| |
Aging in US - Worse Still To Come - polypharmacy, multiple comorbidities,
decreased survival, impaired daily activities functioning
|
| |
| |
Jules Levin, NATAP
- 75% of HIV+ are over 40 years old in NY, SF, Massachusetts & Florida
- 53% are over 50 years old
- 20% over 60
Decreased Survival in HIV+ [http://www.natap.org/2016/HIV/020816_05.htm ]
- we already have Increased Comorbidities & Poly-Pharmacy in HIV+ but we will see increases in individuals and the overall patient population now over 50-60.
Aging: Worse To Come....those with HIV and aging have to deal with both...many studies report HIV accelerates aging by 10 years, yet we are not prepared say Drs Seigler & Singh directors at the NY Cornel Aging Clinic
Italy researchers observe 50% with HIV are over 50 in 2016, which will approach 70%by 2020 and over 75% by 2025: "In 15 years time the HIV geriatric population [65-67 yo] will increase from 4% to 37%"...."In 15 years time the most frail HIV population will increase from 24% [now, 2016] to 48%"....."In 15 years time 34% of PLWH will be disabled" [burden of IADLs - independent activities of daily living] - see graph - appears to predict 30% will experience a fall in 15 years, up from 20% now
Some mistakenly believe HIV survival has been normalized minimizing & underestimating the impact of aging in HIV. CDC reports that in 2013 42% diagnosed with HIV are over 50 years old, 25% over 55, and 6% 65 or older, and 17% were 45-49
[https://www.cdc.gov/hiv/group/age/olderamericans/] The CDC previously projected that by 2015, more than half of all HIV-infected Americans will be over 50 years old
[https://www.nia.nih.gov/newsroom/features/aging-hiv-responding-emerging-challenge] ; soon they will be over 60. In NY & SF almost 80% with HIV are over 40 years old. In NYC 52% were reported by the NYC Dept of health to be over 50, 32% 50-59 & 20% >60, and of note 24% are 40-49. Among women with HIV in NYC [https://www1.nyc.gov/assets/doh/downloads/pdf/dires/hiv-surveillance-annualreport-2015.pdf] In San Francisco 60% of those living with HIV are over 50 years old, 19% 60-69, and 25% are 40-49, reported by the San Francisco Department of Public Health 2015 [https://www.sfdph.org/dph/files/reports/RptsHIVAIDS/AnnualReport2015-20160831.pdf]I have collected a selection of more recent studies many presented at conferences in the past few months or published very recently that still only representing a fraction of the many studies on these topics.]......In Boston health officials reported in 2015 59% were over 50 and 21% over 60 and 16% 45-49, thus 75% of all HIV-infected were over 45. http://www.mass.gov/eohhs/docs/dph/aids/2015-profiles/city-boston.pdf
In Florida health officials reported 53% are over 50 with 25% 45-49 and 25% over 60. [http://www.floridahealth.gov/\/diseases-and-conditions/aids/surveillance/epi-profiles/2015/state-1415.pdf]
by 2030 30% will be 60 & older & 23% >65, said Linda fried, MD in her talk on HIV & Aging: a new paradigm at NYS AIDS Institute Conference [https://www.youtube.com/watch?v=9alEsXqT0BU]
a recent Dutch study projected that by 2030, 73% of those infected with HIV will be at least 50 years of age and 39% will be 60 years or older .....http://www.natap.org/2016/HIV/PIIS1473309915000560.pdf
Senate Hearing 2013: Older Americans: The Changing Face of HIV/AIDS in America
.....[ http://www.aging.senate.gov/hearings/older-americans-the-changing-face-of-hiv/aids-in-america]Sen Nelson of Florida said "30% are over 50 now and in 2 years 50% will be over 50, its actually 53% in 2015 with 25% 40-49; the age group with the highest prevalence is bt far over 60 with 25% [http://www.floridahealth.gov/\/diseases-and-conditions/aids/surveillance/epi-profiles/2015/state-1415.pdf].....Sen Collins of maine said HIV+ are experiencing comorbidities a decade sooner.....Sen Warren stated "52% in her state Mass with HIV are >50 yrs old & 15% are 60 or older".
Perhaps the most revealing is the SCOPE San Francisco Cohort. Average age was 57 (54-62) with 15.4% 60-65 and 19.4% over 65 years old, average number of comorbidities was 4 (3-6), and the number of nonantiretroviral medications was 9 (6-12). The most frequent conditions were prefrailty (n = 87, 56.1%), difficulty with 1 or more IADLs (72, 46.5%) [independent activities of daily living], and cognitive impairment (72, 46.5%). Prefrailty was found in 56.1% http://www.natap.org/2015/HIV/052015_04.htm
An Italian aging research group reported at the Aging Workshops this Fall 2016 in NY & Washington DC that 20% are frail now, 75% will be frail in 15 years and 34% will be so frail they will need to be confined in old age homes. Researchers in Washington DC reported at the DC workshop that 50% in a 7,000 patient cohort were not receiving therapy for their cormorbidities and multicomorbidities was highly prevalent. http://www.natap.org/2016/AGE/AGE_02.htm
The cost of aging has received little discussion: "we were able to demonstrate that the total direct cost increases two-fold moving from the <40 years age strata of HIV-infected patients (US$10,588.45) to those older than 60 years (US$21,280.72)".http://www.natap.org/2016/HIV/120816_02.htm http://www.natap.org/2016/AGE/AGE_18.htm
a recent Dutch study projected that by 2030, 73% of those infected with HIV will be at least 50 years of age and 39% will be 60 years or older .....http://www.natap.org/2016/HIV/PIIS1473309915000560.pdf
Increasing Costs with Aging & Comorbidities
- high & increasing frailty rates, doubling & tripling of comorbidity rates [bone, kidney, heart, cancers, cognitive/neurologic, hypertension, diabetes] in US, Spain, Netherlands, Italy, France, increasing cancer rates, increasing rates of falling for women in WIHS & men too: 40% in older SF cohort, 50% in Wash DC nor getting treated for comorbidities: study at Aging Workshop reports from large federal database, older HIV+ experienced greatly reduced capacity to perform normal daily living activities - from a Medicare study go HIV+ : 2 times the number of comorbidities & 4 times for Blacks & Latinos vs HIV-negatives.....Data from 2005 Medicare expenditure costs, indicate that the annual costs for Medicare beneficiaries with one chronic condition are $7,172, and for beneficiaries with three or more chronic conditions $32,498
- AND 46% balance problems, adherence issues, 14% slow gait / walking problems, loneliness, depression, mobility barriers, anxiety, PTSD, food/insurance/housing concerns, stigma, guilt, fear.....Aging, Worse Still to Come?....Aging Clinic at Weill-Cornell, NYC; aging $costs in HIV skyrocket
- Italy study reports that 42% >50 now in Italy & 95% will be over 50 by 2030 with 34% being frail.....http://natap.org/2016/AdverseReactComor/AdverseReactComor_13.htm
CROI: Aging with HIV: Emerging importance of chronic comorbidities in patients over 75
If an HIV+ person lives to 75, this study presented at CROI this year: when comparing patients >75 vs 50-74 years old - doubled hypertension rates, bone disease, CVD rates, cancers, triple renal failure rates & stroke rates & triple the number of patients with 4 or more comorbidities for patients >75 years old compared to patients 50-74 yo, and doubled the rate with 2-3 comorbidities - 1.5% of these patients were over 75 years
.......management of comorbidities should be prioritized (especially cardiovascular, hepatic, renal, bone, central nervous system). Risk for polypharmacy and drug-drug interactions in older HIV adults should be considered......HIV specialists, primary care clinicians, and geriatricians should work together to achieve successful aging for this population
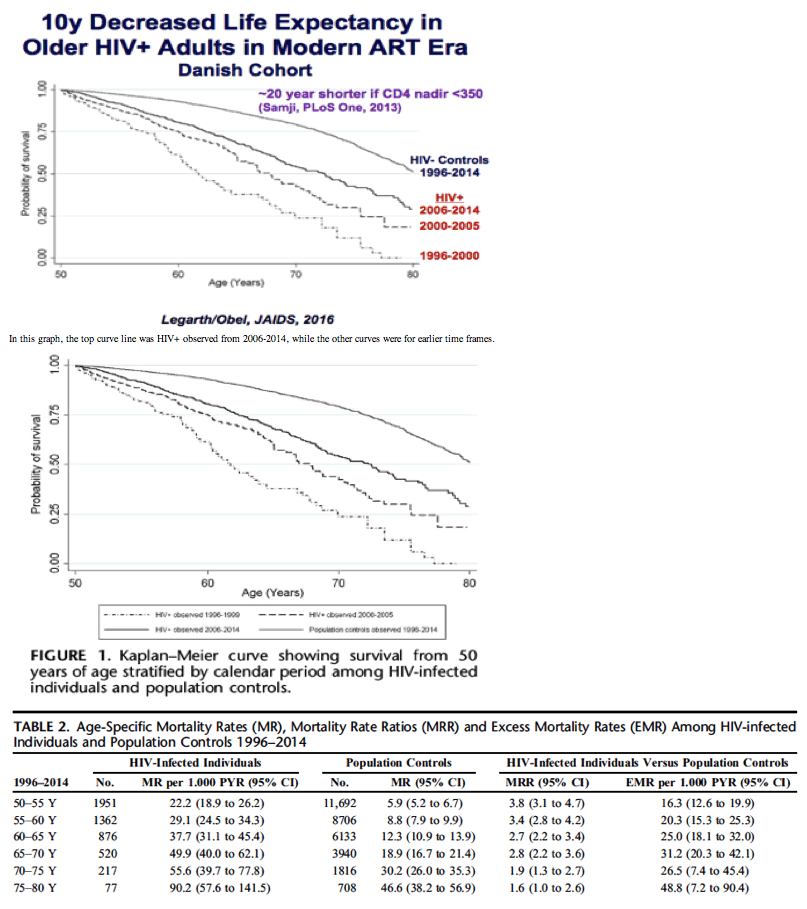
Decreased Life Expectancy in HIV+
1.7 higher mortality risk BUT these were in patients without comorbidities so clearly we can expect mortality will worsen for aging HIV+ with multiple comorbidities..... To our knowledge, this is the first nationwide study to estimate long-term mortality among 50- 80 year old HIVinfected individuals compared with an individually-matched cohort from the background population.....Our aim was to estimate long-term mortality among HIV-infected individuals who were 50 years or older, when compared with an individually-matched cohort from the background population.....We detected a 1.6-fold increased risk of death of among HIV-infected individuals ≥ 50 years without comorbidity compared with population controls without comorbidity....Among HIV-infected individuals without comorbidity the estimated median survival time from age 50 years was 25.6 years (to age 75.6 years) (95% CI: 23.8 to NA) compared with 34.2 years (age 84.2 years) (95% CI: 29.6 to 38.3) among population controls without comorbidity. MRR was 1.7 (95% CI: 1.2 to 2.3) for HIV-infected individuals compared with population controls.
HIV-infected individuals who were observed during 1996-1999 had increased mortality within all age-strata compared with HIV-infected individuals observed during 2006-2014: MRR 1.5 (95% CI: 1.0 to 2.4) for 50-55 years, 1.8 (95% CI: 1.0 to 3.1) for 55-60 years, 2.5 (95% CI: 1.3 to 4.7) for 60-65 years, 1.2 (95% CI: 0.5 to 3.0) for 65-70 years, 1.2 (95% CI: 0.3 to 5.5) for 70-75 years, and 9.5 (95% CI: 1.7 to 53.7) for 75-80 years......and if an HIV+ person squires a comorbidity before getting HIV-infected that increases mortality risk.....http://journals.lww.com/jaids/Fulltext/2011/08010/Comorbidity_Acquired_Before_HIV_Diagnosis_and.14.aspx
In this graph, the top curve line was HIV+ observed from 2006-2014, while the other curves were for earlier time frames.
Frailty in MACS men.....frailty increased with duration of HIV infection.....
Although aging is associated with increased risk of specific diseases, it can also manifest as frailty (15-18), a syndrome that involves enhanced vulnerability to stressors and is thought to be due to dysregulation of multiple physiologic systems (18-20). There is evidence that it predicts loss of independence and death, consistent with geriatricians' observations
.....In a multivariate model including age, ethnicity, and educational level (Table 3, Model 1), HIV-infected men were more likely than were uninfected men to manifest physical shrinking (odds ratio [OR] = 12.80), exhaustion (OR = 3.02), slowness (OR = 3.94), low physical activity level (OR = 3.40), and the aggregate FRP (OR = 10.97)......HIV infection is associated with diverse impairments that resemble frailty, such as myopathy, loss of muscle mass and weight, fatigue, functional impairments, cognitive dysfunctions and motor abnormalities, as well as rheumatological disorders and neuropathies, even in the absence of identifiable opportunistic illnesses
Falls for Women in WIHS.....Longitudinal Study of Falls among HIV-infected and Uninfected Women: Results from the Women's Interagency HIV Study......
average age of women was only around 50, yet - 36% of women experienced a fall, 15% a fall + an injury, & 2% a fall with a fracture; 8-10% had 2 or more falls; cocaine, crack, heroin all increase risk for fall by 50% to 170%, former use increases risk by 50% & current use increases risk by 170%, alcohol use increases risk....also increasing risk for a fall: HCV, subjective cognitive complaints, neuropthy, depression, low kidney function, HCV, hypertension, diabetes & numbers of comorbidities, & CNS active medications
Frailty and the Risk of Falls in HIV-Infected Older Adults in the ACTG A5322 Study.....
average age 51 [46-56] 18% had a fall or more than 1 fall in past 18 months, 7% had recurrent falls, 5.2% got a fracture as a result fall; age breakdown for falls: 25% >60 years old had a fall; 20% 50-59 had a fall; 12% 40-49 had a fall. Falls by frailty status: 49% who were frail had a fall; 21% who were pre-frail had a fall; and, 12% who were not frail had a fall. The study found being frail vs not being frail increases risk for a fall by 2 times but for more than one fail risk increases much more; and once an HIV+ person in this study crosses over pre-frail to frailty that too increases the risk quite a bit.
Up to Half in Older DC Cohort Not Treated for Metabolic Comorbidities - High Burden of Comorbidities in Inner City Washington DC -
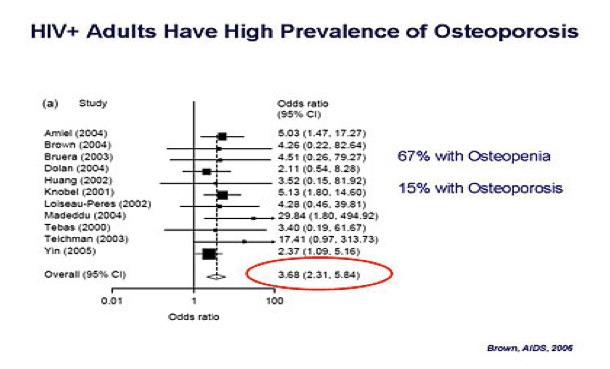
SF - Geriatric Syndromes are Common Among Older HIV-Infected Adults
45% reported difficulty with daily living activities (IADLs) .....more than half of participants had 2 or more geriatric syndromes, which was associated with CD4 nadir....Subjects had a median of 4 (IQR 3-6) co-morbidities and were taking a median of 9 (IQR 5-12) non-antiretroviral medications. 86% of subjects had at least one geriatric syndrome and 54% had 2 or more syndromes
Factors Associated with Limitations in Daily Activity Among Older HIV+ Adults....HIV+ have 2-4 times higher rates of impaired ability to perform daily functioning activities vs HIV-negatives ....HIV+ middle Age & older have 2-3 times higher rates of impaired daily independent living activities vs HIV-negatives.
40% of Aging Experienced a Fall in Past Year in SF, 37% Cognitively Impaired, 34% Severely Lonely, 26% Depressed, Costs of Comorbidities Tripled....Aging Clinics in NY & SF - Non-HIV care provider....Aging, Worse Still to Come?....Aging Clinic at Weill-Cornell, NYC; aging $costs in HIV skyrocket -
Medicare HIV+ beneficiaries Comorbidities Prevalence......
HIV+ >65 on Medicare Have 2 Times More Comorbidities vs HIV-neg AND Blacks & Latinos Have 4-Fold Increased Risk for the 5 Comorbidities Examined vs Whites - CDC Report Chronic health conditions in medicare beneficiaries 65 years and older with HIV infection.
.....were more likely to have 5 chronic conditions (22.11% versus 8.41%).....As greater numbers of PLWHIV enter Medicare as age-eligible beneficiaries, the majority of their care costs will shift from Medicaid to Medicare....Adjusted odds of having HIV infection and one or more comorbidities ranged from aOR 2.38 95% CI (2.21, 2.57) for having one condition to aOR 7.07 95% CI (6.61, 7.56) for having all five chronic conditions (Table 4). ......For male African American and Hispanic beneficiaries with chronic conditions, the likelihood of HIV infection was especially elevated in comparison to that of white female beneficiaries with the same chronic condition, with adjusted odds ratios ranging from 8.99 to 6.33
This is important given that costs for HIV care are considerable, even without the additional costs seen when multiple chronic conditions are also considered. Cost estimates of living with HIV in the U.S. range considerably depending on demographic and HIV related factors; but estimates using 2005 and 2006 data range from $10,000 to $40,000 per year (28, 29). Costs associated with multiple chronic health problems are also high. Data from 2005 Medicare expenditure costs, indicate that the annual costs for Medicare beneficiaries with one chronic condition are $7,172, and for beneficiaries with three or more chronic conditions $32,498 (30 )
EuroSIDA: The proportion of people 50 or older rose from 25.2% in 2006 to 44.0% in 2014 with Doubling & tripling of Some comorbidities
GLASGOW: Mortality rates and excess mortality among HIV-positive persons according to age in Spain, 2004-2014 - (11/08/16)
Glasgow - Spain: "within 4 years from 2010 to 2014 there is a 44% increase in the prevalence of history of CV event. This is concordant with the higher prevalence of diabetes, hypertension, dyslipidemia, and obesity. Diabetes, hypertension and dyslipidima increased between 10% and 45%. For history of renal impairment and fracture, the increase was 24% and 42%, respectively......the proportion of patients on high risk for progression to chronic kidney disease increased 28% (Figure 4)....In 2014, 45% of patients had medium/high risk of coronary heart disease (Figure 5). Of these, 87% also medium/high risk of progressing to chronic kidney disease. Overall, 39% of patients had simultaneously moderate/high risk of chronic kidney disease and chronic heart disease (CHD) Table 3, and approximately two thirds were on TDF or ABC."
Polypharmacy in Chicago Aging: IDSA: [35% Taking 12 Comedications !] - Polypharmacy in HIV+ 50 or Older Linked to Lower CD4s, Higher CVD Rate - Evaluating the Effect of Polypharmacy on Outcomes in HIV-Infected Patients Age 50 and Older
HIV patients 50 or older who took more than 10 medications had a lower CD4 count, higher cardiovascular disease (CVD) rate, more adverse drug effects, and more drug-drug interactions than older people taking fewer medications [1]...A lower proportion taking more than 10 drugs tended to have an undetectable HIV load in this 100-person comparison.....http://www.natap.org/2016/IDSA/IDSA_08.htm
Italy: 50% frail now, 50% > 50 Years Old Projected to Increase a Lot.....Frailty / Aging Projections in Italy - Future challenges for clinical care of an ageing population infected with HIV: a "geriatric -HIV" modelling study .....Frailty 50% Now, Predicted to be 75% in Older Aging HIV in 14 years, requiring a large number of patients, perhaps 40%, to be confined in old age homes because they will not be able to function
Chicago Aging Cohort: Many aging HIV+ patients live alone, and the interplay of co-morbidities, poly-pharmacy, memory issues, and falls places them at an increased risk for non-independent living at an earlier age than the general population......median age stood at 56 years.....40% reported mental health is a concern...42% reported a history of depression.....One third reported memory problems or concerns, and 27% reported one or more falls in the past 12 months.....46%, lived alone.....54% took four or more prescription medicines daily".....IDSA: Assessing the needs of older HIV+ adults; Initial data from the CORE Healthy Aging Initiative (CHAI) - Money, Mental Health, Housing Top List of Concerns in Older HIV+ Chicago Group
Comorbidities Increased in Netherlands....Future challenges for clinical care of an ageing population infected with HIV
....As a result of the ageing HIV-infected population, the number of HIV-infected patients in the Netherlands with at least one NCD [comorbidity / "aging related non-communicable diseases] is projected to increase from 29% in 2010 to 84% in 2030.....The number of patients with three or more NCDs is expected to increase from 0·3% in 2010 to 28% of patients in clinical care in 2030. In 2030, only 16% of HIV-infected patients will not have any of the NCDs investigated"
GLASGOW: Proportion of US HIV Patients With 3 or More Comorbidities Will Rise 4-Fold by 2035
EuroSIDA - Doubling of Some Comorbidities - GLASGOW: Rates of All Age-Related Comorbidities Rise in EuroSIDA From 2006 to 2014
.....The proportion of people 50 or older rose from 25.2% in 2006 to 44.0% in 2014....."There was an increase of 5.0% of patients in renal DAD high risk group. This is particularly observed for patients ≥50 years which increased from 24.3% in 2006 to 36.9% in 2014, in the high risk group.....proportions with a high or very high D:A:D CVD risk score climbed both overall (5.8%, from 9.5% to 15.3%) and in the 50-and-older group (2.5%, from 28.9% to 31.4%)......CKD prevalence increased 3.1% (from 2.0% to 5.1%) overall and 5.6% (from 3.9% to 9.5%) in people 50 or older.....Hypertension had the greatest prevalence gains, rising 15.2% (from 25.4% to 40.6%) overall from 2006 to 2014 and 13.7% (from 48.2% to 61.9%) in people 50 or older
GLASGOW: Doubled & Tripled Rates of Comorbidities France - Prevalence of All Comorbidities Up From 2004 to 2014 in Big French Cohort.....Aquitaine, observational cohort study, southwestern France......2138 people - proportions with a high renal risk score soared from 29.9% to 50.7%.....current alcohol abuse from 3.1% to 14.3%.....hypertension from 18.8% to 56.3%..... Proportions with a 5% to 10% D:A:D coronary heart disease risk index doubled from 13.1% to 26.5%, and proportions with a D:A:D index above 10% quadrupled from 5.3% to 19.9% .....The Aquitaine team proposed that "careful HIV management, including regular monitoring and screening of the major comorbidities
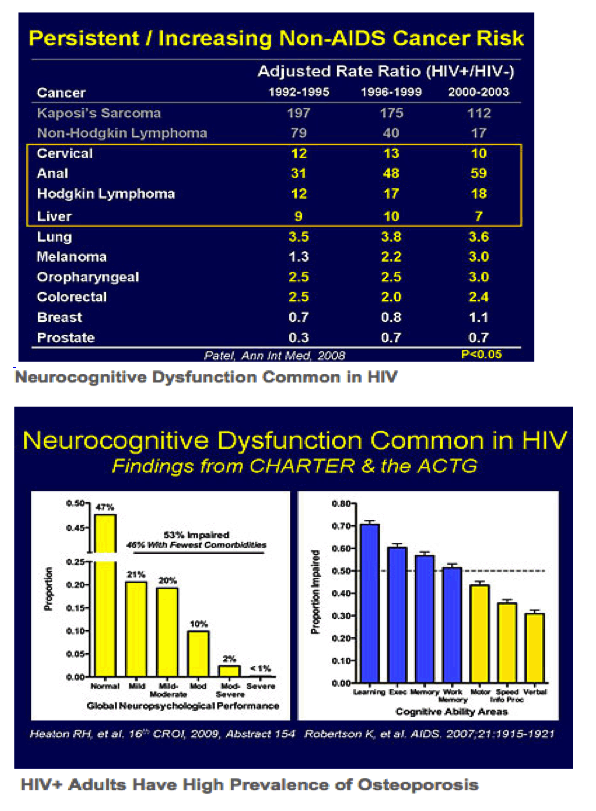
Anal cancer incidence is on the rise among US HIV-positive MSM, with rates as much as 37-fold higher than the in the general population [2].....Among 8514 HIV-positive MSM studied, 914 (11%) had an anal pap test in the past 12 months during 2009-2012. Compared with white men, non-Hispanic blacks had a significantly lower pap testing rate (7% versus 13%, P < 0.0001).
Increased Anal Cancer in HIV+ MSM - IDSA: Should Anal Cancer Screening Get More Aggressive for Some MSM With HIV? - HPV-related disease in HIV-infected MSM with and without recent HCV
IDSA: Depression and HIV Infection are Associated with Higher Risks of All-Cause Mortality in U.S. Veterans - Depression Adds to Mortality Risk With HIV in Large US Veterans Cohort
Increased risk of infection-related malignancies (IRMs) and infection-unrelated malignancies (IURMs) The incidences of both IURMs and IRMs increased with older age. It was projected that the incidence of IRMs would decrease by 29% over a 5-year period from 3.1 (95% CI 1.5-5.9) per 1000 person-years in 2011, whereas the IURM incidence would increase by 44% from 4.1 (95% CI 2.2-7.2) per 1000 person-years over the same period.......these findings suggest the need for targeted preventive measures and evaluation of the cost-benefit of screening for IURMs in HIV-infected populations......IURMs should therefore be a priority in the coming years as higher proportions of HIV-positive people live past 50, 60 and 70 years......The most common IRMs were non-Hodgkin lymphoma (n = 116), anal cancer (85), Kaposi sarcoma (62) and Hodgkin lymphoma (43). Lung (n = 55), prostate (28), colorectal (23) and breast (22) cancers were common IURMs.....Older age was the largest contributor to IURM incidence. Our finding of a twofold higher IURM incidence for a 10-year increase in age is similar to findings of the The Strategies for Management of Antiretroviral Therapy (SMART) study [24] and to data published online by the European Cancer Observatory, which showed a 1.9-fold increase in the incidence of all malignancies in the general population [23]. The effects of aging, including reduced immune function, are thought to be accelerated in HIV-positive populations and may also contribute to an increased IURM incidence [22].
The IURM incidence was 7.33-fold (95% CI 4.07, 13.21; P < 0.01) and 2.37-fold (95% CI 1.31, 4.27; P < 0.01) higher in those aged ≥ 51 years and aged 41-50 years compared with those aged 36-40 years (Table 3), and explained 56% and 17% of excess IURMs within the cohort, respectively. This corresponds to a twofold increase in IURM incidence per 10 years older age (aRR 2.07; 95% CI 1.84, 2.32). Current smoking was associated with elevated IURM incidence and explained 16% of IURMs overall. Stratifying by age, IURMs were elevated in current smokers relative to nonsmokers in those aged ≥ 50 years (aRR 1.75; 95% CI 1.23, 4.49; P < 0.01; Fig. 1b), but not in those aged < 50 years (aRR 1.12; 95% CI 0.71, 1.77; P = 0.51), although the P-value of the interaction term was nonsignificant (P = 0.32). Current smoking was not associated with IURM incidence after the exclusion of lung cancers. A low current CD4 count was associated with a higher IURM incidence (CD4 count < 200 cells/μL: aRR 1.99; 95% CI 1.26, 3.17; P < 0.01, relative to CD4 count > 500 cells/μL). Despite this, the overall excess of IURMs attributable to a CD4 count < 200 cells/μL (6%) was small. The association between higher IURM incidence and low CD4 count was evident in those aged < 50 years (aRR 2.52; 95% CI 1.40, 4.54; P = 0.01; Fig. 1a), but not in those aged ≥ 50 years (aRR 1.14; 95% CI 0.62, 2.12; P = 0.56; Fig. 1a), although the P-value of the interaction term did not reach statistical significance (P = 0.09). Prior HBV coinfection was also associated with higher IURM incidence (aRR 1.73; 95% CI 1.17, 2.55; P < 0.01), but only 5% were attributable to HBV coinfection within the cohort (Table 3).
|
|
| |
| |
|
|
|