 |
 |
 |
| |
Increasing trends in multimorbidity and polypharmacy over a
5-year period in people living with HIV in the United States
- Big US Study Confirms Ballooning Multimorbidity, Polypharmacy With HIV
|
| |
| |
"The combined presence of HIV, aging, and ART has been shown to increase risks of comorbid conditions and increase the likelihood of polypharmacy, but recent trends in prevalence of such are not fully understood"
IDWeek: CHARACTERISTICS, COMORBIDITIES, AND MEDICATION BURDEN AMONG PEOPLE LIVING WITH HIV IN THE US MEDICARE PROGRAM - (09/30/21)
the ages in these 2 studies at IDWeek are much younger than the HRSA study in the link just above which is important understanding the prevalence of comorbidities & polypharmacy because with older groups on Medicare or Medicaid you will see higher rates compared to HIV-negatives. As PWH age their slope of decline in function & slope of increase in comorbidities & polypharmacy is worse compared to HIV-negatives, this worsening slope begins often around 55 but steepens with age often. Jules Levin
IDWeek, September 29-October 3, 2021
Mark Mascolini
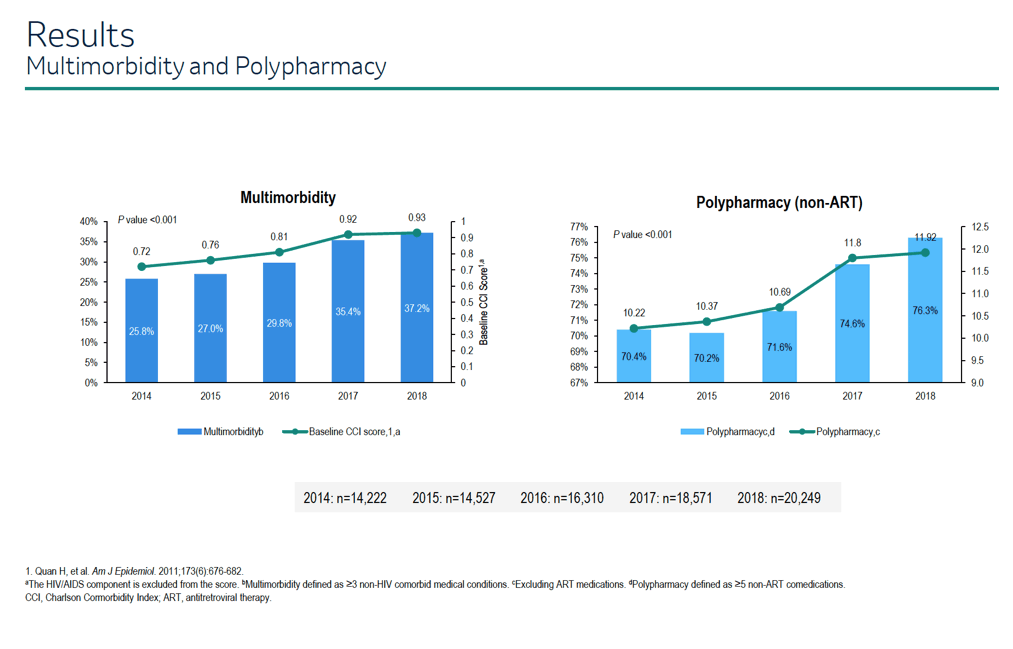
Multimorbidity prevalence rose from 25.8% in 2014 to 37.2% in 2018 in an analysis of 83,879 insurance claims from HIV-positive people using commercial insurance or Medicare in the United States [1]. Prevalence of polypharmacy (taking 5 or more nonantiretroviral drugs) climbed from 70.4% to 76.3% over the same period. Cardiovascular and neuropsychiatric conditions (and medications) were the most frequently reported in this insurance claims database of people with HIV.
As people with HIV live longer thanks to antiretroviral therapy (ART), they acquire age-related diseases, sometimes at a faster pace or in a more advanced form than their HIV-negative contemporaries. These comorbidities often require additional medications, which carry their own risks and further complicate care of people with HIV.
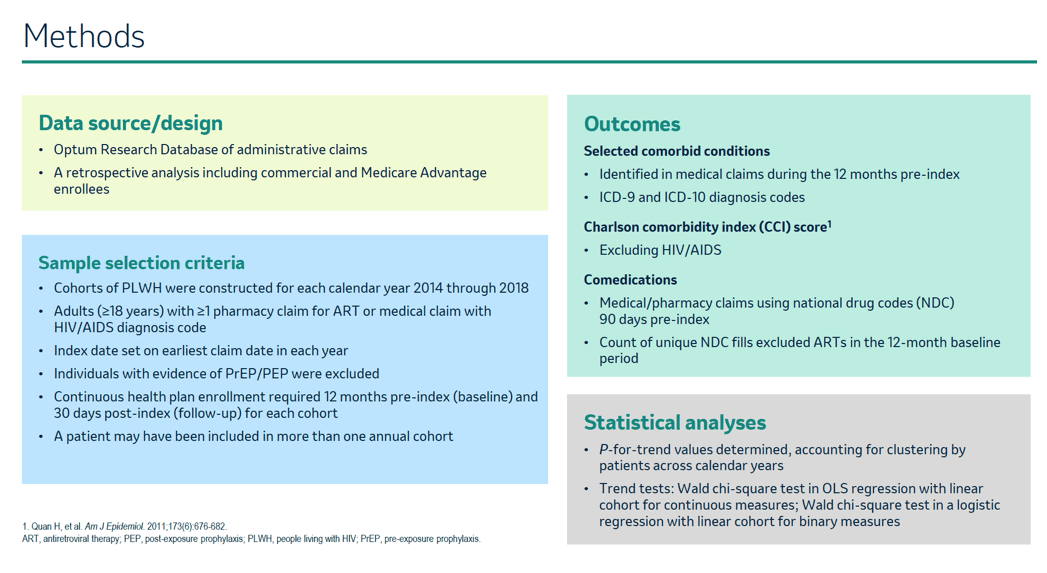
Several clinic- and cohort-based studies have tracked trends in multimorbidity and polypharmacy in HIV-positive people, sometimes comparing findings with HIV-negative comparison groups. To get a broader look at these issues over a longer time, US academic researchers and colleagues working for the Optum Research Database [2] and the pharmaceutical industry retrospectively analyzed pharmacy claims and clinical data of commercial and Medicare Advantage Optum enrollees. The investigators created a cohort for each of 5 study years, 2014 through 2018, including adults who made 1 or more pharmacy claims for ART or medical claims with HIV/AIDS diagnosis codes.
For the multimorbidity and polypharmacy analyses, numbers of people in each annual cohort were 14,222 in 2014, 14,527 in 2015, 16,310 in 2016, 18,574 in 2017, and 20,249 in 2018, totaling 83,879 individual claims.
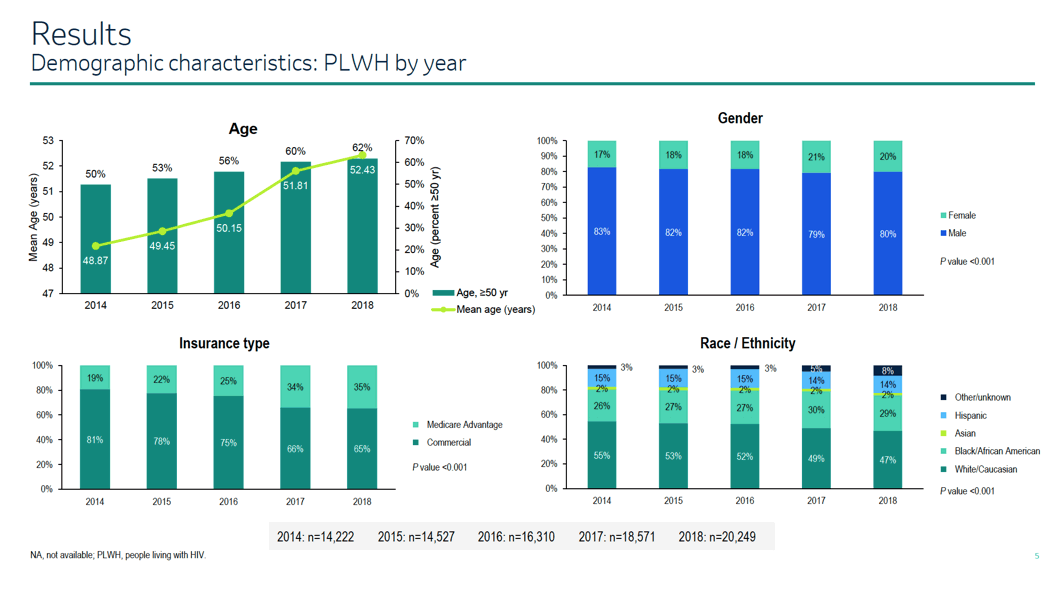
Average age of the 5 yearly cohorts climbed each year from 48.9 years in 2014, to 49.5 in 2015, to 50.2 in 2016, to 51.8 in 2017, and to 52.4 in 2018 (P < 0.001). Proportions of people 50 or older in those 5 years were 50%, 53%, 56%, 60%, and 62%. The proportion of women also inched up across the 5 study years: 17%, 18%, 18%, 21%, and 20% (P< 0.001). Across the same years, the proportion of people using Medicare (public insurance for people 65 or older) rose from 19% to 22% to 25% to 34% to 35% (P < 0.001). The proportion of whites fell from 55% in 2014 to 47% in 2018, while the proportion of blacks edged up from 26% to 29% (P < 0.001).
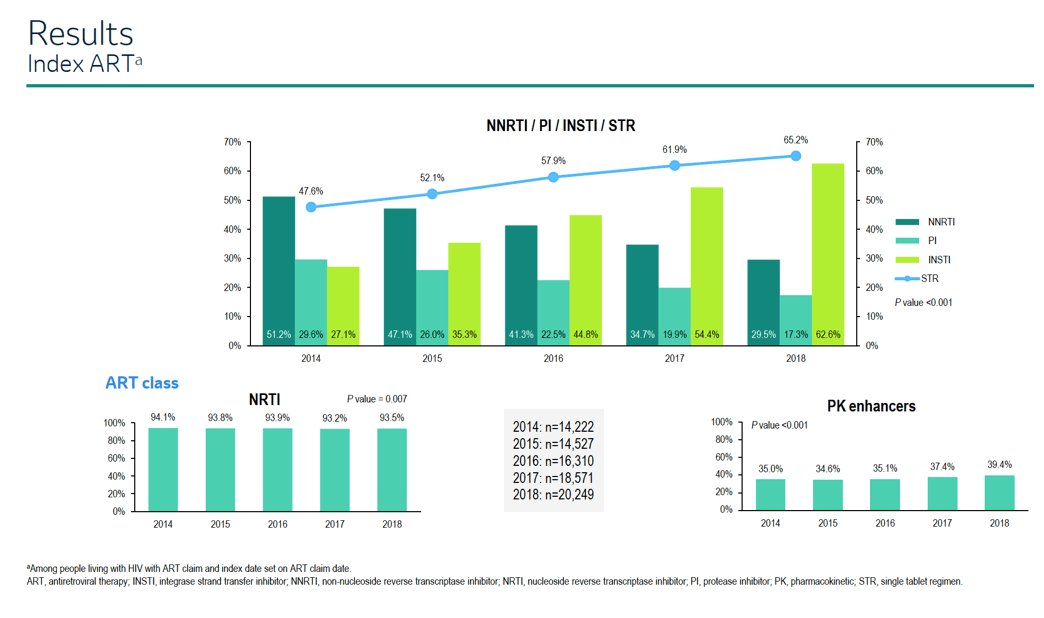
Proportions of people taking a nonnucleoside-based combination plunged from 51.2% in 2014 to 29.5% in 2018, as did the proportion taking a protease inhibitor combination, from 29.6% to 17.3%. These declines were balanced by a steady crescendo in proportions taking an integrase inhibitor regimens, from 27.1% in 2014 to 62.6% in 2018. Use of single-tablet regimens clambered from 47.6% in 2014 to 65.2% in 2018. (For all these changes, P < 0.01.)
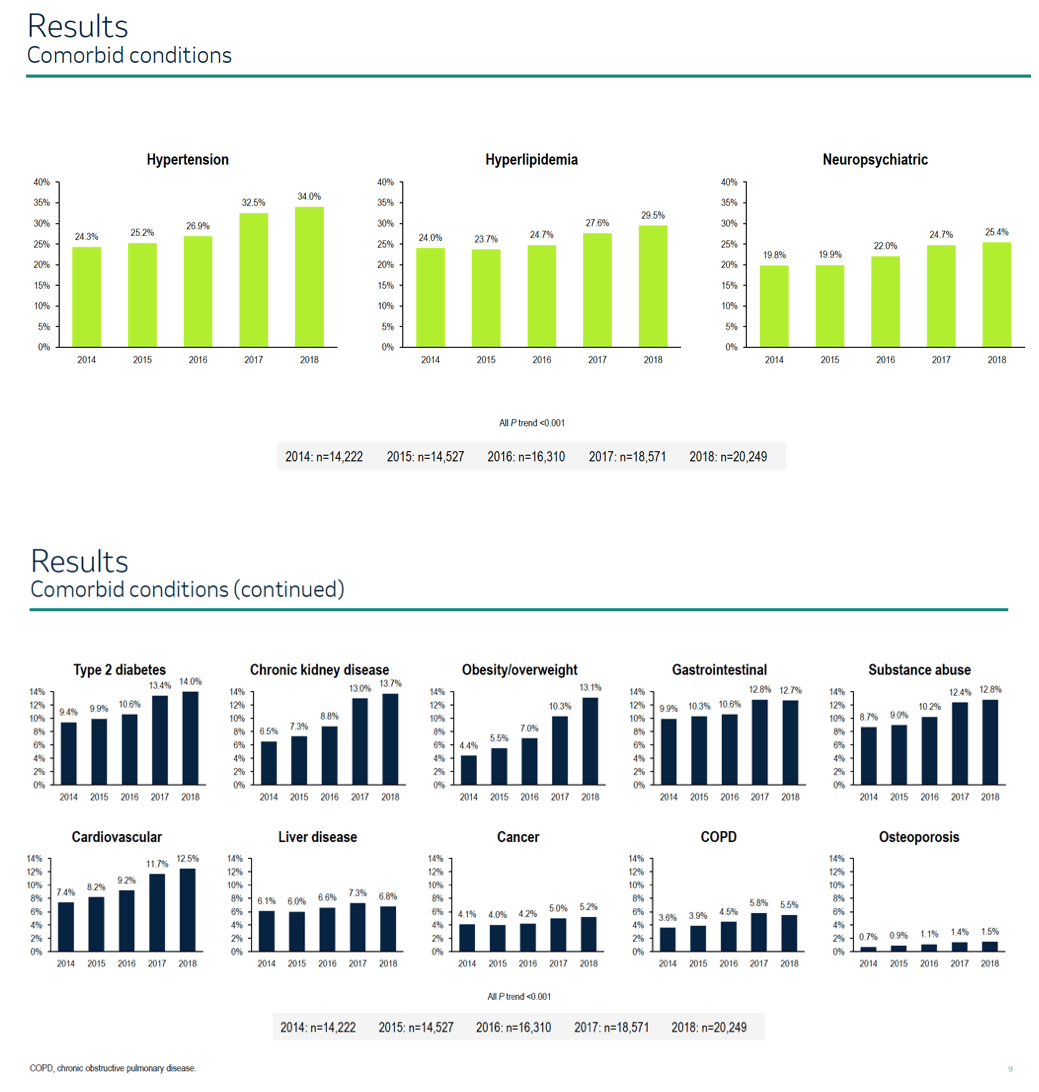
Proportions of cohort members with multimorbidity, defined as having 2 or more non-HIV conditions, rose steadily across the 5 study years: 25.8% in 2014, 27.0% in 2015, 29.8% in 2016, 35.4% in 2017, and 37.2% in 2018 (P < 0.001). Proportions using polypharmacy, defined as 5 or more non-ART medications, ascended from 70.4% and 70.2% in 2014 and 2015, to 71.6% in 2016, to 74.6% in 2017, and to 76.3% in 2018 (P < 0.001).
The most frequently recorded comorbidities were cardiometabolic (hypertension 24.3% in 2014 to 34.0% in 2018; hyperlipidemia 24.0% to 29.5%) and neuropsychiatric (19.8% in 2014 to 25.4% in 2018). Proportions of people with other reported conditions in 2014 and 2018 were type 2 diabetes (9.4% to 14.0%), chronic kidney disease (6.5% to 13.7%), obesity/overweight (4.4% to 13.1%), gastrointestinal conditions (9.9% to 12.7%), substance abuse (8.7% to 12.8%),
cardiovascular disease (7.4% to 12.5%), liver disease (6.1% to 6.8%), cancer (4.1% to 5.2%), chronic obstructive pulmonary disease (3.6% to 5.5%), and osteoporosis (0.7% to 1.5%) (all P < 0.001).
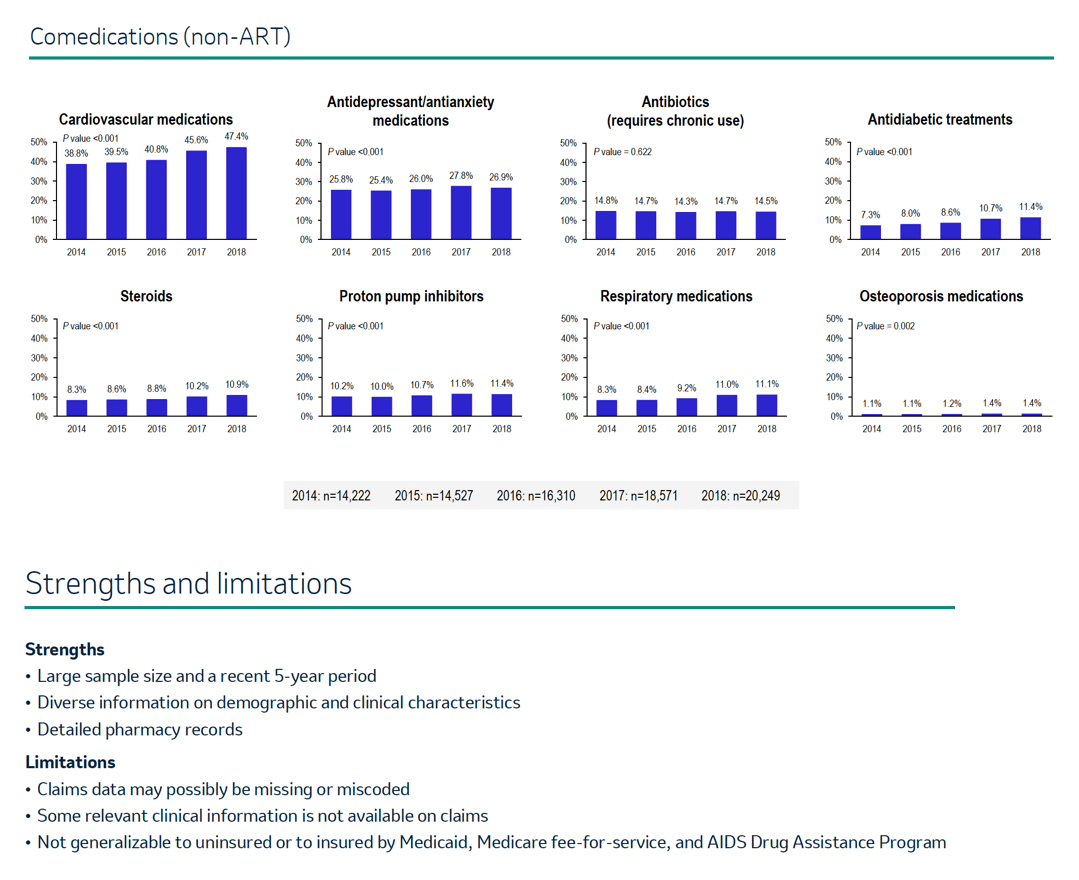
Prescription claims mirrored these trends. The most used agents were cardiovascular medications (from 38.8% in 2014 to 47.4% in 2018, P < 0.001) and antidepressant/antianxiety drugs (from 25.8% in 2014 to 26.9% in 2018, P < 0.001). Chronic antibiotics held third place in frequency but did not rise over the years (14.8% in 2014 and 14.5% in 2018). Prescription frequency of several other classes did rise significantly from 2014 to 2018: antidiabetics (7.3% to 11.4%, P < 0.001), steroids (8.3% to 10.9%, P < 0.001), proton pump inhibitors (10.2% to 11.4%, P < 0.001), respiratory medications (8.3% to 11.1%, P < 0.001), and osteoporosis medications (1.1% to 1.4%, P = 0.002).
The researchers concluded that multimorbidity and polypharmacy rose among people with HIV in recent years. They urged clinicians "to consider the comorbidity profile in HIV management, including selection of appropriate ART to improve patient health by avoiding drug-disease and drug-drug interactions."
In a recent review, HIV clinicians and researchers Todd Brown (Johns Hopkins University) and Giovanni Guaraldi (University of Modena and Reggio Emilia) summarized recent findings on multimorbidity and polypharmacy in people with HIV [3]. Exploring epidemiology, risk factors, causes, and potential consequences of multimorbidity in aging HIV populations, they argued that "with aggressive risk factor management for comorbidities and less toxic antiretroviral medications, the burden of multimorbidity in HIV-infected persons can be reduced" [3].
References
1. Paudel M, Prajapati G, Buysman EK, et al. Increasing trends in multimorbidity and polypharmacy over a 5-year period in people living with HIV in the United States. IDWeek, September 29-October 3, 2021. Abstract 71.
2. Optum Claims Data.
https://www.optum.com/business/solutions/life-sciences/real-world-data/claims-data.html
3. Brown TT, Guaraldi G. Multimorbidity and burden of disease. Interdiscip Top Gerontol Geriatr. 2017;42:59-73. doi: 10.1159/000448544. https://www.karger.com/Article/Abstract/448544



|
| |
|
 |
 |
|
|