| |
The Aging HIV Brain - HIV Accelerates Brain Aging by 3 to 15 Years in Various Studies over the Past 9 years
|
| |
| |
from Jules: its clear to me the problem of brain impairment & function and the affects of aging among HIV+ is a real problem yet this issue appears to be relegated to the dust heap. Why because federal research leaders at HHS, NIAID and OAR have deprioritized this, they have decided this is not as important. When HIV+ reach around 65 the full impact can begin, where HIV+ experience a double hit: the normal affects of aging with HIV with declining immunity and then the affects of HIV on declining immunity. Yes we living with HIV who are older can tell you this is a real problem affecting quality of life and causing impaired mental & physical functioning which causes increased risk for falls and this fractures, added stress and consequent increased heart disease & stroke risk, and much more. Cognitive impairment has a broad affects and is associated with affects on physical functioning like gait, walking capacity, muscle coordination and muscle weakness, and impaired ability to perform daily normal independent activities functioning like household chores and shopping and impaired ability to monitor and understand your healthcare and the comorbidities one has and the ability to interact with care providers. when HIV+
The question of whether HIV+ experience accelerated brain aging has been debated over the past few years with numerous studies published and reported at CROI particularly there were several reported at CROI 2017, notably the COBRA study reported HIV+ did not experience accelerated brain damage. Subsequently several impressive studies were published and also reported at CROI 2017 finding that HIV+ did experience accelerated brain aging. Over the past recent years accelerated aging of the brain in HIV+ has been estimated to range from as little 3 years compared to HIV-neg and as great as 15 years accelerated aging. One study just below found aging in general to be 8 years accelerated in HIV+ vs HIV0neg. The most recent impressive convincing studies that brain aging in HIV+ is accelerated include the one immediately below "Accelerated and Premature...." and the study reported by Goodkin from the MACS group. The main exception is the COBRA grip reporting at CROI 2017 that brain aging in HIV is not accelerated. It is complicated to study and evaluate aging & acceleration of aging in the HIV brain because aging of the brain is not linear, it may vary over the years with no progression for several years and then perhaps acceleration during several years particular ly after around the age of 65 where the double hit of aging in general with its depleted immunity and the affects of HIV on the older aging person where at 65 the combined affects may result in a more severe and accelerated decline in brain function. So looking over a brief period of 5 years may not find acceleration. It also greatly depends on the patient population. There are many confounders including comorbidities, history or current use of substance abuse, and what kinds of drugs were abused. Which is why the Goodkin study is impressive because they controlled as best as possible for most of these confounders in the MACS group. Just this week a study published in JAIDS by Leah Rubin et al reported greater use among HIV+ women in WIHS of drugs that may affect cognitive function: "In conclusion, HIV+ women seem to take a greater number of non-ARV NC-AE medications as well as non-ARVs with anticholinergic properties as well as anxiolytics and anticonvulsants compared with HIV− women." The study found: "HIV+ women may have increased cognitive vulnerabilities to anticholinergic medications. Potential synergy between anticholinergic medications and HIV may explain some HIV-related cognitive impairments. It may be important clinically to consider anticholinergic medication use in HIV+ women." For me this raises several questions: (1) how prevalent is the use of these types or other types of non ARV drugs among HIV+ that can heighten the risk for cognitive impairment, I don't think we have much data beyond this study nor in men, I don't know of such data; (2) are we overusing the types of drugs Rubin examined in her WIHS study; (3) do HIV clinicians and psychiatrics prescribing these drugs have awareness about the risks & dangers of using these drugs in HIV+ and aging HIV? In my report of this study I included information that: Anticholinergic drugs should be avoided in patients with dementia, cognitive impairment, or delirium....It was found the most common anticholinergic drug classes used by the elderly in the study were tricyclic antidepressants, first generation antihistamines and overactive bladder antimuscarinics. Overall, a higher cumulative use of anticholinergic medications (3 years or more) across all subclasses was linked with a 54% higher risk for developing dementia than taking the same dose for three months or less. Results also suggested that the risk for dementia with anticholinergics remain even after drug discontinuation.....some antihistamines, antidepressants, or even muscle relaxants have anticholinergic properties....current use of drugs with anticholinergic properties was significantly associated with low cognitive performance among community-dwelling elderly people"
------------------------------
HIV Accelerates Brain Aging by 3 to 15 Years in Various Studies over the Past 9 years
Accelerated and Premature Aging Characterizing Regional Cortical Volume Loss in Human Immunodeficiency Virus Infection: Contributions From Alcohol, Substance Use, and Hepatitis C Coinfection - (08/15/18) .....The HIV-infected cohort exhibited steeper declining volume trajectories than control subjects, consistently in the frontal cortex. Nonaccelerated volume deficits occurred in the temporal, parietal, insular, and cingulate regions of all three diagnostic groups. Alcohol and drug dependence comorbidities and HCV coinfection exacerbated HIV-related volume deficits. Accelerated age interactions in frontal and posterior parietal volumes endured in HIV-infected individuals free of alcohol or substance dependence and HCV infection comorbidities. Functionally, poorer HIV-associated neurocognitive disorder scores and Veterans Aging Cohort Study indices correlated with smaller regional brain volumes in the HIV-infected individuals without alcohol dependence and alcohol-dependent groups. Conclusions: HIV infection itself may confer a heightened risk of accelerated brain aging, potentially exacerbated by HCV coinfection and substance dependency. Confirmation would require a prospective study with a preinfection baseline.
"Critically, significant HIV-age interactions in lobar and selective frontal and posterior parietal volumes endured in the subset of HIV-infected individuals free of substance dependence or HCV infection compared with control subjects, thereby supporting the premise that HIV infection itself confers a heightened risk of accelerated aging of the brain, notably in the frontal lobes".
HIV Infection and Aging Independently Affect Brain Function as Measured by Functional Magnetic Resonance Imaging - BRIEF REPORT - (01/25/09) Functional brain demands in HIV-positive subjects were equivalent to those of HIV-negative subjects who were 15-20 years older.....HIV infection was equivalent to a 21-year increase in brain age, compared with HIV-negative control subjects. This same group 8 years later from Wash U Ances et all reported this just below declaring HIV brain damage aging was not accelerated.
CROI: LONGITUDINAL ASSESSMENT OF REGIONALLY SPECIFIC BRAIN VOLUMES IN TREATED HIV+ PATIENTS - (02/24/17).
CROI: Cognitive Trajectories in Suppressed HIV Infection Indicate Evolving Disease Activity - (02/24/17).
BIOMARKERS OF AGEING IN HIV-POSITIVE INDIVIDUALS AND MATCHED CONTROLS: 8 years greater biologic age in HIV+ - (02/24/17)
Goodkin is his study published in 2017 controlled for comorbidities and diabetes: Goodkin MACS Study - HIV prematurely ages the brain - new study & Commentary - (07/19/17)....."In an Article in The Lancet HIV,1 Karl Goodkin and colleagues answer the controversial question of whether chronic HIV infection leads to premature ageing in the combination antiretroviral therapy (ART) era: it does." Commentary by Bruce Brew & Lucette Cysique
"Older age was significantly associated with lower performance in all five neuropsychological domains tested (working memory, episodic memory, motor function, executive function, and information processing speed; p<0⋅0001 for all comparisons)...... results should spur the development of geriatric medicine into an integrated multidisciplinary model of care for ageing patients with HIV.....large studies are needed to address whether ageing people with HIV are at increased risk of age-associated neurodegenerative disorders, such as vascular cognitive impairment6, 7 and perhaps Alzheimer's disease.....results support the general clinical need to screen HIV-infected individuals for HIV-associated neurocognitive disorders and to do so particularly intensively for older HIV-infected individuals, ideally with tests sensitive to deficits in the episodic memory and motor domains"......Our study also adds to the methodological rigour of published work through its controls for medical and psychiatric comorbidities and other factors that can affect cognition. we applied additional exclusion criteria: history of CNS opportunistic infections or tumours; treatment with chemotherapy; major psychiatric disorder (eg, psychosis); history of or current non-HIV-associated neurological disease; current severe alcohol or substance-use disorder; collagen vascular disease; thyroid disease; chronic obstructive pulmonary disease; emphysema; congestive heart failure; angina pectoris; myocardial infarction within the previous 6 months; hepatic failure; renal failure; daily use of systemic steroids (catabolic or anabolic), narcotic or opioid analgesics, or immunostimulant or immunosuppressive drugs; and participation in blinded trials of antiretrovirals that were not approved by the US Food and Drug Administration. Individuals with a history of intravenous drug use were few and were not excluded.......We used control variables to optimise control for extraneous sources of variance in neuropsychological outcomes. Educational level10 ......Other control variables were time since seroconversion (months at each visit [in a subsample analysis] by actual date of seroconversion [or date of study entry as a proxy]; HIV-seronegative participants were coded as 0), ART era (before and after Jan 1, 1996, which was defined as the beginning of the era of effective ART), medical comorbidities (diabetes diagnosis,12 ......hypertension diagnosis,..... history of exposure to hepatitis14 B virus [metabolic effects] or C virus [metabolic effects and direct CNS effects], .....global nutritional status15 (relative change in total bodyweight from the previous visit and body-mass index [BMI], which were obtained by weighing participants: underweight [<18·5], average [18·5–24·9], overweight [25·0–29·9], and obese [>30·0]), depressed mood level (per the Centers for Epidemiology-Depression [CES-D] Scale16), fatigue level17 .....pain18 (self-report by number of types present [head, joint, abdominal, muscle, or urinary]—0=0–1 types, 1=2–3 types, and 2=4–5 types present). Alcohol and psychoactive substances requiring control were reduced to self-report of alcohol use19 ...... cigarette smoking20 (MACS-derived algorithm generating total pack-years), and frequency of use (none vs any) of cannabis21 and nitrite inhalants (ie, poppers).22 Psychotropic drug use23 was controlled by use at assessment derived from self-report based on relevant drugs listed across psychotropic categories. HIV-specific control variables (eg, CD4 cell count nadir, plasma HIV load, antiretroviral adherence, and CNS-penetration scores) were not used because these variables cannot be properly defined for HIV-seronegative participants. Insufficient data were available to allow us to control for cholesterol and triglyceride concentrations, renal and hepatic function, and laboratory measures of general nutritional status.
Progressive Brain Atrophy Despite Persistent Viral Suppression in HIV Over Age 60 - (07/19/17) "In summary, we find that long-term virally suppressed HIV-infected individuals have brain atrophy rates that exceed that expected from healthy controls. These results inform a potential gap in neuroprotection despite adherence to cART with long-term maximal viral suppression in plasma."....In longitudinal ROI models adjusted for age and sex, we uncovered progressive atrophy in the HIV-infected group exceeding rates seen among healthy controls (Table 2, bottom panel) with faster annualized rates of progressive atrophy in the cerebellum (0.42% vs 0.02%, p=0.016), caudate (0.74% vs 0.03%, p=0.012), frontal lobe (0.48% vs 0.01%, p=0.034), total cortical gray matter (0.65% vs 0.16%, p=0.027), brainstem (0.31% vs 0.01%, p=0.026), and pallidum (0.73% vs 0.39%, p=0.046) (Figure 1)......We add to a growing number of studies identifying detrimental neuropathogenic pathways, typically associated with persistent inflammation.
IMPACT OF ADVANCING AGE ON COGNITION IN HIV+ PERSONS ON A FIRST SUPPRESSIVE REGIMEN - (02/24/17)
Cognitive trajectories over 4 years among HIV-infected women with optimal viral suppression: HIV+ virally suppressed had worse cognitive decline in 3 domains vs HIV-neg, 4 yrs followup - (02/24/17)
COBRA - LONGITUDINAL ANALYSIS SHOWS NO EVIDENCE FOR ACCELERATED BRAIN AGEING IN TREATED HIV - (02/24/17)
HIV Infection May Make the Brain 15 to 20 Years Older: HIV slows cerebral blood flow and stimulus response in MRI study - - (02/23/09)
"Baseline cerebral blood flow declined significantly with age in both the HIV group and controls (P < 0.001) and was significantly lower in the HIV-infected people at every age (P < 0.001).......There is about a 15-year brain aging because of HIV-infection"..... Ances speculated that HIV-induced decreases in endothelial function or platelet function could lead to decreases in cerebral blood flow......"How do we link this all together and how is this creating a strain on the brain. HIV and aging both have a lot of similar parallels for naïve and memory T-cell function, replicative sinesence as all as even increased cytokine production, so they could have parallel streams that could be developing. So when we have a younger HIV+ individual (represented in slide below) they have aging that is present and they may have co-morbidities present, as well HIV being present contributes to stress on the brain. As they get older the comorbidities present as well as aging may put a strain on the brain on top of HIV".
Frailty Stronger Than Neurocognitive Impairment in Predicting Falls-Disability-Death - - (02/26/17)
Neurologic Complications of HIV Disease and Their Treatment - written by Scott L. Letendre, M.D. et al for NATAP CROI coverage - (03/19/09)
Neurocognitive (and neuropathy) Impairment Rate Remains High in Diverse US Cohort - written by Mark Mascolini - (02/18/09)
Neurocognitive Disorders Threaten HIV+ - (02/20/09)
High Prevalence (24%) of Mild Neurocognitive Disorders in HIV-infected Patients, ANRS CO3 Aquitaine Cohort: "For every 4 treated adults with well controlled HIV-infection, 1 had a mild cognitive disorder as compared to 6% in the French general population of 65 years or older".....In multivariate analysis, older age (OR = 1.1 for 1 additional year and a lower nadir of CD4 was significantly associated.....High Frequency (51%) of Neurocognitive Disorders in Older HIV-infected Patients despite a Sustained Virological and Immunological Response on cART: The Sigma Study: Despite a sustained response to cART, neurocognitive disorders are more frequent in old HIV+ patients than in the general aging population, but are underdiagnosed by their physicians. In our patients, subcortical types of cognitive impairment remain more predominant than neocortical types. The respective role of HIV, ART, and co-morbidities is debated. Longitudinal studies are needed to assess the outcome of these disorders in aging and to determine their predictive factors.
Immune Senescence, Activation and Abnormal T cell Homeostasis Despite Effective HAART, A Hallmark of Early Aging in HIV Disease - (03/03/09)
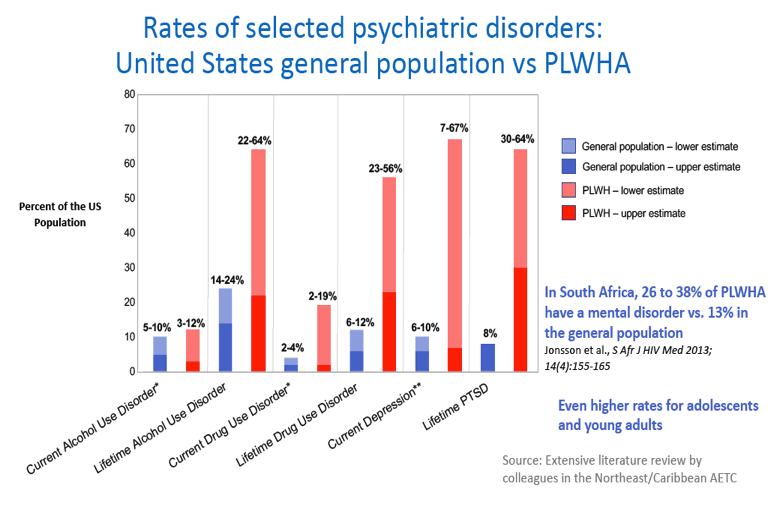
CROI: Mental Disability in HIV- Misunderstood & Unmet Need - (05/15/18)
|
|
| |
| |
|
|
|