs, relative rate 1⋅90, 95% CI 1⋅47-2⋅45 [p=0⋅0001] with abacavir and 1⋅49, 1⋅14-1⋅95 [p=0⋅003] with didanosine); rates were not significantly increased in those who stopped these drugs more than 6 months previously compared with those who had never received these drugs. After adjustment for predicted 10-year risk of coronary heart disease, recent use of both didanosine and abacavir remained associated with increased rates of myocardial infarction (1⋅49, 1⋅14-1⋅95 [p=0⋅004] with didanosine; 1⋅89, 1⋅47-2⋅45 [p=0⋅0001] with abacavir).
Interpretation
There exists an increased risk of myocardial infarction in patients exposed to abacavir and didanosine within the preceding 6 months. The excess risk does not seem to be explained by underlying established cardiovascular risk factors and was not present beyond 6 months after drug cessation.
Funding
HAART Oversight Committee.
Introduction
Antiretroviral therapy continues to provide durable clinical benefit to individuals who are infected with HIV. 1 However, as survival has improved, several conditions associated with an ageing population have emerged as health concerns; 2 in particular, cardiovascular disease now contributes to more than 10% of deaths among HIV-infected individuals. 3, 4Although factors that affect cardiovascular risk in the general population seem to be similarly associated with cardiovascular risk in HIV-infected individuals,5, 6, 7exposure to antiretroviral therapy has also been shown to adversely affect the risk of cardiovascular disease.6, 7To date, the focus has been on antiretroviral drugs from the protease inhibitor (PI) class because of their tendency to cause dyslipidaemia.8, 9 Continued exposure to PIs has been shown to be associated with an increasing risk of myocardial infarction.6, 10, 11
However, PIs are usually prescribed in combination with drugs from the nucleoside reverse transcriptase inhibitor (NRTI) class.12In an analysis of the Data Collection on Adverse Events of Anti-HIV Drugs (D:A:D) study, controlling for exposure to NRTIs reduced the association between exposure to PIs and the risk of myocardial infarction, suggesting that NRTIs could also contribute to cardiovascular risk.6 Two of these drugs, the thymidine analogues stavudine and zidovudine, have been associated with development of dyslipidaemia and impaired insulin resistance,13, 14, 15, 16, 17 an increased risk of diabetes mellitus,18, 19, 20 and greater intima media thickness. 21, 22 Thus, exposure to NRTIs, and the thymidine analogues in particular, could plausibly contribute to increased risk of cardiovascular disease.
We designed a series of analyses to explore whether exposure to NRTIs was associated with an excess risk of myocardial infarction in a large, prospective observational cohort of HIV-infected patients. Although our primary hypothesis focused on exposure to stavudine and zidovudine, for completeness, we did the same analyses for other NRTIs for which there was sufficient exposure in the D:A:D cohort.
Methods
D:A:D is an international collaboration of 11 cohorts, following 33 347 HIV-1-infected individuals at 212 clinics in Europe, the USA, and Australia. 6 , 7 ,23 All participants were under active follow-up in their cohorts at the time of enrolment into D:A:D (December, 1999, to January, 2005). Sociodemographic, clinical, treatment (antiretroviral and other medications received both before and after enrolment), and laboratory data are collected. For the purpose of our analyses, hypertension is defined as a systolic blood pressure greater than 140 mm Hg, diastolic blood pressure over 90 mm Hg, or if the patient is in receipt of anti-hypertensive medication. Dyslipidaemia is deemed to be present if total cholesterol is greater than 6⋅2 mmol/L, HDL cholesterol below 0⋅9 mmol/L, triglyceride greater than 2⋅3 mmol/L, or if the patient is in receipt of lipid-lowering drugs.
All incident cases of myocardial infarction are reported to the study coordinating office for validation and coding.7 Reported myocardial infarctions are classified as definite, possible, or unclassifiable according to criteria applied in the WHO MONICA study,24 independently of knowledge of a patient's antiretroviral treatment history. Other validated outcomes include strokes (definitive or possible), invasive cardiovascular procedures (coronary artery angioplasty or bypass, or carotid endarterectomy), diabetes mellitus, and death.
Statistical analysis
The analysis plan specified that assessment of the rate of myocardial infarction affected by the individual drugs would be done only when the study had accrued sufficient follow-up among individuals receiving each drug to permit a robust analysis. This objective was reached for the five most commonly used NRTIs (zidovudine, stavudine, didanosine, lamivudine, and abacavir) in 2007. The analysis presented here is based on myocardial infarctions and other cardiovascular outcomes that had occurred up to Feb 1, 2007.
Full details of the analytical approach have been described.7 Individuals were followed prospectively from enrolment in D:A:D to the date of the first myocardial infarction, the date of death, 6 months after a patient's last clinic visit, or Feb 1, 2007, whichever occurred first. Each person's follow-up was divided into a series of consecutive 1-month periods, and a patient's cumulative exposure to each antiretroviral drug at the start of each period was calculated (including exposure to treatment before enrolment). This information was used to assign the patient-month (and any events that occurred) to the appropriate exposure category. Each person's covariate data was also updated at the start of each month, permitting a time-varying analysis.
Poisson regression models (GENMOD procedure, SAS version 9.1) were used to quantify the relation between exposure to each NRTI and the rate of myocardial infarction. We postulated that cumulative exposure to zidovudine and stavudine would be associated with an increased risk of myocardial infarction, while no such effect would be detected with exposure to other NRTIs. Thus, the initial pre-planned analyses incorporated five continuous covariates measuring cumulative exposure to each NRTI. This model, and all subsequent models, was also adjusted for demographic factors (age, sex, HIV transmission group, and ethnic origin), calendar year, cohort, cardiovascular risk factors that are unlikely to be associated with use of combination antiretroviral therapy (smoking status, family history of cardiovascular disease, previous cardiovascular event, body-mass index), and cumulative exposure to other antiretroviral drugs (zalcitabine, tenofovir, and the main PIs and non-nucleoside reverse transcriptase inhibitors [NNRTIs] in use during the study, each included individually). These models did not adjust for factors that could lie on the causal pathway between receipt of each drug and the development of myocardial infarction (ie, abnormal serum lipids, development of diabetes, raised blood pressure, etc). Specific categories were generated for missing data (eg, unknown family history) to ensure that all individuals and observed events were included. Exploratory analyses then categorised cumulative exposure to each drug (as none, <1, 1-2, 2-3, 3-4, 4-5, 5-6, and >6 years) to determine the linearity of any associations. Subsequently, as a consequence of these findings, we investigated whether risk of myocardial infarction was associated with recent use (defined as current use or use within the previous 6 months) of each drug (as binary time-updated covariates with patients being categorised at the start of each patient-month) and determined whether the relation was potentially reversible by the inclusion of dummy variables to additionally capture past use (last use >6 months previously). All analyses were based on the first myocardial infarction that occurred during follow-up; patients developing a myocardial infarction during follow-up did not contribute further person-months of follow-up thereafter. All p values are two-sided.
In line with previous analyses of this dataset, we assessed whether any effects could be mediated through changes in the levels of other risk factors for myocardial infarction that have been shown to be modified by combination antiretroviral therapy, including serum lipids (total cholesterol, HDL cholesterol, and triglycerides [log2-transformed]), systolic and diastolic blood pressure, glucose, and the presence of diabetes or physician-defined lipodystrophy. This was achieved by the incorporation of the latest measurements of each of these variables as a time-updated covariate into the Poisson regression model (again, defined at the start of each patient-month). All lipid measurements were included, irrespective of fasting status. For analyses of serum lipids and blood pressure, follow-up was additionally left-truncated at the time of a patient's first measurement of each marker to allow for the fact that measurements might have been unavailable in earlier calendar years; each variable was deemed to be a continuous covariate in these analyses. By contrast, because glucose monitoring did not become routine in this group until more recently, the latest glucose concentration was incorporated as a categorical covariate with an additional category for missing values. Combined with adjustment for other risk factors that were unlikely to be affected by combination antiretroviral therapy, this analysis in effect additionally controls for any differences in patient characteristics at the time of starting each drug. We also considered whether any effects could be explained by different disease-related responses (ie, changes in viral load or CD4 cell count) to combination antiretroviral therapy in those receiving different NRTIs by incorporating the latest recorded value for these variables as time-updated covariates.
We did a further series of sensitivity analyses to investigate possible explanations for unexpected findings. First, we excluded follow-up time or events that occurred in the first 2 months after starting abacavir to exclude the possible effect of hypersensitivity reactions to abacavir. Second, we incorporated interaction terms between recent and cumulative exposure to each NRTI to identify whether an effect of cumulative exposure remained in those recently exposed but not in those without recent exposure to each drug. Lastly, we studied whether the association between each NRTI and the risk of myocardial infarction differed according to whether the patient had also recently received a PI or NNRTI (by including an interaction term between recent use of each NRTI and recent use of either the PI or NNRTI drug class), and also adjusted our analyses for recent (rather than just cumulative) exposure to each PI.
To place our results into clinical context, patient follow-up and events were also classified according to the patient's latest predicted 10-year risk of coronary heart disease, as determined by the Framingham equation 25 (assuming that left ventricular hypertrophy had not been diagnosed). Patients were categorised as being at high (>20% risk; this group also included all patients with a personal history of cardiovascular disease), moderate (10-20% risk), low (<10% risk), or unknown risk (where the predicted risk of coronary heart disease could not be assessed because of missing data). Rates of myocardial infarction were calculated after stratification of the patients according to their predicted 10-year risk of coronary heart disease, as well as recent exposure to the NRTIs. The predicted 10-year risk of coronary heart disease was added to the main Poisson regression model; interactions with recent exposure to each drug were investigated to see whether the effect of either drug seemed to be different in those at moderate or high predicted risk, compared with those at low or unknown predicted risk.
To further investigate whether there was any potential for our results to be affected by channelling bias (ie, the possibility that patients at high underlying risk of cardiovascular disease were preferentially treated with certain antiretroviral regimens), we compared, for each NRTI, the cardiovascular risk profiles and treatment histories of patients under prospective follow-up who had recently received the drug with those that had not.
Role of the funding source
The study sponsors had no role in the design or conduct of the study, or in the collection or analysis of the data. Members of the oversight committee commented on the manuscript and interpretation of results, but there was no obligation for the study group to incorporate any of their suggestions. The D:A:D steering committee made the decision to publish the results and the members of the writing group had full access to the database. Caroline Sabin and the corresponding author had full access to the dataset.
Results
By Feb 1, 2007, 33 347 patients had been followed up for a total of 157 912 person-years (median 5⋅1 [IQR 3⋅2-6⋅5] years per person) over which time 517 patients had a myocardial infarction (event rate 3⋅3 [95% CI 3⋅0-3⋅6] per 1000 person-years). Of these patients, 284 (55%) were white and 304 (59%) had a homosexual risk for HIV infection. 509 individuals who had a myocardial infarction had been exposed to antiretroviral therapy, 59 of whom were off therapy at the time of their myocardial infarction. At the last test before diagnosis of myocardial infection, median CD4 cell count was 420 (range 1-1686) cells per μL; median nadir CD4 cell count was 130 (0-1020) cells per μL. 262 (51%) of these patients had a viral load of less than 50 copies per mL at the last reading before diagnosis of myocardial infarction.
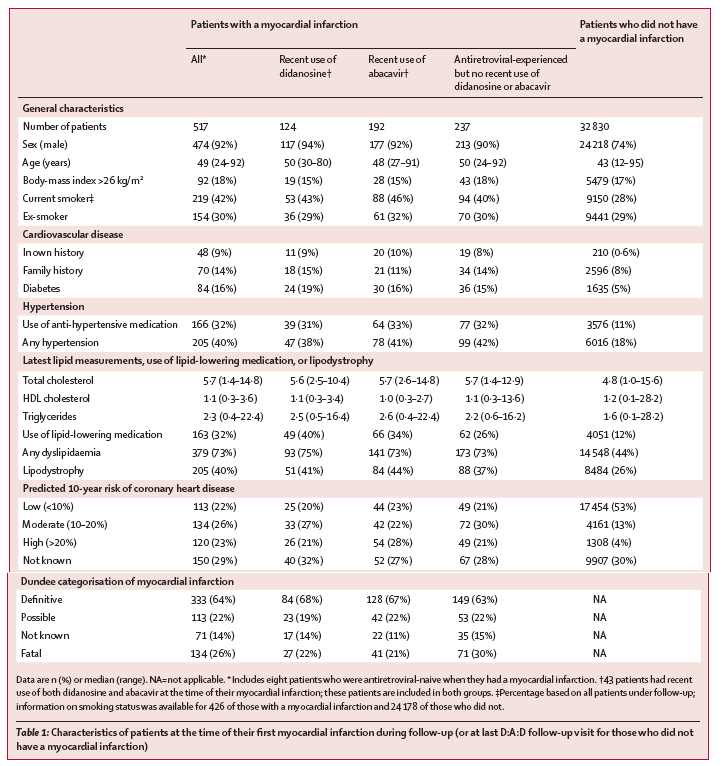
Patients who had a myocardial infarction were older, more often were men and current smokers, and more often had a family history of cardiovascular disease, or were more likely to have been diagnosed with diabetes mellitus, hypertension, lipodystrophy, or dyslipidaemia than were individuals who did not have such an event (table 1). More patients who had a myocardial infarction had a high or moderate predicted 10-year risk of coronary heart disease than did those who did not have a myocardial infarction (table 1). When analyses were restricted to only those with sufficient data to calculate risk, 120 (33%) patients who had a myocardial infarction were at high risk and 134 (37%) were at moderate risk compared with only 1308 (6%) and 4161 (18%) patients who had not had a myocardial infarction, respectively. 29629 (90%) patients who not had a myocardial infarction had been exposed to antiretroviral therapy.
In a regression model that incorporated cumulative exposure to each NRTI, there were no significant associations between the development of myocardial infarction and exposure to zidovudine, stavudine, or lamivudine (table 2; model 1). However, longer duration of exposure to didanosine and abacavir was associated with an increased rate of myocardial infarction (table 2; model 1). Initial analyses of the associations with use of didanosine and abacavir revealed that the rate of myocardial infarction increased rapidly after first use of each drug and remained high thereafter compared with patients not taking these drugs (data not shown).
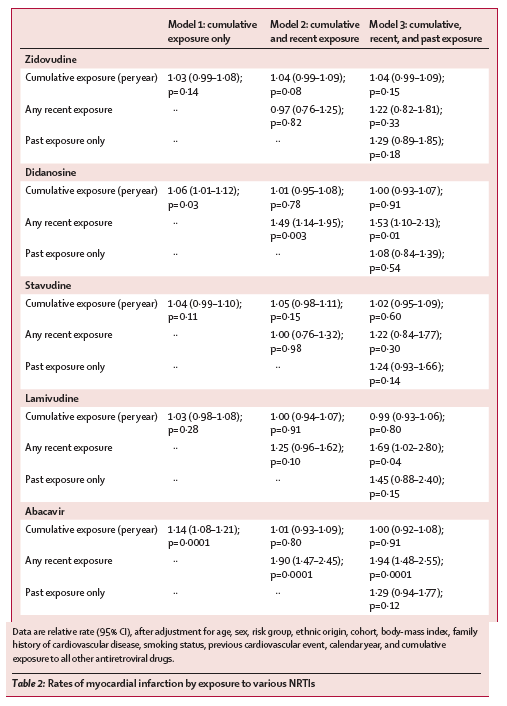
The rate of myocardial infarction was significantly increased with recent use of didanosine or abacavir (table 2; model 2). The rate of myocardial infarction was 49% greater in patients who had recently used didanosine and 90% greater in those who had recently used abacavir than in those who had never used or who last used these drugs more than 6 months previously (table 2; model 2). After adjustment for recent use of didanosine and abacavir, no evidence remained of an increased risk associated with increasing exposure to each drug (table 2; model 2). By contrast, there were no significant associations with recent or cumulative use of other NRTIs.
There were no associations between the rate of myocardial infarction and past exposure to any of the NRTIs when we incorporated covariates for past use of each drug (table 2; model 3); recent use of didanosine and abacavir remained significantly associated with an increased rate of myocardial infarction. In this model the comparator group consisted of patients who had never used the drug in question. Recent use of lamivudine was also associated with an increased rate of myocardial infarction (table 2; model 3).
Additional sensitivity analyses resulted in consistent findings, even after exclusion of follow-up time and events in the first 2 months after starting abacavir and after consideration of cumulative exposure to each NRTI as a categorical rather than continuous variable (data not shown). In each case, recent-but not cumulative-exposure to didanosine or abacavir was most strongly associated with the development of myocardial infarction. There was no evidence of an interaction between recent and cumulative exposure (data not shown). Our analyses did not reveal any significant interaction between recent use of didanosine or abacavir and recent use of either the PI or NNRTI class of drugs, and results were unchanged when analyses additionally controlled for recent use of each PI (as opposed to cumulative exposure only; data not shown).
The characteristics of patients at the time of myocardial infarction were similar in those recently exposed to didanosine, those recently exposed to abacavir, and those who were antiretroviral-experienced but had not recently been exposed to either drug (table 1). In particular, there was no evidence that the classification of myocardial infarction differed, or that myocardial infarctions were more likely to be fatal in any one group.
Patients who started abacavir or didanosine for the first time while under follow-up in D:A:D generally had worse cardiovascular risk profiles than did those who started the other NRTIs for the first time: 1119 (27%) of 4076 patients first starting abacavir and 383 (22%) of 1731 first starting didanosine had moderate or high predicted 10-year risk of coronary heart disease compared with 414 (19%) of 2177, 139 (19%) of 741, and 474 (19%) of 2546 patients first starting zidovudine, stavudine, and lamivudine, respectively. When we analysed all patients who started or switched to each NRTI (including those who restarted these drugs) during follow-up, the differences between the groups remained but were less marked: 1651 (26%) of 6266 patients starting or switching to abacavir and 1081 (24%) of 4486 patients starting or switching to didanosine had a moderate or high predicted 10-year risk of coronary heart disease compared with 1611 (22%) of 7461, 607 (23%) of 2650, and 2627 (22%) of 12 085 patients starting or switching to zidovudine, stavudine or lamivudine, respectively.
Table 3 shows the characteristics of patients under follow-up with recent use of each NRTI, compared with those without recent use; the webtabledescribes concomitant use of other antiretroviral drugs as well as treatment history. Patients with recent exposure to abacavir were more likely to be men, older, and to have diabetes, hypertension, dyslipidaemia, or a personal or family history of cardiovascular disease than those with no recent exposure to abacavir, but were less likely to be smokers or to have a high body-mass index. Patients with recent exposure to didanosine did not differ greatly from those without recent exposure to this drug. For other NRTIs there was generally little difference between those with and without recent use, although most drugs (with the exception of zidovudine) seemed to be associated with diabetes and dyslipidaemia to some degree.
Figure 1 shows the observed rates of myocardial infarction stratified by predicted 10-year risk of coronary heart disease as well as by recent exposure to didanosine or abacavir. In those who had no recent use of didanosine, rates of myocardial infarction were 1⋅3, 6⋅0, and 19⋅4 events per 1000 person-years in those with low, moderate, and high predicted risk of coronary heart disease, respectively. In those who had recently used the drug, rates were higher, with 1⋅8, 7⋅7, and 23⋅1 events per 1000 patient-years for those with low, moderate, and high risk of coronary heart disease. In the same categories of risk, rates of myocardial infarction were 1⋅0, 5⋅9, and 15⋅9 events per 1000 patient-years in those with no recent abacavir use, but 2⋅9, 7⋅7, and 32⋅5 events per 1000 patient-years in those with recent use of abacavir.
After incorporation of the predicted 10-year risk of coronary heart disease into the main regression model of cumulative and recent exposure to NRTIs, the rate of myocardial infarction was increased both in those with moderate and in those with high 10-year risk of coronary heart disease, compared with those with a low 10-year risk (relative rate 2⋅19, 95% CI 1⋅64-2⋅92 [p=0⋅0001] for those with moderate risk; 3⋅22, 2⋅27-4⋅57 [p=0⋅0001] for those with high risk). After adjustment for the predicted 10-year risk of coronary heart disease, recent use of both didanosine and abacavir remained significantly associated with increased rates of myocardial infarction (relative rate 1⋅49, 1⋅14-1⋅95 [p=0⋅004] for didanosine; 1⋅89, 1⋅47-2⋅45 [p=0⋅0001] for abacavir compared with those who had never received or who had only past exposure to the drugs). There was no significant interaction between predicted 10-year risk of coronary heart disease and recent use of didanosine (p=0⋅36 for test of interaction between moderate/high risk and recent use of drug). However, there was a significant interaction between the predicted 10-year risk of coronary heart disease and recent use of abacavir (p=0⋅04 for test of interation between moderate/high risk and recent use of drug). In relative terms, the effect of recent use of abacavir was stronger in those with lower underlying risk of coronary heart disease, although the absolute difference was greater in those at higher risk of coronary heart disease.
Figure 2 shows the association with recent use of each drug before and after adjustment for the latest CD4 cell count, viral load, lipid and glucose measurements, blood pressure, and the presence or absence of diabetes and lipodystrophy. Adjustment for these measurements had little effect on either estimate. Further adjustment for the actual use of lipid-lowering or anti-hypertensive medication did not modify our estimates.
Recent use of didanosine and abacavir was associated with the composite endpoint of myocardial infarction, cardiovascular death, or invasive cardiovascular procedure; by contrast, there was no association between cumulative exposure to didanosine and abacavir and this endpoint after adjustment for recent use of the drugs (table 4). No association was found between exposure to either drug (either cumulative or recent use) and stroke, although confidence intervals were wider because of the smaller number of patients with this endpoint (table 4).
Discussion
On the basis of evidence linking the use of stavudine and zidovudine to the development of dyslipidaemia and insulin resistance, we analysed data from a large cohort of HIV-infected patients to determine whether there is an association between the use of these drugs and risk of myocardial infarction. However, by contrast with our expectations, we found that neither drug was associated with an excess rate of myocardial infarction, whereas an association was seen with abacavir and, to a lesser extent, didanosine. Although these two drugs are from the same class, neither are thymidine analogues like stavudine and zidovudine. This finding was unexpected because neither drug is thought to have substantial effects on metabolic factors 15, 16, 26, 27and we could find only one preliminary data-mining analysis of databases of reported spontaneous adverse events that might have suggested these findings.28The increased rate of myocardial infarction in those exposed to abacavir and didanosine was evident while patients were actually receiving the drugs as well as shortly after stopping them, but seemed to decrease within a few months after their cessation.
The D:A:D study is an observational study and, as such, is not designed to definitively establish whether any associations are causal. Thus, we did various analyses to ensure the consistency and robustness of our findings. Since patients with a higher underlying risk of cardiovascular disease might be initially placed on abacavir (a fact that was confirmed in our analyses), we explored whether our findings could be explained by such channelling bias. Although this possibility cannot be excluded definitively, several of our findings argue against this. First, although patients receiving abacavir and didanosine generally had a poorer cardiovascular risk factor profile than did those receiving other NRTIs, our main analyses adjusted for key cardiovascular risk factors (sex, age, body-mass index, smoking status, personal and family history of cardiovascular disease); further adjustment for current lipid measurements, blood pressure, diabetes, and predicted 10-year risk of coronary heart disease resulted in only minor changes to the relative rates. Although alternative analytical methods could be used to account for the potential confounding effects of these factors (eg, propensity scores, marginal structural models), relative rates changed only slightly when adjusting for the latest recorded values of all available potential predictors of treatment choice and of risk of myocardial infarction, so use of these methods would be unlikely to change our conclusions. Second, our analyses revealed that the rate of myocardial infarction remained high as long as patients were receiving these drugs, but then decreased after their cessation. Had the drugs merely served as surrogates for a high underlying cardiovascular risk, we would have expected that this increase in rate would remain after discontinuation of the drugs. Finally, the effect was specific for myocardial infarction and other outcomes related to coronary heart disease but not for stroke, which shares many risk factors with myocardial infarction and might, to some extent, be expected to be affected by the same bias.
Patients participating in D:A:D have also received other drugs as part of their nucleoside/nucleotide backbone, including emtricitabine and tenofovir. There is currently insufficient follow-up time (<2 years on average) among patients receiving these drugs to assess reliable associations with the rate of myocardial infarction.
Although the optimum study design to illustrate a causal relation between myocardial infarction and the use of abacavir or didanosine would be a randomised controlled trial, such a trial would require an extremely large sample size (at least 5000 patients per arm followed for 2 years) and is unlikely to be feasible. Possible pathogenic mechanisms by which abacavir and didanosine affect the risk of coronary heart disease are, as yet, unknown. The increased rate of myocardial infarction associated with recent exposure to abacavir and didanosine in our study did not seem to be mediated through changes in metabolic risk factors. Rather, our finding that the effect could be reversed on cessation of the drug supports a more rapidly acting underlying mechanism, which could involve vascular inflammation. Studies investigating an inflammatory role of abacavir are currently underway and could provide further insight. Moreover, abacavir has been shown to induce cardiomyopathy in mice and rats.29The drug is metabolised intracellularly to carbovir, which has the potential to be cytotoxic.30 Further exploration of these conditions in patients exposed to abacavir could also be worthy of consideration. However, although biological plausibility strengthens the likelihood that an association identified in an observational study is causal, 31 the lack of such a mechanism should not lead to the conclusion that a causal link might not exist. In the last few years, a variety of drugs32, 33, 34, 35 have been shown in randomised controlled trials to increase the risk of cardiovascular disease despite the underlying biological mechanism being unclear.
Abacavir is at present frequently used as part of antiretroviral therapy regimens, while didanosine is used to a lesser extent. Our findings pose a clinical dilemma: should clinicians simply increase their vigilance of possible risk of myocardial infarction without making changes to abacavir or didanosine use while waiting for further evidence to accrue, or should all or some patients who are receiving these drugs be advised to consider discontinuing their use? Although a randomised trial is unlikely to be feasible in the near future, supportive data could become available from other observational studies and biomarker studies. If the decision is made to consider discontinuation of either drug, then a full assessment of the possible risks and benefits of their continued use should be undertaken. Such an assessment must be individualised for each patient and should take into account their underlying risk of myocardial infarction, the availability of other treatment options after taking into account their history of past treatment and HIV resistance testing, and the safety profile of alternative HIV medication. 12, 35, 36, 37, 38 All other NRTIs have the potential for long-term toxicity including metabolic, haematotoxic, renal, or bone-related adverse effects. 36, 37, 38, 39
Our findings of a possible interaction between recent abacavir use and predicted risk of coronary heart disease should be interpreted cautiously given the marginal significance of the findings. However, the relative excess risk of myocardial infarction associated with the use of abacavir tended to be lower in those at moderate or high underlying risk of coronary heart disease than in those at low risk of such disease, although the absolute effect of the increased risk associated with ongoing use of abacavir will be most apparent in those at moderate or high risk. No such interaction was detected for recent use of didanosine. One should note that previous analyses from the D:A:D study have reported that, although the Framingham equation tends to slightly underestimate the risk of coronary heart disease in HIV-infected individuals, it remains a good predictor of such risk in this population.40, 41
Furthermore, among those at low predicted risk of coronary heart disease, rates of myocardial infarction remained low, even in those who had recent exposure to either drug.
The strengths of the present analyses are the large size of the cohort, its long-term follow-up, and the prospective nature of the study which allows for ongoing control of the quality and ascertainment of outcomes. Availability of accurate data for the use of antiretrovirals, as well as those for demographic, HIV-related, and metabolic variables allowed us to control for various factors. Conversely, we do not have complete data for all cardiovascular risk factors at all timepoints and cannot rule out the possibility that this could bias our estimates. However, even in the subgroup of patients with sufficient data to calculate predicted risk of coronary heart disease, recent use of abacavir or didanosine remained associated with a higher observed rate of myocardial infarction, suggesting that our findings are unlikely to be a consequence of missing data. Although we studied the effects of several drugs in our analyses, we did not adjust any p values for multiplicity; the small p values obtained in our analyses for the associations with recent abacavir use would suggest that the results are unlikely to be a consequence of testing errors. By contrast, we have a weaker belief in the association with recent didanosine use given the larger p values seen for these findings. Lastly, although an association was noted in one model between recent exposure to lamivudine and the development of myocardial infarction, this only became apparent after adjustment for past use of the drug. Thus, although we cannot rule out the possibility that this is also a real association, we believe that it is more likely to be a type I error.
The complex treatment patterns necessary to treat HIV infection do not always lend themselves to statistical analysis, and several simplifying assumptions have been made for our analyses. For example, when patients stop a drug in their regimen their exposure to that drug is fixed at the time of stopping and does not change until such point that they restart the drug (if this occurs), at which time exposure continues to accrue. Furthermore, rather than focusing on drug combinations (of which there are a great number of possible options) we have generally considered exposure to each NRTI, PI, and NNRTI individually. Ongoing work in this large cohort collaboration will enable us to investigate the value of alternative analytical approaches.
Once antiretroviral therapy is initiated, it is best used continuously and for life. 42 Our findings emphasise the need to continue to explore the long-term consequences-both beneficial and harmful-of exposure to antiretroviral drugs. At present, most available data are from 48-week randomised controlled trials designed to assess how various components of antiretroviral therapy regimens affect surrogate laboratory endpoints of effectiveness (CD4 cell count and viral load) and safety (lipid and glucose measurements, etc). Our findings serve as a reminder that, ultimately, only studies powered to assess the risk of clinically relevant complications can exclude possible harm reliably.
|
|
| |
| |
|
|
|